Literature and clinical experience give multislice CT angiography (CTA) high marks for diagnosing traumatic injury to the carotid and vertebral arteries. And like all CT exams, image quality is soaring on wings of thin slices and fast scanners.
Unfortunately, excellent image quality isn't enough to predict complications and manage patients optimally, particularly those who present with few or no neurological symptoms. New markers and tests may eventually improve the ability to predict complications and outcomes. But for now, careful attention to the clinical and imaging data is the best hope.
Speaking at Stanford University's 2006 International Symposium on Multidetector-Row CT in San Francisco, Dr. Jay Cinnamon talked about his CTA technique and the quandary of diagnosis and management. Cinnamon is a radiologist specializing in neurovascular imaging at Quantum Radiology in Marietta, GA.
The incidence of vascular injury resulting from blunt trauma ranges from 0.1% to 0.7%, and for penetrating trauma to the neck it's higher, he said. But complications and outcomes are a big question mark.
"There are some data out there, but if you really dive into it, it's not very good data," Cinnamon said. "Even if you diagnose, nobody knows the complication rate or the risk of a future event. So if you presume a blunt trauma vascular injury rate of 0.1% and you have 10,000 blunt trauma patients, that leaves you 100 patients who have vascular injuries. How many of those 100 will go on to stroke next week, next month, next three months, or next year? Nobody really knows for sure."
Potential complications include dissection, occlusion, pseudoaneurysm, rupture, arteriovenous (AV) fistulas, arterial laceration, and occlusion. Injuries are not necessarily limited to the trauma site; a patient with blunt trauma to the left side of the neck could well have a right subclavian artery traumatic injury, he said. And although outcomes are hard to predict, finding the injury is key.
"In the setting of blunt trauma you want to consider everything from the aortic arch all the way up to and potentially even through the head, because intracranial dissections and pseudoaneurysms occur as well," Cinnamon said. There are many treatment options as well, including surgical ligation to endovascular occlusions, stenting, anticoagulation therapy, antiplatelet therapy, or doing nothing at all, he added.
The algorithmic approach to diagnosis and patient management is controversial and poorly defined, he said. The premise is that making a diagnosis will help the patient. But without knowing the real incidence of arterial injury, particularly in brain trauma, and considering all the treatment variables, diagnosis won't necessarily impact positively on the outcome.
One woman, for example, was admitted with a gunshot wound to the neck, Cinnamon said. CT showed a bullet fragment and a completely occluded internal carotid artery, but the patient was completely asymptomatic. Five days later she came down from the hospital ward with right hemiparesis and aphasia. There were multiple infarctions in the region of the left middle cerebral artery, and repeat angiography showed a clot within the recanalizing left internal carotid artery that was sending off emboli into the intracranial circulation.
"So we really don't know incidence of traumatic vascular injury in the setting of trauma," he said. "We know it's not as common in blunt trauma as it is in penetrating trauma, but we don't have a good handle on the incidence. We don't really don't know who should be screened, we don't know the clinical significance once we make a diagnosis, we don't really know the complication rate in terms of how many patients go on to neurological deficit. We don't know how to treat and for what period of time, but other than that we know everything there is to know about vascular injury."
Future research may provide answers, Cinnamon noted in an abstract. Might there be risk factors that raise the index of suspicion of traumatic vascular injury, such as Horner's syndrome, cervical spine fracture, and mechanism of injury? Should patients be evaluated with catheter angiography, CTA, MRI, or ultrasound? When should patients be examined to optimize outcomes? Immediately, the next day, or sometime during their hospital stay?
What's clear is that CTA is good and getting better. In recent years, clinical experience and several studies have demonstrated the modality's accuracy in evaluating neurovascular trauma. Among them, Cinnamon said, Dr. Diego Núñez Jr. and colleagues from the Yale University School of Medicine in New Haven, CT, provided an excellent compendium of trauma knowledge (Radiographics, July-August 2004, Vol. 24:4, pp. 1087-1098; discussion 1099-100).
Just this month, Núñez and his colleague Dr. Turgut Berkmen published a paper on blunt neurovascular trauma. Readily available, accurate, and easy to perform, CTA is increasingly valuable for screening, as angiography is shifting to a therapeutic role, they wrote (European Journal of Radiology, September 2006, Vol. 59:3, pp. 317-326).
"The applicability and practicality of angiography as the screening method of choice for blunt cervical vascular injuries have been challenged in recent years," Núñez and Berkman wrote. "MR and duplex sonography have potential advantages as noninvasive screening techniques, but also have limiting shortcomings. MR is not universally available in the acute trauma setting, and MR scanners limit the accommodation of monitoring devices and (ventilation) equipment often needed in trauma patients. In addition, reported sensitivity has been low, particularly if performed with flow-dependent time-of-flight technique. DUS has also been tested but is very operator-dependent and limited accuracy is found for diagnosing lesions near the skull base...."
Meanwhile, advances in endovascular devices have enabled new endovascular treatment options for lesions that were traditionally difficult or impossible to manage nonsurgically, creating new therapeutic options for angiography.
On the diagnostic side, the evolution of CTA techniques has enhanced CT's clinical utility, Cinnamon said in his presentation. At his facility, multidetector-row CT (MDCT) is commonly acquired from the aortic arch up to the skull base and higher, he said, and slice thicknesses have been reduced from 3 mm to submillimeter-thick slices. Contrast is being used more efficiently and the CT radiation dose has been lowered.
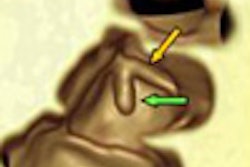
"In our experience, the diagnosis of traumatic vascular injury has been primarily made on axial images, no different than what we would do in looking for traumatic injury in any other blood vessel, abdominal aorta, or thoracic aorta," he said. "We're looking for intimal flaps, we're looking for irregularities of the contour of the vessel, we're looking for extravasation, we're looking for pseudoaneurysms. We use axial images to scroll up and down looking for these irregularities."
Multiplanar reconstructions (MPRs) can be helpful, but most of the time the actual diagnosis is made on axial images, Cinnamon said. MPRs are useful for demonstrating injuries to clinicians and surgeons -- for example, for depicting the relationship of a vessel injury to surrounding structures such as the skull base or temporal bone. And MPRs can be necessary to demarcate the relationship of pseudoaneurysms to surrounding vessels, he said.
The seat-belt sign is controversial, he said. Marks from an automobile seat belt on the trauma patient's neck or torso are markers for vascular injury, though the relationship is poorly understood and literature on the subject is poor.
In addition, skull-base fractures signal a higher risk of arterial injury, Cinnamon said. But once again the value of the information for patient management is questionable.
Even if the patient is symptomatic, with a traumatic carotid artery injury diagnosed from a skull-base fracture, what is the clinical significance of the finding? Trauma patients often have altered mental status and neurological symptoms, Cinnamon said. And what part of the patient's symptoms are related to the vascular trauma rather than axonal injury or some other cause? The answer is unknown.
"CTA is an evolving tool that's fast and accurate," Cinnamon concluded. "The key diagnosis in our experience has generally been made on axial and transverse images. We don't know much about natural course and the natural history. Evaluation is tailored to clinical decision-making and not necessarily to the clinical outcome."
By Eric Barnes
AuntMinnie.com staff writer
October 16, 2006
Related Reading
3D penetrates trauma imaging niche, August 24, 2006
CT mostly outperforms alternatives in penetrating trauma, February 20, 2006
CT is the blanket modality for neuroimaging blunt injury patients, January 12, 2006
MDCT spurs boom in ER CT utilization, January 4, 2006
When x-ray finds cervical spine injuries, CT picks up more, September 14, 2005
Copyright © 2006 AuntMinnie.com