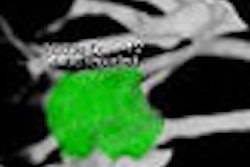
Virtual colonoscopy has shown that it can reliably detect significant lesions of the colon and rectum. Unfortunately, some researchers have also noted a certain susceptibility to failure, relative to conventional colonoscopy, when VC is performed poorly.
Two recent editorials contemplate the myriad details that constitute a virtual colonoscopy protocol, and the ways in which minor differences in methodology can affect results in major ways. In the April Radiology online, Dr. Joseph Ferrucci discusses what we have learned about technique that can inform future studies.
In a Current Opinion in Gastroenterology review article, Dr. Joel Fletcher and colleagues from the Mayo Clinic in Rochester, MN, examine the technical differences separating the major trials, some key factors affecting interpretation, and the limitations of VC with respect to polyp size.
Although a detailed examination of those factors is beyond the scope of this article, some major points from each editorial are included. The good news is that a rising tide of technological improvements, especially in the form of computer-aided detection and better CT scanners, will surely lift all study results. The bad news is that with so many factors potentially affecting outcomes, a certain amount of speculation with regard to the influence of each individual factor cannot be avoided.
"CT colonography (alternately CTC or VC) is a technically demanding imaging technique in which the elements of success are multifactorial, that is, the devil is in the details," wrote Dr. Joseph Ferrucci in his editorial. "Striking success was reported for the first and much larger study by Pickhardt et al (New England Journal of Medicine, December 4, 2003, Vol. 349:23, pp. 2191-2200), and CT colonography was widely heralded as a major clinical advance. Findings in the report by Cotton et al published five months later (Journal of the American Medical Association, April 14, 2004, Vol. 291:14, pp. 1713-1719), however, indicated that the performance of CT colonography was relatively poor" (Radiology 2005, Vol. 235, pp. 13-16).
"While there are several clinical indications for CT colonography, the recent disparate results of large screening studies have created controversy regarding the technique," Fletcher et al wrote in their review. "Clinical studies can be difficult to compare because of the rapid evolution of technology, particularly relating to technical advances in CT and postprocessing computer software, and the large number of variables comprising the component parts of the CT colonography examination. Our purpose is to delineate differences between published clinical studies, in an effort to understand implications for gastroenterologists and radiologists incorporating this new technology into their medical practice" (Current Opinion in Gastroenterology, January 2005, Vol. 21:1, pp. 90-98).
Technique
Technical factors influence the conspicuity of polyps, Fletcher's group noted. Among them, mechanical insufflation of the bowel appears to be a promising method for obtaining more reliable distension with fewer collapsed segments (American Journal of Roentgenology 2004, Vol. 183: 4 suppl., pp. 76). (A recent presentation at RSNA 2004 found similar results.)
"Labeling with a high-attenuation oral agent will make polyps conspicuous if they are submerged underneath fluid or lie adjacent to stool," Fletcher and colleagues wrote. "More importantly, labeling stool may increase specificity, as adherent stool is the most common cause of false-positive examinations at CT colonography.... We systematically examined the use of labeling colonic fluid and found no benefit" (Radiology, September 2000, Vol. 216:3, pp. 704-711).
Nevertheless, the relatively wide 5-mm slice thicknesses used in the early study may have hampered detection, Fletcher's group wrote. More recently, Pickhardt's more advanced 3D review system was able to subtract high-attenuation labeled stool, though the long-term benefit of tagging remains doubtful, Fletcher et al stated.
With regard to slice thickness, several studies have failed to show a connection between thinner slices and the detection of clinically significant polyps, although specificity has improved with thinner slices in other cases, Fletcher's group wrote. However, they added, in a 2003 study by Taylor et al using an explanted human colon, reducing slice thickness from 2.5 mm to 1.25 mm significantly improved the detection of 1-cm polyps (Radiology, October 2003, Vol. 229:1, pp. 109-118).
Interpretation
Pickhardt and colleagues relied on a 3D primary interpretation system, while Cotton et al read 2D images first, with 3D follow-up for some images, and segmental unblinding of virtual colonoscopy results, Fletcher's group noted. But the Fletcher paper cautioned against concluding from this experience that 3D primary interpretation is inherently superior, noting that studies have shown mixed results.
"The truth is likely that some polyps are better seen on two-dimensional images, while others are better seen on three-dimensional images," Fletcher et al wrote. "Reading strategies that employ both two- and three-dimensional reading are likely to result in the detection of more polyps than either method alone."
In his paper, Ferrucci listed factors other than primary interpretation method that may have worked against the Cotton team, notably its use of older scanner technology and slice thicknesses, as well as older image visualization software.
"To what extent the older technology affected the performance of CT colonography in the study of Cotton et al is unclear, but it probably did not help," Ferrucci wrote. Second, he said, there was no documentation of the adequacy of preprocedural colon cleansing or air insufflation, key elements of proper CT colonographic technique. Third, no fecal tagging was used. Fourth, underestimation of the steep learning curve for CT colonography was also evident." The single VC site in the Cotton trial with a sufficient number of patients (n = 184) for the researchers to train on had results comparable to the Pickhardt group, Ferrucci noted.
"Unfortunately," Fletcher and colleagues wrote, "additional training may not ensure better performance, as variability between the radiologists with extensive experience has been demonstrated" (European Radiology, June 2004, Vol. 14:6, pp. 1025-1033).
As for VC's limitations in detecting tiny polyps, multiple studies have shown that the risk of invasive cancers in polyps 5-9 mm in size is a minuscule 0.5% to 1.3%, and the risk of high-grade dysplasia is 2% to 6%. "We have adopted a policy of not reporting or commenting on lesions 5-mm or smaller in size," Fletcher's team noted.
Moreover, the 1-cm lesion cutoff size many practices use to triage VC patients into conventional colonoscopy may not endure. Pickhardt et al, for example, chose an 8-mm lesion-size cutoff for their multisite study, and in a JAMA editorial accompanying the Cotton study, Dr. David Ransohoff from the University of North Carolina in Chapel Hill also suggested the possibility of reduced target threshold size, Ferrucci noted.
"The many diminutive non-neoplastic polyps or lesions now so often found and removed at colonoscopy pose no patient threat but add substantial system costs," Ferrucci wrote. "Even the threat posed to the patient by small adenomas has been challenged. Hence, some utilization patterns of colonoscopy in clinical practice recently have been described as excessive, inappropriate, and unnecessary" (Annals of Internal Medicine, August 17, 2004, Vol. 141:4, pp. 264-271).
More VC indications ahead
Virtual colonoscopy's discrepant results in screening studies "may be due to different patient populations studied, technical factors, and interobserver variability," Fletcher et al concluded in their editorial. "At present, CT colonography outperforms other noncolonoscopic approaches to neoplasm detection. Current indications for (VC) include incomplete endoscopy and screening in persons at risk or averse to colonoscopy. Technical innovations should lead to improvements in the quality of the (VC) dataset, accuracy of interpretation, and patient acceptance. When such advances reproducibly yield high accuracy, widespread use ... for colorectal cancer screening may be acceptable."
Better preps, better CT images, and computer-aided detection schemes are rapidly improving VC's accuracy, Ferrucci wrote, and performance-quality issues are being addressed by the Reston, VA-based American College of Radiology, which is developing a practice standard, and by the Working Group for Virtual Colonoscopy, which is drafting consensus standards, reporting schema, and training guidelines, he noted.
"For patients who are unwilling or unable to undergo optical colonoscopy, (VC) is a 'compliance enhancer,'" Ferrucci concluded. "Hospital industry data suggest that as many as 60% of patients who undergo CT colonography have never had any previous colorectal screening. In many areas of the country, colonoscopy volume outstrips manpower resources, with several months of patient appointment waiting times. Prescreening with CT colonography to select the relatively few patients with large adenomas for referral to colonoscopic polypectomy should produce better use of colonoscopic resources...."
By Eric Barnes
AuntMinnie.com staff writer
April 20, 2005
Related Reading
Internal medicine doc finesses colon cancer screening guidelines, April 18, 2005
Senate hears testimony on virtual colonoscopy, March 28, 2005
VC with contrast finds more extracolonic trouble, April 11, 2005
Multicenter VC trial begins with high hopes, state-of-the-art protocol, March 1, 2005
Duke VC trial results disappointing, November 1, 2004
Colonoscopy performed too often after polypectomy, August 17, 2004
Group credits 3D reading for best-ever VC results, October 15, 2003
Copyright © 2005 AuntMinnie.com