Computer-aided detection found most of the polyps in a reduced-prep virtual colonoscopy protocol, a new study concludes. On the other hand, the technique produced too many false-positives when barium fecal tagging was incomplete, which was often.
Based on studies showing bowel prep to be the most uncomfortable part of both virtual and conventional colonoscopy, much of today's VC research is focused on finding ways to eliminate cathartic cleansing while keeping diagnostic accuracy high -- a lofty goal that some doubt will be achieved anytime soon. But if radiologists succeed, they may be able to attract more people to colorectal cancer screening by making it easier to endure.
To this end, Dr. Hiro Yoshida and colleagues from the University of Chicago set out to evaluate their CAD's system performance in a minimal-prep cohort -- not to assess the adequacy of the fecal tagging, Yoshida explained in a presentation at the RSNA meeting earlier this month in Chicago. But the tagging, or rather the lack of it, turned out to be a key factor in the CAD system's performance.
Making the CAD algorithm more robust, optimizing the tagging regimen, and even digitally subtracting the fecal material might be required to get the process right.
"The purpose of our study was to assess the performance of CAD for polyp detection in patients who received dietary fecal tagging," Yoshida said.
The retrospective study examined data from 60 patients (mean age 67) who had undergone both virtual and conventional colonoscopy under the care of Dr. Philipe LeFere and colleagues at the Stedelijk Ziekenhuis in Roeselare, Belgium. The subjects received 50 mL of 40% w/v barium suspension with the meals.
A day before imaging, the subjects were given a reduced bowel cleansing regimen consisting of 16.4 g of magnesium citrate and four bisacodyl tablets. (The regimen may not have been all that comfortable, LeFere acknowledged after Yoshida's presentation, rating the technique a 6 on a discomfort scale of 1 to 10.)
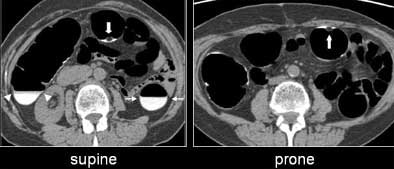 |
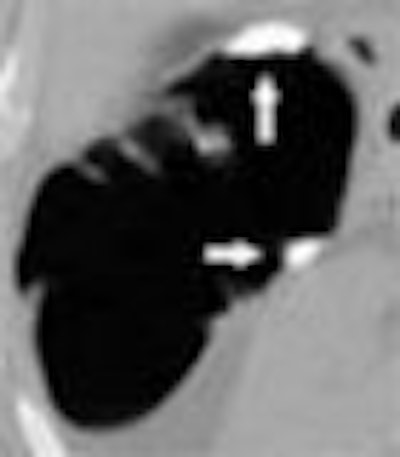
| Untagged stool can be seen floating in a small pool of barium (large white arrow, right and left). Well-tagged fluid in the descending (small white arrows) and the ascending (white arrowheads) colon. All images courtesy of Dr. Hiro Yoshida. |
The researchers' CAD scheme, which has been described previously, first segments the colon, then looks for candidate lesions based on their likely geometric features. An additional filter reviews all the polyp candidate lesions and eliminates likely false-positives.
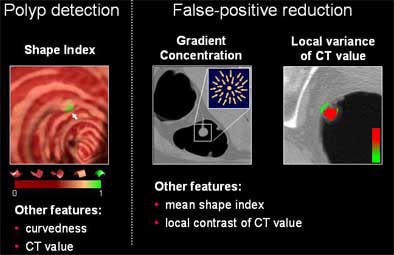 |
| The CAD scheme relies on volumetric features in the CT dataset to select polyp candidates. |
"By combining all these features, the system finally comes up with the set of CAD-detected polyps," Yoshida said.
Before tackling the minimum-prep dataset, the group's CAD scheme was trained to find polyps in data from 121 virtual colonoscopy patients who had undergone standard cathartic preparation VC, with room-air colonic insufflation. This group had 42 polyps larger than 5 mm in 28 patients. There were 22 polyps 5-10 mm and 20 polyps larger than 10 mm in the study, which used single- and multidetector-row CT with collimation of 2.5-5.0 mm, reconstruction intervals of 1-5 mm, pitch 1-2, 60-100 mAs, and 120 kVp, Yoshida said.
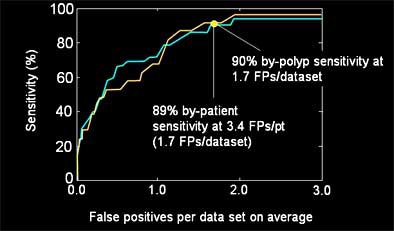 |
| Before assessing the minimal-prep cohort, the CAD system was "trained" on 121 patients (242 data sets) with 42 polyps larger than 5 mm. All the patients had undergone a conventional bowel-cleansing regimen. The results from this dataset, including a low number of false-positives, can be seen in the chart. |
The reduced-prep patients that CAD would be directed to assess after training had a slightly different protocol: CT colonography (VC) on a single or multidetector-row CT scanner with collimation from 2-5 mm, reconstruction interval of 2 mm, pitch 1.25, 70 mAs, and 120 kVp, following manual CO2 insufflation. To exclude tagged stool from the calculation of polyp candidates, the CAD scheme designated regions with 150 HU or greater as tagged stool.
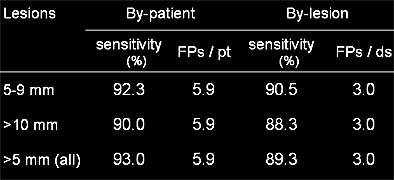 |
| In the minimal-prep study, CAD yielded high sensitivity, but with a relatively large number of false positives. |
"Then we applied the CAD system to the dietary fecal tagging patients," Yoshida said. "Tagged regions were excluded from feature calculations.... The results show that CAD yielded high sensitivity with relatively low rate of false-positive detections. By patient and by lesion, sensitivity stays around 90%. However, false-positives by patient as well as false-positives by dataset almost doubled."
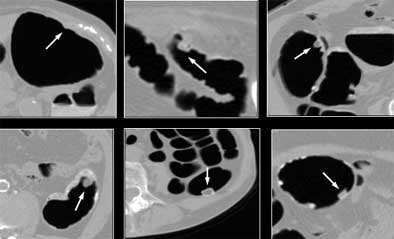 |
| The presence of untagged or partially tagged stool in images above led to false-positive results with CAD. |
"There were some cases that were partially covered by stool, which were unfortunately missed by CAD," he said. In fact, untagged or partially tagged stool was the principle cause of false-positives (40%), followed closely by haustral folds (39.3%), nonspecific findings (4.1%), stomach or small bowel (4.1%), ileocecal valve (4.1%), extrinsic compression (0.7%), rectal tube (0.1%), and other findings (6.2%) the CAD scheme took as polyps, and which the radiologist would presumably eliminate upon inspection of the CAD results, according to Yoshida.
"CAD trained on a cleansed colon can yield a high sensitivity in the detection of polyps in CTC after dietary fecal tagging with barium," he concluded. "However, CAD may produce a relatively large number of false-positives due to inhomogeneously tagged stool."
Further research is needed to improve both the homogeneity of tagged stool and CAD's ability to detect untagged or partially tagged stool, Yoshida said.
Digital subtraction technology, still in early development, has also been suggested as a partial solution, though the technology could potentially introduce errors of its own.
By Eric Barnes
AuntMinnie.com staff writer
December 23, 2004
Related Reading
Mass appeal: VC CAD doesn't stop at polyps, October 10, 2003
Knowledge-guided segmentation improves polyp detection, October 18, 2002
Virtual colonoscopy: 2-D vs. 3-D primary read, June 3, 2002
Prepless virtual colonoscopy shows early promise, June 3, 2002
New CAD technique improves CT colonography, December 21, 2001
Copyright © 2004 AuntMinnie.com




















