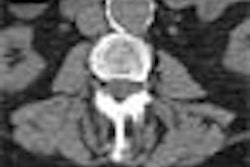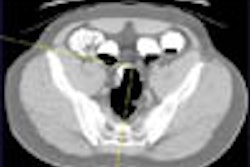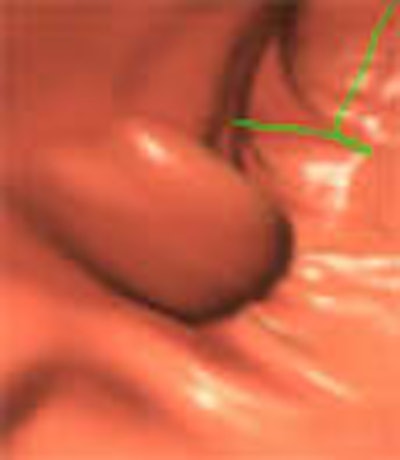
In the battle between 2-D and 3-D reading of virtual colonoscopy data, the winner won't ever take all. That's because both methods are essential, and each is needed to solve problems in the other. At the least, 2-D and 3-D will both be needed until some future CAD or novel-view system proves itself superior.
At the International Symposium of Virtual Colonoscopy in Boston, Dr. Abraham Dachman from the University of Chicago promoted the primary 2-D read, while Dr. Mark Wax from the State University of New York at Stony Brook spoke in favor of 3-D.
To begin, the 2-D primary read was defined as axial images with multiplanar reconstructions, and 3-D as the endoluminal view or "fly-through" method. Novel views, such as virtual dissection schemes, weren't included.
Dachman reeled off 2-D's advantages as he saw them: speed, ease of interpretation, and accuracy of polyp-size measurements. Secondary advantages include smaller data storage requirements, easier export of images, and better documentation of lesion location.
Successful 2-D reading requires the radiologist to "mentally reconstruct" the dataset into a 3-D image while scrolling through it, Dachman said.
"I think all of us have the ability to do that, some of us more so than others, but I think it's critical for differentiating folds versus polyps versus pseudotumors," he said. Dachman's group performs 2-D primary reads with 3-D problem solving in about 10 minutes, with a range of 7-30 minutes.
"Sometimes you want to spend a little time on a case," Dachman said. You may still need to read a case in both lung windows and soft-tissue windows (to look for wall thickening, extracolonic findings, etc.), he said. Diverticular disease can easily be problem-solved in 3-D. "Whichever way you do it, 2-D may require 3-D problem solving, but 3-D will also require 2-D problem solving."
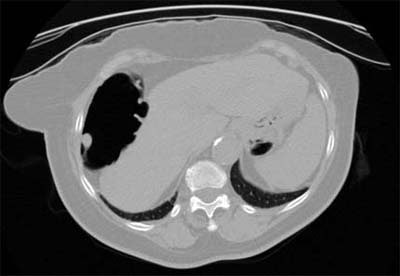 |
| Axial 2-D CT image showing a 12-mm pedunculated polyp in the hepatic flexure. Image courtesy of Dr. Abraham Dachman, University of Chicago. |
Among a handful of trials to compare the two approaches, a study in 2000 by Macari and colleagues used two methods and compared interpretation times. The first method involved the evaluation of a 2-D dataset in cine mode at a workstation, using multiplanar reconstructions (MPR) for problem-solving only. The second method began with the first technique, adding 3-D fly-through endoluminal navigation and multiplanar reformatted images. Mean evaluation time was 16 minutes for method 1, and 40 minutes for method 2, which detected no additional polyps (AJR, June 2000; Vol. 174:6, pp. 1543-1549).
Still, it's difficult to draw conclusions from the studies due to important differences in the methods and equipment, experience, and individual patients, Dachman said.
"Reader experience is important," he said. As for user software preferences, there are a variety of different platforms featuring 2-D and 3-D, and individual users may find wide variations in their relative speed and ease of use. One essential feature is the ability to switch rapidly between 2-D and 3-D, and good patient prep facilitates interpretation in both methods. Two-dimensional viewing is also generally better for navigation accuracy and size measurement, he said.
Using 2-D for primary reading, 3-D problem-solving is needed only about half the time, he said. Adding 3-D increased reading time by about 26 minutes. Axial images show 100% of the mucosa, but 3-D can't ever claim that, he said.
"I will take the opportunity to make a crystal ball comment," Dachman said. "The best answer may turn out to be something like a novel view, neither classic 3-D nor 2-D, combined with computer-aided diagnosis. I think the actual answer will be driven by market forces as much as by good science."
The case for 3-D
"The real advantage to a 3-D approach has to do with real-time volume rendering, in which we're developing these images live, not just moving backwards and forwards, but really interactive with an endoscopic view," Wax said.
A principal of virtual colonoscopy workstation developer Viatronix of Stony Brook, NY, Wax demonstrated the concepts of 3-D reading on the firm's V3D Colon workstation. Earlier studies need to be redone, he said, since they compared 2-D to 3-D using prototype 3-D systems that were cumbersome, limited, and time-consuming.
Some studies did show certain advantages to the 3-D approach, Wax said. For example, a 1999 study in Radiology compared polyp visualization in three display modes for CT colonography, including 2-D, 3-D endoscopic movies, and a 3-D view called panoramic endoscopy, which provides some of the navigation capabilities of current workstations.
The 3-D methods had higher overall sensitivity than axial CT, up to 85% vs. 68%, respectively. The authors concluded that higher sensitivities for three-dimensional displays may justify the additional computation and review time (Radiology, July 1999, Vol. 212:1, pp. 203-212).
Still, the newer 3-D workstations go beyond looking at the colon reconstruction in movies that are limited to retrograde and antegrade movement through the colonic lumen. Guided fly-throughs enable the reader to start and stop, turn in any direction, mark and measure the colonic surface, and look behind haustral folds.

Click here to see the video (produced for high-speed connections)
"We talk about colonoscopy as a gold standard, but it's not really a good standard because gastroenterologists never really turn around and see the back ends of these folds," Wax said. "We're able to see all significant areas of the colon."
The V3D system features a technique called electronic cleansing, an advanced digital subtraction method that also maintains the partial-volume effect. Another feature automatically "paints" areas of the colon that have not yet been examined in the endoluminal view, enabling the radiologist to review the areas of the lumen that were missed. After the initial fly-though, the radiologist can then return to examine previously unseen patches until further review makes them all disappear, Wax said.
"We can sort these areas by size, you can step through them to look at the colon," he said. As smaller and smaller patches are reviewed, the chance of missing significant polyps is greatly reduced, he said.
Another V3D feature, called translucent volume rendering, is used to differentiate polyp from stool by enabling visualization of different densities that occur within stool but not polyps. Also, current 3-D systems enable prone and supine images to be viewed side by side, for easier differentiation of polyps from stool that moves, he said.
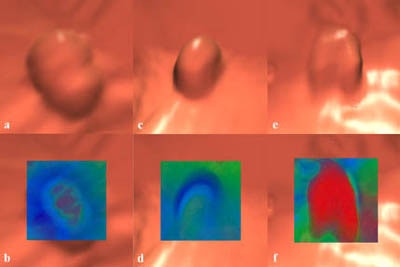 |
| Use of the translucent rendering mode applied to the endoscopic views is shown on the top images. An adenoma (b) has a gradual change in density towards the center shown by the color change from blue to green to red. A hyperplastic polyp (d) has uniform blue colors similar to the mucosa and colonic folds. A stool ball with barium (f) has dark red, indicating high density, extending to the surface. Images and movie courtesy of Dr. Mark Wax and Viatronix. |
The Viatronix system can switch from 2-D to 3-D view, and fly through the data using an automated lumen centerline. And the important job of measuring polyps is more straightforward in 3-D, he said; in the V3D system it's a drag-and-click process.
"The system can ensure evaluation of all mucosal areas, especially around haustral folds and sharp turns," Wax said.
Following the presentations, audience questions came back to the subject of how much mucosal surface is actually seen in 3-D endoscopic reconstructions. While the theoretical answer may be 100%, the realistic answer is probably lower, Dachman said.
As a result, a frank cancer located in an unexamined mucosal area could be missed on 3-D, he said, while the so-called "pixel stripping" effect could result in underreporting of polyp size. Both are potential liability issues.
Wax responded that the painting feature on V3D ensures that 100% of the mucosa can be easily examined. Still, Dachman said that in the 3-D systems he has used, examining 100% of the mucosa would be prohibitively time-consuming.
By Eric BarnesAuntMinnie.com staff writer
June 3, 2002
Copyright © 2002 AuntMinnie.com