Respiratory Distress Syndrome/Surfactant Deficiency Disorder/Hyaline Membrane Disease:
View cases of respiratory distress syndrome
Clinical:
Respiratory distress syndrome (RDS)/surfactant deficiency syndrome (SDD) is the result of surfactant deficiency in the newborn. Surfactant is a lipoprotein produced by Type II pneumocytes that reduces the surface tension of alveoli, permits normal expansion of the lungs during respiration, and functions to prevent alveolar collapse [2]. Surfactant production does not mature until approximately 35 weeks gestation [2]. A L/S ratio greater than 2.0 indicates fetal lung maturity. The condition typically presents within 2 hours of birth with retractions, cyanosis, expiratory grunting, nasal flaring, and tachypnea. Pathologically the condition is characterized by acinar atelectasis, dilatation of the terminal bronchioles, and deposition of a hyaline membrane (proteinaceous exudate from necrotic cells).The greatest risk factor for SDD is prematurity [2]. The frequency of SDD is 60-80% in children born before 28 weeks and 15-30% in children born between 32-36 weeks [2]. Other authors report there is a 66% incidence in infants less than 27 weeks (or less than 1000 grams) and only a 1% incidence in infants at 36 weeks (or greater than 2500 grams). SDD is rare after 36 weeks, but can occur in the setting of maternal diabetes because of high insulin levels which interfere with surfactant production maturation [2]. Other risk factors include multiple gestations, c-section delivery, and perinatal asphyxia [2].
Some feel that a normal CXR at 6 hours virtually rules out RDS. Differential considerations include: neonatal pneumonia, pulmonary hemorrhage, wet lung/transient trachypnea of the newborn (although there is typically normal or hyperaeration in these cases), and CHF. RDS may be complicated by reopening of the ductus arteriosus which is characterized by sudden clinical deterioration at about 7 days, increased oxygen requirement, and a cardiac murmur. An indication that the ductus has reopened is that the granular pattern of RDS on CXR becomes more opaque (complete white-out of the lungs) and there are signs of CHF (enlarged heart, effusions). Other complications include pulmonary interstitial emphysema (PIE), pneumo-thorax/ mediastinum/ pericardium/ peritoneum, and bronchopulmonary dysplasia.
After delivery, endotracheal administration of exogenous surfactant improves oxygenation, decreases the need for mechanical ventilation, and reduces mortality from SDD [1]. High frequency oscillatory ventilation is often used in these infants [1].
X-ray:
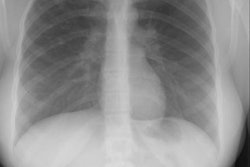
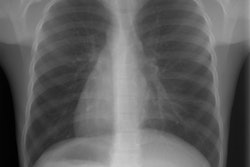
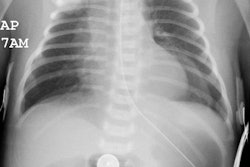
CXR in SDD reflect generalized acinar collapse with LOW lung volumes, diffuse reticulogranularity, and air bronchograms. The findings represent the summation of collapsed alveoli, transudation of fluid into the interstitum from capillary leak, and distention by air of innumerable bronchioles which remain more compliant than the surfactant-deficient lung [1]. The findings are usually present shortly after birth, but occasionally do not reach maximum severity until 12-24 hours [1,2]. Look for evidence of prematurity- the proximal humeral ossification center never ossifies before 36 weeks (although it may not be present in all term infants) If it is present in a cyanotic neonate (ie: full term), this suggests complete transposition of the great vessels, rather than RDS. The radiographic findings in RDS are also typically symmetric- if asymmetric, there may be superimposed infection or pulmonary hemorrhage.Following endotracheal surfactant therapy, follow-up CXR's demonstrate uniform improvement in 38% of infants, asymmetric improvement in 35%, no improvement in 10% [1]. Heterogeneous or asymmetric improvement tends to be most pronounced in the upper and middle regions of the right lung- possibly related to preferential/uneven distribution of surfactant into the right main bronchus [1].
REFERENCES:
(1) Radiographics 2005; Agrons G, et al. Lung disease in
premature neonates: radiologic-pathologic correlation. 25:
1047-1073
(2) AJR 2018; Liszewski MC, Lee EY. Neonatal lung disorders:
pattern re to diagnosis. 210: 964-975