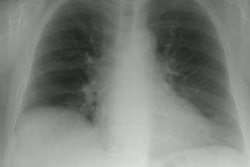
Polymyositis/Dermatomyositis:
View cases of polymyositis/dermatomyositis
Clinical:
Polymyositis/Dermatomyositis (PM-DM) are rare disorders characterized by striated muscle inflammation that predominantly affect middle aged females (females are affected twice as commonly as males [5]). The peak incidence is between the ages of 40 to 50 years [5]. The clinical hallmark of the disorder is subacute myopathy proximal limb and neck involvement with pain, fever, and weakness that evolves over weeks or months [5]. The two conditons are identical, except for the presence of a skin rash which is characteristic of dermatomyositis, but absent in polymyocitis [4]. Skin manifestations include a heliotrope-hued (blue-purple discoloration) skin rash with symmetric violaceous to erythematous periorbital (upper eyelid) erruptions and Grotton papules which are slightly raises violaceous papules and plaques that overlie prominent bones- especially those in the dorsum of the hand (the knuckles) [4,5]. Subcutaneous calcinosis can also occur.The incidence of parenchymal lung disease associated with these disorders ranges from 5 to over 50% of patients in some studies. The incidence of interstitial pneumonia is associated with the presence of anti-Jo-1 antibodies [4]. Interstitial pneumonia occurs in up to 75% of polymyocitis patients with anti-Jo-1 antibodies and is uncommon in patients that lack this antibody [4]. Pulmonary involvement can precede muscle or skin manifestations of the disorder in up to one-third of patients [3].
Two pulmonary forms of PM-DM are recognized: an acute progressive form and a form associated with bronchiolitis obliterans organizing pneumonia (BOOP). The acute progressive form is associated with mixed air space and interstitial lung disease (5-10% of patients) which is histologically indistinguishable from NSIP/UIP. In patients with parenchymal lung disease, those with BOOP have a much better prognosis, than those with UIP (1). Other pulmonary findings include aspiration pneumonia due to proximal esophageal-pharyngeal dysfunction (15-45%) and plexigenic pulmonary hypertension. Patients over the age of 45-60 years with dermatomyositis are at an increased risk for malignancy of the lung, colon, breast, ovary, cervix, and panceas. Treatment for PM-DM consists of steroids or cyclophosphamide.
X-ray:
Computed tomography: In patients with parenchymal lung disease, findings at CT include areas of ground glass opacification, linear opacities, prominent interlobular septa, subpleural lines, irregular peribronchovascular thickening, patchy airspace consolidation, small parenchymal nodules, and honeycombing. [2]Nodular foci of ground-glass opacity with epripheral or circumferential consolidation, the "reverse halo sign", are highly suggestive of an organizing pneumonia pattern [4].REFERENCES:
(1) J Thorac Imag 1996; 11: 250-259
(3) Radiology 1999; Akira M, et al. Interstitial lung disease in association with polymyositis-dermatomyositis: Long term follow-up CT evaluation in seven patients. 210: 333-338
(4) Radiographics 2011; Kanne JP, et al. Beyond skin deep: thoracic
manifestations of systemic disorders affecting the skin. 31: 1651-1668
(5) Radiographics 2012; Capobianco J, et al. Thoracic manifestations of collagen vascular diseases. 32: 33-50