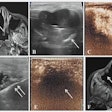
Ultrasound has been around forever. It suffers from low resolution. It hasn't had the same buzzworthy advancements seen in other imaging modalities. But that's changing, thanks to new technologies redefining how ultrasound is performed -- and who gets to perform it.
What's the result? Leading radiologists are increasingly pointing to ultrasound as the imaging method of the future.
"There are a lot of interesting things happening that I hope will reelevate the status of ultrasound within radiology," said Dr. Brian Coley, the radiologist in chief at Cincinnati Children's Hospital Medical Center and one of the expert radiologists who think ultrasound is due for a revamp.
Numerous trends are contributing to the likely reelevation in ultrasound's status in radiology, including a broadening of the user base, a push toward value-based care, and advancements making the technology cheaper, smaller, and more durable. The intersection of these trends presents a unique opportunity -- and challenge -- for radiologists.
"With the democratization of ultrasound and the ubiquity of use among other specialists, radiologists need to up their game if they want to maintain their position as the overall experts in ultrasound," Coley said.
AI, contrast, and other ultrasound improvements at RSNA
The research presented at the RSNA 2020 virtual meeting will offer radiologists one way to learn about ultrasound innovations and up their game. The conference will cover a number of cutting-edge ultrasound topics driving improvements in quality and accuracy.
 Jerome Liang, PhD.
Jerome Liang, PhD.RSNA Physics Chair Jerome Liang, PhD, pointed to exciting new research on emerging sensor technology to improve image quality, as well as the use of artificial intelligence (AI) for signal processing. Meanwhile, RSNA Pediatric Radiology Chair Dr. Lynn Fordham is excited about research and discussion on contrast-enhanced ultrasound applications.
"The use of ultrasound contrasts is really an exciting new direction -- everything from analyzing liver lesions to using contrast for voiding cystourethrograms," she said.
For RSNA Vascular and Interventional Radiology Chair Dr. Ronald Arellano, miniaturization is one of the most exciting topics in all of radiology, and nowhere is that more evident than in ultrasound. It's a revolution he's witnessed firsthand during his vascular radiology career.
For instance, Arellano distinctly remembers a surgery internship where he held retractors for six hours while the surgeon created a surgical shunt between the portal and hepatic veins. Now, he can use intravascular ultrasound to get the same result in 20 minutes with a transjugular intrahepatic portosystemic (TIPS) shunt.
"Having intravascular ultrasound now to help to create that TIPS shunt, to watch in real-time the needle traversing the hepatic vein into the portal vein ... I see that as a major advancement," he said.
Vendors will no doubt be virtually showcasing the next generation of even-smaller tools for ultrasound systems at RSNA 2020. Arellano firmly believes that miniaturization will continue to revolutionize ultrasound-guided procedures in the future.
For instance, one day, he foresees interventional radiologists being able to use ultrasound to guide procedures in the biliary system of the liver and other small, nonvascular channels. Liang said that work to further miniaturize ultrasound equipment is already underway.
Another area ripe with research potential -- and a surefire topic at this year's RSNA meeting -- is the use of artificial intelligence. AI advancements are notoriously challenging for ultrasound because the modality is highly dependent on the user, Fordham noted.
 Dr. Lynn Fordham.
Dr. Lynn Fordham.Despite the inherent difficulties, researchers and vendors have slowly expanded the number of AI applications for ultrasound. Dr. Fiona Gilbert, the RSNA chair for breast imaging, is one of the clinicians eagerly awaiting more AI ultrasound applications.
"Whole-breast ultrasound is quite a time-consuming examination for the radiologist to scroll through all the images," she said. "To have really good AI detection tools for ultrasound would be fantastic. They're being developed, so we're hoping they're going to become available shortly."
The use of synoptic reporting -- a type of structured reporting -- could also expedite future ultrasound AI applications, noted Dr. Christopher Roth, a neuroradiologist and director of imaging informatics strategy at Duke Health.
"Synoptic reporting is like what you would do when filling out a survey form," Roth said. "It's yes/no. Structured questions with structured answers. Doing ultrasound artificial intelligence is really difficult. ... Having structured data that can be associated with the pixel data does open up some possibilities."
Other exciting areas of ultrasound include the use of one-touch features and other tools to address repetitive stress injuries experienced by sonographers. In addition, current ultrasound-guided procedures could potentially be expanded into new organ systems or use cases.
Overall, the experts are excited by the developments making ultrasound technology and image quality even better -- and they don't see that trend slowing down any time soon.
"Ultrasound may have more and more development and advances over the next 10 to 15 years," Liang said.
Radiologists and the point-of-care revolution
Excitement around new diagnostic and technological capabilities has fueled renewed interest in ultrasound use and research among radiologists. Fordham pointed to new grant funding provided by the Society of Pediatric Radiology for pediatric ultrasound research as evidence of that interest.
 Dr. Ronald Arellano.
Dr. Ronald Arellano."Radiologists are recognizing the clinical utility and are successfully able to write grants for funds to further their work," she said.
Coley and Roth added that the shift to value-based payment models may also be driving an increase in radiologist interest in ultrasound.
"Imagers are becoming more aware -- or being forced to become more aware -- of the need to provide value," Coley said. "Ultrasound has a convincing case as a high-value diagnostic tool."
Coley hypothesized that significant payment reform, such as using encounter-based payment models and bundling care, would make ultrasound an even more financially attractive modality in the future.
Roth took that line of thinking one step further.
"Ultrasound is an inexpensive imaging modality that is going to be encouraged more and more if it's diagnostically efficacious enough in coming years, instead of more expensive modalities like CT and MRI," he said.
The excitement around ultrasound -- technologically or financially -- is a departure from recent trends. By and large, interest in ultrasound had largely fallen by the wayside among radiologists, Coley said.
Coley cited a number of reasons for this, including that performing ultrasound scans takes time and effort, resources that are in increasingly short supply for radiologists. Radiologists have also focused their attention on other modalities.
"Look, other modalities are very cool and, for many, have greater sex appeal," Coley said.
This lack of radiologist attention on ultrasound is perhaps most apparent in the research on point-of-care ultrasound (POCUS) for COVID-19 imaging. While radiology has largely focused on CT, emergency physicians have stepped in to fill the ultrasound knowledge gap.
 Dr. Fiona Gilbert.
Dr. Fiona Gilbert."Generally radiologists have not been that involved in ultrasound of the chest, but it's what's available to those point-of-care physicians," Roth said. "In many cases, they are taking a look at COVID patients under ultrasound, and they're doing their own research."
Emergency physicians taking the lead in research on the use of POCUS for COVID-19 reflects broader trends in point-of-care at hospitals. Physicians of all stripes are increasingly using POCUS across the entire care continuum.
The experts all agreed that this trend is being driven by cheaper, better, and smaller devices -- and that it's for the benefit of patients.
"It's great that there's so much more access," Fordham said. "The challenge is to make sure that all of the folks who are using ultrasound have some quality standards in place. And that is a little bit of a challenge."
"A little bit of a challenge" may be an understatement. In coming years, hospitals are going to have to grapple with creating encounter-based workflows that work for different types of providers in different locations. They're also going to have to create ultrasound credentialing and privileging processes for new types of physicians, residents, fellows, and medical students.
At this point in time, the experts agreed that there are far more questions than answers. But the answers to those questions will be determined by decisions being made today, Roth noted.
"Decisions around credentialing and privileging, when to bill, how to handle trainees, what role is radiology going to be, educating the trainees and attending providers around the enterprise -- those decisions are getting made now," Roth said. "If they're not on the ball, the decisions will get made without radiologists."
 Dr. Christopher Roth.
Dr. Christopher Roth.Both Roth and Coley said this is an excellent opportunity for radiologists to step in as imaging leaders within healthcare institutions. For Roth, this responsibility is tied to radiologists' role as the stewards of good imaging. Coley expressed a similar stance.
"Radiology has an advantage in understanding the totality of medical imaging," he said. "It is still in a position to facilitate sensible imaging pathways."
Roth offered five concrete steps radiologists can take today to shape the future of ultrasound use at their institutions:
- Offer guidance to providers and specialties already capturing ultrasound.
- Consider sharing image software with other specialties with appropriate oversight.
- Keep tabs on budgetary decisions regarding new ultrasound purchases.
- Talk to referrers to learn radiology blind spots.
- Get involved in credentialing and privileging committees.
While these steps are not necessarily easy, Roth said they are critically important for radiologists. After all, good imaging is fundamental to patient care, no matter where it happens.
"It's not reimbursed. It's not necessarily a sexy job. But it is something that is critically important to patient care," he said. "Radiologists need to be the stewards of good imaging at the hospitals in which they work."
Programming schedule
Ultrasound sessions on the virtual RSNA 2020 program.
Thursday, December 3
- 3:30 pm-4:30 p.m. -- Education Session: Hepatobiliary Sonography 2020: Update Controversies
Friday, December 4
- 10:00 a.m.-11:00 a.m. -- Education Session: Thyroid Sonography: At a Tipping Point
- 2:00 p.m.-3:00 p.m. -- Education Session: Case-based Review of Ultrasound
Saturday, December 5
- 11:00 a.m.-12:00 p.m. -- Education Session: Case-based Review of Ultrasound
All events are listed in Central time.