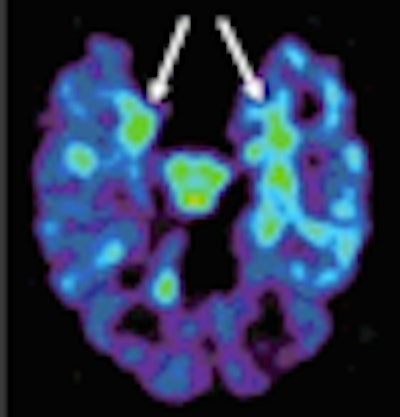
Researchers at the University of California, Los Angeles (UCLA) have produced additional evidence demonstrating that a new PET radiotracer is effective in diagnosing brain aging before symptoms appear, and in differentiating Alzheimer's disease from other less serious neurological conditions.
In studying the aging brain, researchers are looking to "detect the first subtle evidence of decline," said study lead author Dr. Gary Small, a professor at the Semel Institute for Neuroscience and Human Behavior at UCLA and UCLA's Parlow-Solomon Chair on Aging. "What drives this research is the basic idea that we think it will be easier to protect a healthy brain rather than repair a brain that is already damaged."
In previous research published in the New England Journal of Medicine in December 2006, the UCLA researchers used FDDNP and PET to differentiate between Alzheimer's disease and other neurologic conditions. In their most recent study, they used FDDNP and PET to help diagnose brain aging before such symptoms appear. Small said the group "found that FDDNP seems an effective marker for Alzheimer's and to differentiate Alzheimer's disease from mild cognitive impairment and normal aging."
The new study included PET brain scans of 76 volunteers, who had an average age of 76 years and no signs of dementia. The subjects received PET scans after intravenous injection with FDDNP, which binds to plaque and tangle deposits in the brain. Details of the UCLA initiative were published in the January 2009 issue of Archives of General Psychiatry (Vol. 66:1, pp. 81-87).
Pinpointing deposits
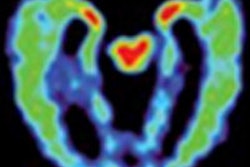
With the combination of FDDNP and PET scans, the researchers were able to pinpoint where abnormal protein deposits were accumulating. The study also noted that older age correlated with higher concentrations of FDDNP in the medial and lateral temporal regions of the brain, which are involved with memory and where plaques and tangles usually collect.
Of the 76 volunteers, 34 carried the APOE-4 gene allele, which heightens the risk for developing Alzheimer's disease. The researchers found that this group exhibited higher levels of FDDNP in the frontal region of the brain, which also affects memory, than study participants without APOE-4.
"We were looking at what happens when you combine several bits of information, not just the scan result, but the results of cognitive data, to give you more information," said Small, who also serves as the director of the UCLA Center on Aging. "Just looking at people who do not have dementia or if they have APOE-4, they are more likely to have FDDNP signal to the brain, which we think reflects a buildup of the abnormal protein deposits that define Alzheimer's."
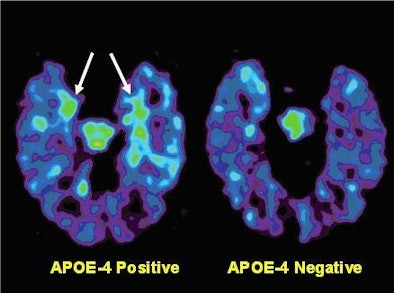 |
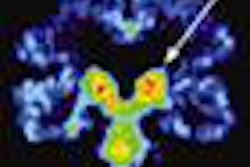
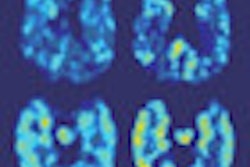
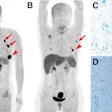
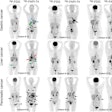
| PET brain scans reveal plaque and tangle accumulation in patients with the APOE-4 gene, which increases risk for Alzheimer's. Image courtesy of Dr. Gary Small and UCLA. |
A subset of the 76 volunteers demonstrated mild cognitive impairment, which increases the risk of developing Alzheimer's disease. The 36 subjects in this group demonstrated greater levels of FDDNP in the medial temporal brain regions than normal volunteers.
In addition, subjects with both mild cognitive impairment and the APOE-4 gene had greater concentrations of FDDNP in the medial temporal brain regions than volunteers who had mild cognitive impairment but no APOE-4.
"We are trying to get to that stage to combine genetic markers and the FDDNP-PET brain scan, to see what's going on years before the people have the condition," Small said.
Disease progression
Small and his colleagues are following the progress of their current volunteers and plan to expand the sample size. They also are currently preparing the next research paper with more detailed follow-up results, delving into the meaning of high FDDNP levels and whether that condition can predict a decline in memory over time or an accumulation of FDDNP signal over a number of years.
"To be useful, we want to see if it correlates with the disease," Small added. "If the disease changes or worsens, do you have a change in the FDDNP signal? If there is, it could be useful in this type of study."
FDDNP-PET scans currently are used only in research settings, but Small said that clinical trials are in development to bring the technology to more patients.
Small said that if Alzheimer's can be detected at its earliest stages, doctors may someday be able to treat patients with drugs, much as they do now for other medical conditions. "Right now, you get a cholesterol test and, if it is high, you take a statin drug to lower your risk for a stroke or heart attack," he said. "I think in the future, you will get a blood test and that will tell the doctor that you should take a certain drug to lower your future risk for Alzheimer's disease."
The study was funded by both government and nonprofit agencies, including the National Institutes of Health, the U.S. Department of Energy, the Ahmanson Foundation, the Larry L. Hillblom Foundation, and the Tamkin Foundation.
By Wayne Forrest
AuntMinnie.com staff writer
January 13, 2009
Related Reading
PET may help differentiate dementia syndromes, uncover ALS, December 2, 2008
PET, PiB support cognitive reserve hypothesis in Alzheimer's, November 14, 2008
WSJ: FDA supports imaging agents for Alzheimer's, October 24, 2008
PET with C-11 PiB can assess beta-amyloid brain deposits, August 12, 2008
PET scans help spot and classify dementia types, March 27, 2008
Copyright © 2009 AuntMinnie.com