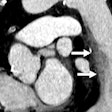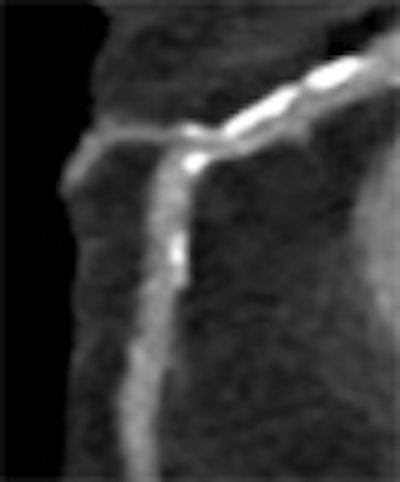
For all its promise, coronary CT angiography (CTA) has been off limits to patients with significant coronary artery calcifications -- there are simply too many nonevaluable segments to justify its use. Motion is another factor that degrades image quality in single-source coronary CTA, and generally only the administration of beta-blockers can overcome it.
Researchers in Zurich, Switzerland, hope to expand the potential CTA patient population substantially with the aid of dual-source CT angiography, which is earning a track record for imaging fast hearts -- and in one recent study, even patients with high Agatston scores and fast hearts.
At the 2007 European Congress of Radiology (ECR) in Vienna, Dr. Hans Scheffel from took a swipe at both limitations by evaluating a problematic population with dual-source CT (DSCT). The patients had high calcium scores and skipped the beta-blockers, but dual-source CT did just fine.
Even with 64-slice MDCT, up to 12% of coronary vessel segments have been deemed nonevaluable in such patients, Scheffel said.
"Recent studies using 64-slice CT scanners have shown high diagnostic accuracy in evaluating coronary artery disease, but there are still factors which may degrade image quality," Scheffel said. "For example, coronary motion and vessel wall calcifications -- up to 12% of coronary segments in some studies have to be excluded from evaluation because they were not assessable."
Aiming to test the diagnostic ability of dual-source CT in this population, Scheffel, with Dr. Sebastian Leshka, Dr. André Plass, and their colleagues at University Hospital Zurich and the Clinic for Cardiovascular Surgery examined 30 patients (six women, 24 men; mean age 63.1 ± 11.3 years) with DSCT.
"The mean Agatston score was 821" (± 904), with a range of 0 to 3,010, Scheffel said. All patients were symptomatic and had a high pretest probability of coronary artery disease (CAD). Invasive coronary angiography, performed within 14 ± 9 days of DSCT, served as the reference standard.
Excluded were patients with contraindications to iodinated contrast, such as renal insufficiency, and those with hemodynamic instability, a history of coronary artery bypass surgery, and other contraindications.
The radiologists acquired images on a DSCT scanner (Somatom Definition, Siemens Medical Solutions, Erlangen, Germany), which is equipped with two x-ray tubes and two corresponding detector arrays mounted on a rotating gantry with an angle offset of 90º.
Gantry rotation time was 330 msec with 120 kVp and 400 mAs, and ECG pulsing was used in all cases, Scheffel said. Slices were 0.75-mm thick with a reconstruction interval of 0.5 mm, he added. Prior to imaging, 80 mL of iodinated contrast material (320 mgI/mL) was injected at 5 mm/sec, using flow tracking set at 100 HU.
Two readers working independently evaluated the image quality of all coronary segments 1.5 mm or larger in diameter using a four-point score (1 was excellent, 4 meant not assessable), and qualitatively assessed significant stenoses as luminal diameter narrowing greater than 50%.
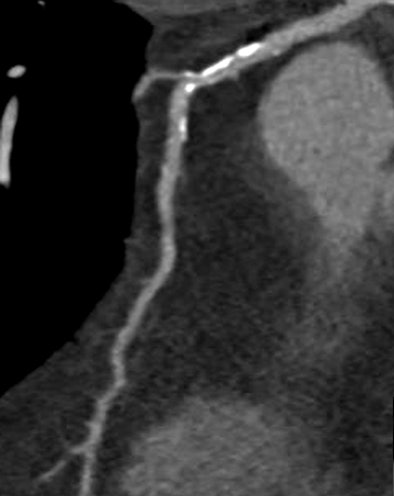
"Image quality was diagnostic in 98.6% (414/420) segments, and the mean image quality was (1.68 ± 0.75)," Scheffel said. Six segments in three patients were considered nonassessable, and DSCT correctly identified 54 of 56 significant coronary lesions.
In all there were nine false positives and two false negatives. The causes were very large calcifications in nine segments, and motion artifact in two segments.
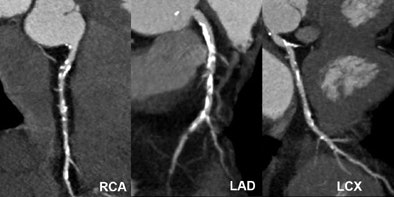 |
| Significant calcified stenosis of the RCA and LAD, both correctly diagnosed with dual-source CT coronary angiography; and nonsignificant stenosis of the LCX. |
On a per-segment basis, the overall sensitivity, specificity, and positive and negative predictive values for evaluating CAD were 96.4%, 97.5%, 85.7%, and 99.4%, respectively. Per-patient sensitivity was 93.3%, specificity was 100%, and positive and negative predictive values were 100% and 93.8%, respectively.
Based on previous tests with an anthropomorphic phantom, the radiation dose was estimated at 7-9 mSv, Scheffel said.
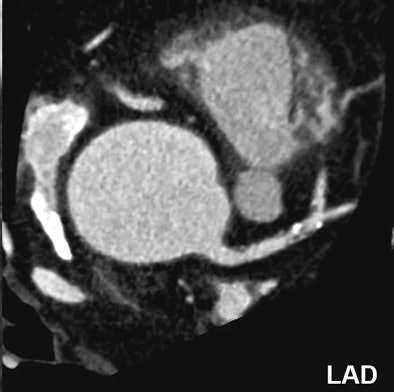 |
| Nonsignificant mixed stenosis of the mid-LAD, false-positive diagnosis with dual-source CT coronary angiography (rated as 60% to 70% stenosis). |
The first experience suggests that DSCT coronary angiography provides high diagnostic accuracy for assessing CAD in a symptomatic patient population with extensive coronary artery calcifications and no beta-blockers, Scheffel said.
"And taking into account these circumstances, there were only six segments that had to be excluded from evaluation, all in distal parts of the coronary artery tree and with small vessel diameters," he said. "The false readings were due to severe calcifications rather than motion artifacts."
However, the small cohort of 30 patients with high pretest probability "may have resulted in overestimation of the ability of DSCT to detect and rule out stenoses," he said. Future studies in populations with a low pretest probability of CAD are expected to provide a better picture of DSCT's capabilities.
"Why did you scan those patients with a high pretest probability?" a session moderator asked. "The more recent guidelines say that in those cases it is not useful to perform CT."
Most patients are imaged in anticipation of heart surgery, Scheffel said, adding that the use of 64-slice CT consistently has been problematic owing to the high number of nonassessable segments.
The facility's current indications for dual-source coronary CTA include:
- Exclusion of CAD in patients prior to cardiac valvular surgery
- Exclusion of CAD in patients prior to cardiac tumor surgery
- Exclusion of CAD in patients prior to noncardiac surgery (for example, repair of abdominal aortic aneurysm)
- Exclusion of CAD and preoperative planning in patients undergoing minimally invasive cardiac surgery
- Exclusion or diagnosis of CAD in patients with a low to intermediate pretest probability of CAD
- Exclusion or diagnosis of CAD, aortic dissection, or pulmonary embolism in patients presenting to the emergency department with acute chest pain
In an e-mail to AuntMinnie.com, study authors Scheffel and Dr. Hatem Alkadhi said the group continues to acquire coronary CTA studies, with an emphasis on patients from the cardiovascular surgery clinic with high calcium loads.
"We consider these patients the most difficult population for CT coronary angiography, particularly because we do not perform heart rate control with beta-receptor antagonists," they wrote. "Fortunately, our cardiovascular surgeons more and more believe in noninvasive CT coronary angiography, and we have recently started to implement dual-source CT coronary angiography as a first-line imaging modality (serving as an excellent filter test) for patients prior to surgery."
The study has been accepted for publication in European Radiology.
By Eric Barnes
AuntMinnie.com staff writer
April 13, 2007
Related Reading
64-slice cardiac CT points to important incidental findings, March 29, 2007
Radiation dose slashed in 64-slice coronary CTA, February 15, 2007
Dual-energy CT may assist in coronary plaque identification, January 15, 2007
Dual-source imaging promises better CT scanning, June 15, 2006
Siemens launches new dual-source CT technology, November 17, 2005
Copyright © 2007 AuntMinnie.com