Nearly three years after the U.S. Food and Drug Administration (FDA) published draft guidance on how it plans to regulate computer-assisted detection (CAD) technology, the agency has released the final versions.
Initially published in draft form in the Federal Register on October 21, 2009, the two guidance documents apply only to what the FDA categorizes as computer-assisted detection (CADe) technology. Technology the agency considers to be computer-assisted diagnosis (CADx) is not included.
The first guidance provides recommendations on documentation and performance testing for a 510(k) submission for class II CADe devices applied to radiology images and radiology device data, while the second guidance offers recommendations on clinical performance studies for both 510(k) and premarket approval (PMA) applications.
While many CAD vendors contacted by AuntMinnie.com declined to comment on the new guidances pending their review of the final documents, those who did were hopeful that the delineation of different forms of CAD would be a positive step for the CAD industry.
The Medical Imaging and Technology Alliance (MITA) said that it and its member companies are examining the documents to determine their effect on manufacturers and customers.
"As a result of almost three years of regulatory uncertainty surrounding the FDA's draft guidances, the marketplace is significantly different than when this discussion began," MITA said in a statement. "We are hopeful that the agency's release of these final guidances will improve predictability and transparency for the CAD industry."
CAD vendor Medipattern CEO Jeff Collins said that the FDA has done a great job of defining CAD technology by officially recognizing CADe and CADx, as well as further defining CAD versus non-CAD products.
"CAD capability and uses have also evolved well beyond the original and best-known mammography CAD during the past decade," Collins told AuntMinnie.com. "As the industry evolved, more types of CAD have been developed. It has become confusing to customers. The new guidelines go a long way to resolving some of this confusion."
CAD definitions
The FDA defines CADe as "computerized systems that incorporate pattern recognition and data analysis capabilities (i.e., combine values, measurements, or features extracted from the patient radiological data) intended to identify, mark, highlight, or in any other manner direct attention to portions of an image, or aspects of radiology device data, that may reveal abnormalities during interpretation of patient radiology images or patient radiology device data by the intended user (i.e., a physician or other healthcare professional)."
Meanwhile, CADx is defined by the FDA as "computerized systems intended to provide information beyond identifying, marking, highlighting, or in any other manner directing attention to portions of an image, or aspects of radiology device data, that may reveal abnormalities during interpretation of patient radiology images or patient radiology device data by the clinician."
Not covered under the guidance documents are CADe devices designed for use in intraoperative procedures, and computer-triage devices such as a prescreening computer scheme that identifies patients with normal MRI scans that do not require any review or diagnostic interpretation by a clinician.
Draft revisions
Based on comments to the draft documents and also comments received during the public meetings of its Radiological Devices Panel advisory committee in March 2008 and November 2009, the FDA said it revised both guidance documents to clarify the level of detail it would like to see regarding the description and operation of CAD devices and about test data reuse, according to a notice in the July 3 edition of the Federal Register.
The new guidance documents also clarify that digitized film is within the scope of radiological data, and that the FDA intends to create new product codes as necessary to identify and track new types of CAD products, according to the notice.
The revisions also include updated recommendations on the CAD scoring process (the procedure for determining the correspondence between the reader's interpretation and ground truth) and when a clinical performance assessment may be necessary.
510(k) guidance
The 510(k) guidance covers CADe devices marketed as a complete package with a review workstation, or as add-on software to be embedded within imaging equipment, an image review platform such as a PACS, or other imaging accessory equipment, according to the FDA.
Examples of devices the FDA said fall within the scope of the guidance include a CADe device intended to identify and prompt colonic polyps on CT colonography studies; a CADe device intended to identify and prompt filling defects on thoracic CT examinations; a CADe device intended to automatically detect liver lesions, and a CADe device intended to identify lung nodules on CT, x-ray, or MRI studies. The full document can be accessed here.
Mammography CADe algorithms are not listed as an example in the new FDA document, leaving open the question of whether mammography CAD technology would still require a PMA.
Clinical performance assessment
The second guidance document provides recommendations to vendors regarding clinical study design, study population, reference standard, reporting, and postmarket planning for PMAs.
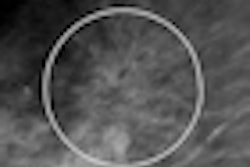
In contrast to the 510(k) guidance, a CADe algorithm designed to identify and prompt microcalcification clusters and masses on digital mammograms is listed as an example of devices that fall within the scope of the clinical performance assessment guidance.
For that document, click here.