MRI is just as effective as CT for assessing body composition in obese individuals at risk of conditions such as type 2 diabetes mellitus and nonalcoholic fatty liver and cardiovascular disease, according to a team of researchers from Spain.
But MRI carries the added benefit of not exposing patients to radiation, noted a group led by Juan Manuel Alcantara, MD, of the Public University of Navarre in Pamploma, Spain. The team's review of body composition assessment techniques was published in the most recent issue of Current Opinions of Clinical Nutrition and Metabolism (Volume 26:5, pp. 440-446, September 2023).
"Although body composition can be assessed by simple techniques, these calculations can provide erroneous results and conclusions, requiring complex interpretations when diverse metabolic situations are concomitantly engaged," it noted. "[Medical] imaging techniques [such as MRI, allow clinicians] to objectively and unbiasedly measure changes that may occur during longitudinal studies (e.g., pharmacological drug interventions)."
Incidence of obesity has increased over the last few decades, and it can negatively affect the body, especially when fat is stored as visceral adipose tissue, the team explained, writing that "it is well known that visceral adipose tissue ... is a representative marker of cardiovascular disease and all-cause mortality."
Assessing how a patient's fat tissue is distributed helps clinicians determine the individual's cardiovascular health risk, the researchers noted. There are non-imaging-based techniques for evaluating a person's body composition -- such as skinfold thickness or bioelectrical impedance analysis, as well as other imaging modalities such as dual-energy x-ray absorptiometry (DEXA) and ultrasound -- but clinicians have been turning more and more to MRI to assess fat distribution because of its high accuracy.
The key benefit of MRI is that its performance is comparable to CT, but it does not impart radiation, the group noted.
| Ability to assess body composition by imaging modality | ||||
| Factor | DEXA | US | CT | MRI |
| Total fat deposits | Yes | No | Yes | Yes |
| Total lean tissue | Yes | N/A | Yes | Yes |
| Visceral adipose tissue | N/A | N/A | Yes | Yes |
| Skeletal muscle tissue | No | No | Yes | Yes |
| Fat fraction in tissues | No | N/A | Yes | Yes |
| Ionizing radiation | Yes | No | Yes | No |
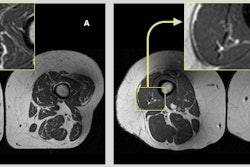
"MRI is comparable to CT in accurately measuring adipose tissue deposits and intermuscular adipose tissue, and muscle volume," the team explained. "Additionally, MRI estimates the fat fraction (expressed as percentage) of different organs as liver, muscle, pancreas or bone marrow tissue. Moreover, because of its high accuracy and reliability, MRI can be used to measure the relatively small changes that may occur during longitudinal and interventional studies (e.g., lifestyle or pharmacological interventions)."
The review offers a useful primer for defining a patient's fatty tissue deposits and thus risk of disease, Alcantara and colleagues concluded.
"There are no doubts that ectopic adipose tissue deposits are strongly associated with cardiovascular disease and metabolic risk factors, and that all deposits are interrelated," they wrote. "Thus, determining their specific roles and underlying mechanism in the pathophysiology of cardiovascular disease represents a fertile research area for future investigations in whole-body ectopic adipose tissue deposits."
The complete study can be found here.




![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=167&q=70&w=250)