Changes in body composition over time can be identified on total-body dual-energy x-ray absorptiometry (DEXA) exam by artificial intelligence (AI) algorithms and help to predict mortality risk, according to research presented at RSNA 2021 in Chicago.
After developing deep-learning algorithms on data from over 3,000 subjects, researchers from the University of Hawaii found that DEXA image data-enhanced mortality predictions.
"Including longitudinal and total-body DEXA information [in deep-learning models] does improve mortality prediction," said presenter Yannik Glaser, PhD.
Although it's known that body composition and changes in body composition are related to mortality, that relationship can be complicated, Glaser said. In addition, there also hasn't been much research investigating the use of imaging in mortality prediction.
The researchers hypothesized that total-body DEXA scans could provide relevant body composition information beyond what's reflected in traditional risk factors. Furthermore, they theorized that tracking these body composition changes over time on longitudinal total-body DEXA scans could improve mortality risk models.
They trained deep-learning algorithms on data from 3,075 participants in the Health, Aging and Body Composition (Health ABC) study. For the first hypothesis, the researchers trained three specific deep neural networks: a model using only analysis of body composition on total-body DEXA exams; an algorithm that used only traditional mortality risk factors such as blood markers, general fitness indicators, and disability; and a model that combined both methods.
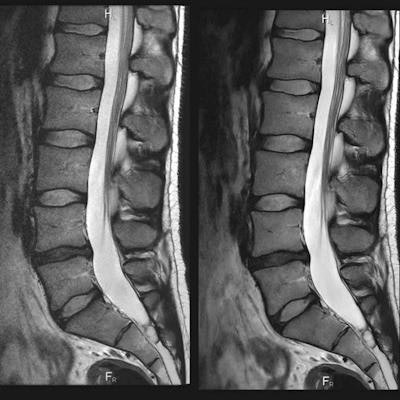
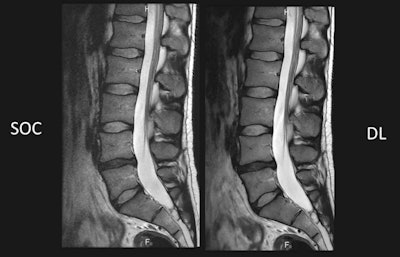 Comparison of standard of care (SOC) against deep learning-based (DL) reconstruction at 60% shorter scan time. Images courtesy of Dr. Lawrence Tanenbaum.
Comparison of standard of care (SOC) against deep learning-based (DL) reconstruction at 60% shorter scan time. Images courtesy of Dr. Lawrence Tanenbaum.In addition to these cross-sectional models that analyzed each data point separately, the researchers tested their second hypothesis by developing longitudinal models that treated a patient's sequence of DEXA scans as a single data point.
After reviewing the first hypothesis that inclusion of imaging data could improve mortality predictions, the researcher found that although the algorithm based only on image analysis didn't perform as well as the model that included only traditional risk factors, it did provide complementary information. The algorithm combining both methods yielded the best results.
"This trend also holds for the longitudinal results, but most importantly, all of the longitudinal models outperformed all of the cross-sectional ones, indicating that this inclusion of longitudinal data is really beneficial for mortality prediction," Glaser said.
| Improved area under the curve for mortality prediction by incorporating sequential data analysis | ||
| Cross-sectional models (isolated analysis of each record) | Longitudinal models (treating sequential data as one data point) | |
| Total-body DEXA exam | 0.63 | 0.73 |
| Traditional risk factors | 0.69 | 0.76 |
| Combination of risk factors and total-body DEXA analysis | 0.71 | 0.79 |
In further analysis, the researchers found that of the five most informative risk factors for mortality, three -- fasting serum glucose, walking speed (long), and walking speed (medium) -- can be directly targeted by lifestyle interventions, Glaser said.
Glaser noted that the algorithm's gradient-weighted Class Activation Mapping (Grad-CAM) feature maps indicate that the model learned to correctly identify biologically relevant areas for mortality prediction.
The model -- especially the one that includes longitudinal data analysis -- can help motivate patients to adhere to lifestyle interventions, according to Glaser.
"With the sequence data, you can kind of monitor how it progresses over time," Glaser said.
In the future, the researchers plan to validate the models more extensively on datasets beyond the Health ABC study, Glaser said.