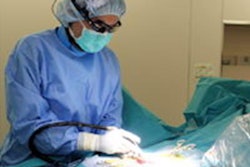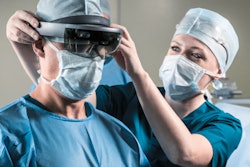
Researchers from Brazil have developed a way to visualize and interact with patient-specific anatomy using augmented reality (AR) and 3D printing. They describe how the technique could improve preoperative planning for cranial surgery and patient outcomes in an article in the March issue of Neurosurgical Focus.
The group, led by Dr. Giselle Coelho, PhD, from the University of São Paulo, turned to 3D printing and AR technology to provide physicians with a more detailed and realistic visualization of cranial anatomy than currently possible with conventional imaging alone.
In the case of complex neurosurgical procedures, CT and MRI offer a limited view of patient anatomy with no tactile perception and minimal insight into relationships between different anatomical structures, Coelho and colleagues wrote (Neurosurg Focus, March 2020, Vol. 48:3, p. E19). Conversely, the combination of 3D printing and AR "join multisensory inputs of touch and vision, leading to improved spatial conceptualization compared with simple 3D anatomical images."
The researchers applied this concept retrospectively to the case of a 5-month-old boy diagnosed with metopic craniosynostosis and who had undergone a challenging and high-risk surgical procedure.
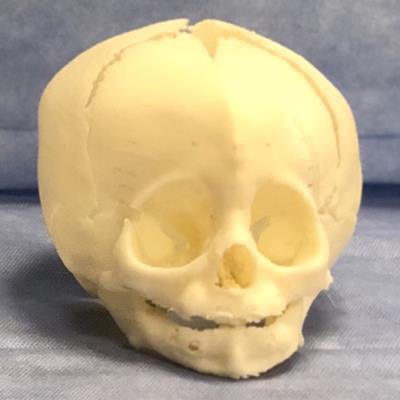
First, they created a 3D-printed skull model based on the patient's CT scans. The model was composed of resin and various types of silicone resembling the texture and mechanical resistance of human tissue.
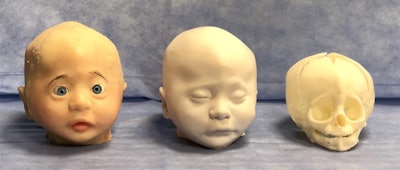 3D-printed models based on head CT scans of a patient with metopic craniosynostosis. Image courtesy of Dr. Giselle Coelho.
3D-printed models based on head CT scans of a patient with metopic craniosynostosis. Image courtesy of Dr. Giselle Coelho.Then the researchers used computer software to transform the CT data into virtual 3D models compatible for viewing with AR technology. They also developed an AR application that enabled users to project the virtual 3D models onto a real-world environment with a smartphone.
Using both the AR and 3D-printed skull models, surgeons were able to plan the optimal surgical approach and simulate frontal craniotomy using surgical instruments as if it were a real surgery. The measurements they obtained from the models to perform the simulated procedure matched the measurements used to complete the actual surgery.
The 38 neurosurgeons and craniofacial surgeons who tested the AR smartphone application evaluated its utility for surgical planning and educational purposes by filling out a questionnaire.
Overall, more than 76% of the surgeons agreed or strongly agreed that using the AR simulator for preoperative planning was extremely useful, and roughly 74% believed that using the simulator could improve postoperative outcomes. All but one surgeon (97%) found it possible to diagnose the patient's condition using the simulator and agreed that it could contribute to family understanding of the patient's condition.
The vast majority of surgeons also agreed or strongly agreed that practicing with the simulator would improve their ability to determine the best surgical approach (82% of surgeons) and would participate in future preoperative planning sessions with the simulator (86%).
"The remarkable realism of this method significantly enhances the teaching of surgical anatomy and operative strategies in the neurosurgical field ... [and] may provide a complementary educational tool in any preoperative surgical planning, enhancing the safety of the procedure and contributing to a better outcome," Coelho and colleagues wrote.
Production of the 3D-printed skull model cost approximately $1,700, and the AR mobile platform is not yet commercially available.
The combination of AR and 3D printing "can be applied in a revolutionary and safe manner to the training of neurosurgeons in performing other operative techniques used in the correction of craniofacial malformations," they concluded.