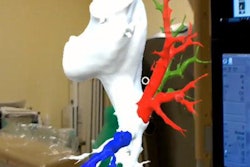
Researchers in the U.S. have created hundreds of individually tailored 3D-printed cardiac models to facilitate presurgical planning for pediatric heart disease. Using these models has helped lower operating times and reduce costs, according to a new article published in 3D Printing in Medicine.
The group, led by first author Justin Ryan, PhD, assessed the utility of 3D-printed heart models as an alternative to more conventional medical images for planning complex surgeries for pediatric patients with heart disease at Phoenix Children's Hospital. Over the course of three years, the researchers found that applying 3D printing to preoperative planning not only helped clinicians reduce the time required to complete surgery but also lowered patient morbidity as well (3D Print Med, November 8, 2018).
Since completing the study at Phoenix Children's, Ryan has moved to Rady Children's Hospital in San Diego, where he serves as director of the hospital's new 3D Innovations Lab.
"It is still challenging to describe the specific impact of surgical planning with 3D printing, but our numbers support a positive trend for reduced operating time and length of stay," Ryan told AuntMinnie.com. "Improved time metrics are linked to a better economic scenario, and less time spent in the operating room has a correlation with better patient outcomes."
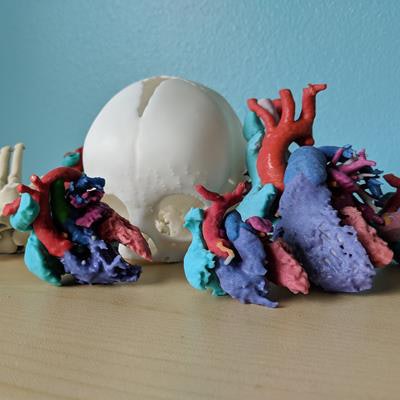
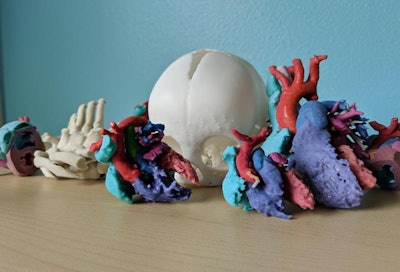 Color-coded 3D-printed heart models. Image courtesy of Justin Ryan, PhD.
Color-coded 3D-printed heart models. Image courtesy of Justin Ryan, PhD.3D-printed pediatric hearts
Congenital heart disease (CHD) is characterized by severe anatomical deviations that often require surgical intervention, and it is the leading cause of mortality from birth defects. Traditionally, clinicians have relied on CT, MRI, and echocardiography to diagnose and plan treatment for patients with CHD, but images from these conventional imaging modalities provide a limited visualization that does not necessarily capture anatomical structures in their entirety, the authors noted.
At the start of 2012, Ryan and colleagues acquired a 3D printer and launched a 3D printing lab at Phoenix Children's Hospital, in large part to offer cardiologists and surgeons a more intuitive, hands-on way to visualize patient anatomy. Thus far, they have produced more than 500 3D-printed models and have developed a framework that allows for the delivery of same-day prints.
For this retrospective study, the group reviewed how implementing these models into presurgical planning affected the quality and efficiency of pediatric heart surgery at the hospital between September 2012 and December 2014.
Among nearly 1,000 cases, the researchers examined 79 for which clinicians referred to 3D-printed models for preoperative planning. They compared these cases with 113 in which planning involved standard care instead of 3D-printed models.
Ryan and colleagues created the models by segmenting the patients' CT or MRI scans using image processing software (Mimics Innovation Suite, Materialise) and reconstructing these scans into 3D virtual models. They then had a cardiologist or radiologist review each model and assess anatomical accuracy and proper color coding before finally printing the models using a binder-jetting 3D printer (ZPrinter, 3D Systems).
"As an extension of medical imaging, we recognize the role radiology plays in 3D printing," Ryan said. "We regularly work with radiologists to improve the image quality of CT and MRI scans to ensure the 3D reconstructions are as clear and sharp as possible, and to refine questionable areas before presenting 3D-printed models to other clinicians."
More favorable outcomes
On average, the surgical team members completed operations more quickly when they planned them using 3D-printed models instead of conventional medical images. Although the results did not achieve statistical significance, every response variable trended toward more favorable outcomes for the hospital and patient.
This included patient mortality and morbidity, which the researchers measured based on the patients' rates of mortality and readmission to the hospital within the first 30 days after surgery.
| Preoperative planning for heart surgery with and without 3D-printed models | ||
| Standard of care | 3D-printed model | |
| Average time spent in surgery | 229.33 minutes | 220.7 minutes |
| 30-day readmission rate | 56.12% | 12.95% |
| 30-day mortality rate | 1.37% | 0% |
In terms of cost, 3D printing necessitated approximately $150 to $200 per model in material expenses alone. However, the consistent reductions in operating time more than made up for these costs, Ryan said.
"There are costs for every minute a patient is in the operating room," he said. "The Mayo Clinic estimates costs of $80 to $150 per minute. So if we save a couple of minutes, we have already saved enough money, not to mention the positive impact this [reduced surgical time] has for patients."
After each operation, the cardiothoracic surgeons filled out surveys from the researchers. The results of the questionnaires indicated that examining the 3D-printed heart models helped the surgeons improve their spatial acuity. The models also appeared to address deficiencies in the conventional visualization of medical images during preoperative planning.
A number of surgeons rated the 3D-printed models highly in terms of perceived usefulness and ease of use. All of the surgeons agreed that the 3D-printed models enhanced their ability to execute surgical repair for applicable cases. Several of them also mentioned that the models displayed components of patient anatomy that they did not expect to see based on conventional imaging for at least three of the cases.
'A matter of time'
"More and more hospitals are using 3D printing," Ryan said. "And 3D printing labs are starting to adopt a whole-hospital approach that involves numerous specialties ... and is also inclusive of augmented reality and virtual reality."
Ryan and colleagues recommended that clinicians interested in testing the waters with this technology begin by establishing a good collaboration with a nearby academic institution. They also suggested that newcomers consider reaching out to experienced members of the RSNA's 3D Printing Special Interest Group.
Beyond its relevance to 3D printing, reconstructing medical images produces data that allow for additional analysis of anatomical geometry, according to co-author Jonathan Plasencia, PhD.
"Recently, we have been taking 3D [imaging] data from the pipeline of the 3D printing process and saving it for future machine-learning projects," he said.
"The underlying data used to generate 3D-printed models can be leveraged and mined for its incredible information," Ryan said. "We're making rapid increases in consistencies and standardization efforts. ... It's only a matter of time before more hospitals get this technology into their system."