Breast cancer care doesn't have to be mysterious, according to radiologist Rachel Brem, MD, and breast surgeon Christy Teal, MD, both of George Washington University in Washington, DC.
In May, the two published a book with Simon & Schuster called No Longer Radical: Understanding Mastectomies and Choosing the Breast Cancer Care That's Right for You that offers readers an outline of not only the nature of breast cancer but also how women can discern what treatment is best for them once they are diagnosed. In this excerpt from Chapter 2, the authors address high-risk screening and the politics of breast tissue density.
We also have an interview with Brem and Teal in which they further discuss the book.
High-risk screening
Because of the incredible strides in early detection of breast cancer and targeted and novel therapies, the death rate from breast cancer has declined by almost half in the past 20
years. Most women (63%) are diagnosed before the cancer has metastasized, or spread to other parts of the body. The five-year survival rate for early breast cancer is greater than 95%. We've seen major advances in diagnosis, treatment, and screening. Now the question is, how do I screen for breast cancer, understanding that every woman is at risk, and that breast cancer found early is curable? Screening for breast cancer has become far more personalized in recent years. It's no longer assumed that every woman should be screened with only a mammogram every year. So how can you make sure you're getting the care you need?
Two primary criteria
We now routinely adjust surveillance, or screening, for breast cancer based on two primary criteria: your breast density and your risk of getting breast cancer.
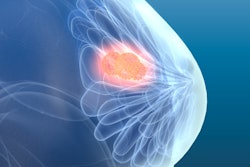
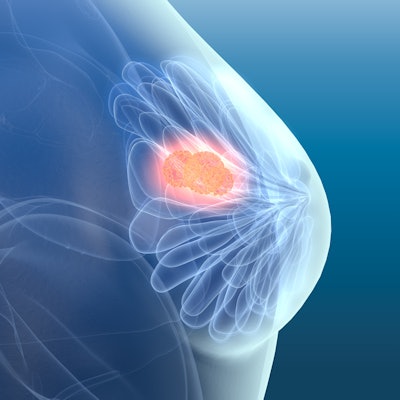
Breast density is determined by the amount of glandular tissue in a breast. It's a strong risk factor for developing breast cancer. Currently, the only way to know if you have dense breast tissue is to see how much white tissue there is on your mammogram.
Women with dense breast tissue, like all women over age 40, must have an annual mammogram to detect early, curable breast cancer. The challenge is that on a mammogram, breast tissue is white and breast cancer is white. Therefore, the ability to detect breast cancer with a mammogram is significantly diminished in women with dense breasts. What is even more daunting is that the risk for developing breast cancer is up to four times higher in women with dense breasts.
Overall, mammography detects 85% of breast cancers, but in women with dense breasts, that decreases to between 45% and 65%. Although this is disappointing, it's critical to remember that mammography still finds most cancers in women with dense breasts, and it remains an important component of screening for breast cancer.
If you have dense breasts, there are additional ways to look for cancers that are hidden in mammograms. MRI can certainly find these cancers. So can screening breast ultrasound, the same ultrasound that's used to image babies in utero, which doesn't use ionizing radiation. In fact, on an ultrasound, dense tissue is white and breast cancer is dark, so the ability of ultrasound to detect breast cancer in women with dense breasts is actually better. That being said, there are certainly still cancers that can be seen only through mammography, even in women with dense breast tissue.
If the report given to you by the radiologist indicates that you have dense breasts, you should insist on an annual screening breast ultrasound. Numerous studies, including some that we had the privilege of leading, have shown that in women with dense breasts, ultrasound can find up to 25% more cancers. That alone is a great stride forward. Furthermore, the types of cancer that ultrasound finds in women with dense breasts are clinically critical cancers -- small, early, invasive breast cancer. These are the cancers we must find to save lives, because they have the propensity to metastasize and become killers.
It's critical that women with dense breast tissue have annual screening ultrasounds in addition to annual screening mammograms to optimize their ability to detect early, curable breast cancers.
The politics of breast density
The issue of breast density isn't only medical but political. Women deserve the right to know about the importance of breast density. In 2018, 29 states had laws that required an indication of a woman's breast density be part of the letter that's sent to her with her mammography results. In 2022, 37 states and the District of Columbia had breast density notification laws, and a federal bill was introduced in Congress that year.
Where we work with and care for women in the District of Columbia, the death rate from breast cancer is the highest in the country. In response to this, Andrea Wolf, CEO of the Brem Foundation to Defeat Breast Cancer, helped write and pass the Breast Density Screening and Notification Amendment Act of 2018 (D.C. Law 22-261), which requires doctors to inform women of their breast density and insurance companies to cover not only ultrasound but also MRI and any future technologies to screen for cancer in women with dense breasts. Not only did the bill unanimously pass but D.C. went further and, with the support of the Brem Foundation, included the requirement that insurance companies provide mandatory coverage of the cost of the lifesaving additional annual ultrasound and other screening imaging studies for women with dense breast tissue.
Andrea's vision and commitment to improving outcomes for women has resulted in her initiating a movement to change the wording of adjunct screening for women with dense breasts from "additional" to "essential screening," since that's what it is, and now the terminology that's increasingly being used reflects this. This was not enough for Andrea and the team at the Brem Foundation. For many underserved women, free mammography was not enough. There was an enormous barrier to obtaining lifesaving mammography: Although one of the benefits of the Affordable Care Act was no-cost mammograms, underserved women often didn't have the means to get to appointments. The Brem Foundation partnered with the ride-share company Lyft to develop a program to break down the barrier for under-resourced women called Wheels for Women, providing no-cost-to-them rides to their free mammograms. This program has been a resounding success and is being utilized by many more women than expected. Women's lives are truly being saved by the breast density notification bill, the Wheels for Women program, and the change in language from "additional" to "essential" screening.
Today, 37 states and the District of Columbia have passed breast density notification legislation requiring that women be informed of their breast density. However, these laws are all different: some simply tell a woman she has dense breasts; some include information about other imaging modalities, such as ultrasound and MRI, that can find additional cancers that are hidden on mammography; and some require insurance coverage of the additional testing. Once again, breast cancer isn't only a medical condition but a political one, which hopefully will further empower women with the knowledge they need to advocate for and seek the care they deserve.
From No Longer Radical by Dr. Rachel Brem and Dr. Christy Teal. Copyright © 2023 by Dr. Rachel Brem and Dr. Christy Teal. Reprinted by permission of Simon Element, an Imprint of Simon & Schuster, Inc.
The comments and observations expressed are those of the authors and do not necessarily reflect the opinions of AuntMinnie.com.