When a patient learns that cancer has spread from a primary tumor to other anatomic regions, what else can be done? Metastasis is the leading cause of cancer death -- but metastasis is not always widespread and may lend itself to radiation therapy.
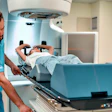
Preliminary results from an ongoing clinical trial at the University of Chicago reveal that some patients with low-volume metastatic cancer restricted to a limited number of organs may benefit from stereotactic body radiotherapy. The first prospective test of targeting radiotherapy to multiple organs simultaneously has determined not only that carefully selected patients can tolerate the treatment and be treated safely, but also that a portion of them do not have their cancer progress.
For a handful of patients with metastatic cancer, the outcome of this clinical trial offers hope that such therapy will curtail tumor progression and spread of metastases, and even potentially render them free of the disease. Research on the trial was published in the August 15 edition of Clinical Cancer Research (2008, Vol. 14:16, pp. 5,255-5,259).
In the study, researchers at the University of Chicago hypothesized that patients with oligometastases, a condition in which a low volume of metastatic lesions are limited to several organs, might benefit from local therapy administered to all the cancerous regions at the same time. They were following up on an analysis conducted in 2004 by the university's department of radiation and cellular oncology that determined that half of the institution's non-small cell lung cancer patients had metastasis limited to three additional sites other than the primary tumor.
Based in part on this finding, and the fact that stereotactic body radiotherapy allows for the delivery of a few tightly focused high radiation doses while sparing dose to adjacent normal organs, the researchers initiated a dose-escalation trial with confirmed stage IV cancer patients who had metastatic disease limited to one to five anatomic sites.
Surgery is generally not considered an option for patients with oligometastases. The standard treatment regimens of systemic cytotoxic chemotherapy and hormonal manipulations are rarely curative and can also be ineffective, according to lead author Dr. Joseph Salama, an assistant professor of radiation and cellular oncology at the University of Chicago.
Criteria for inclusion in the trial included:
- Having a life expectancy of more than 90 days
- Being 18 years of age or older
- Having each tumor dimension no greater than 10 cm
- Having no prior radiotherapy to involved tumor sites
- Not receiving chemotherapy during the clinical trial (hormonal therapy was allowed)
- Having normal marrow and organ function
- Having an Eastern Cooperative Oncology Group performance status of 2 or less
The clinical trial commenced November 2004, with 29 patients enrolled. Of the patients, 24 had received prior systemic therapy before enrollment. They represented a wide variety of primary tumor sites, including lung (27.6%), head and neck (17.2%), colon/rectum (13.8%), breast (13.7%), extremity sarcoma (10.3%), renal (10.2%), uterine (3.4%), and ovary (3.4%).
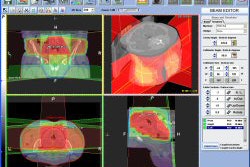
A CT scan was performed within 30 days of treatment, and radiotherapy planning was performed using standard techniques including CT simulation coordinated with the patient's respiratory cycle. Tumors were expanded 5-7 mm before radiotherapy planning, and a variety of nonoverlapping axial fields and noncoplanar fields were combined to achieve the optimal radiation distribution around the tumors while minimizing radiation to surrounding noninvolved organs.
A total of 56 metastatic lesions were identified and treated. Each metastasic lesion was classified within an abdominal, extremity, head and neck, liver, or lung anatomic region. A standard 3+3 dose escalation schema was used, escalated in 2 Gy increments. The same dose was administered for each of three treatments performed, but the dose could be greater or less based on the anatomic region.
The starting dose for all sites was 24 Gy delivered in three 8-Gy fractions, and the protocol-specified maximum dose was 60 Gy in three 20-Gy fractions, each separated by a minimum of 48-192 hours. A physical examination was performed upon completion of each radiation fraction.
Patients were examined twice in the first month, once monthly for the next three months, and then every three months thereafter. CT and PET examinations were performed one month following the completion of treatment and every three months thereafter.
The overall irradiated tumor control rate was 57% as of April 2008, when Clinical Cancer Research accepted the article for publication. A complete response was achieved in 31 tumors (55.4%), two (3.6%) achieved a partial response, and 20 (35.7%) maintained stable disease. Only three tumors (5.4%) did not respond to treatment.
Acute and chronic toxicity has been limited, according to Salama and colleagues. Only one patient experienced grade 3 pneumonitis, and one patient experienced grade 3 nausea because the patient did not take prescribed antiemetics before treatment. A third patient experienced grade 3 gastrointestinal hemorrhage three months after treatment completion.
As new research is published about stereotactic body radiotherapy doses, the University of Chicago is modifying its protocols with new patients. As of September 2008, 50 patients are currently enrolled in the clinical trial. Breast cancer patients seem to be responding well to this type of treatment, and in part because of this, Salama reports that further trials are being planned to specifically focus on patients with breast cancer, kidney cancer, and non-small cell lung cancer that has metastasized.
By Cynthia Keen
AuntMinnie.com staff writer
October 21, 2008
Related Reading
Stereotactic radiotherapy shows promise in acromegaly, August 26, 2008
Stereotactic radiosurgery can extend survival in small recurrent glioblastomas, June 20, 2008
Stereotactic single-dose radiotherapy an option for early lung cancer, August 29, 2007
Stereotactic radiosurgery improves survival after melanoma brain metastases, May 24, 2007
Whole-brain radiation does not improve on stereotactic radiation, June 8, 2006
Copyright © 2008 AuntMinnie.com