A half dose of a commercially available MRI contrast agent works as well as a full dose in patients with acute myocardial infarction, according to Italian researchers. The findings show it's possible to achieve shorter imaging times while protecting renally impaired cardiac patients at risk for nephrogenic systemic fibrosis (NSF).
NSF is a debilitating and sometimes fatal condition that can cause fibrosis of the bone, kidneys, lungs, muscle, and other structures, and it's been a major concern for patients with kidney problems who receive large doses of gadolinium-based contrast agents.
"Until now, there has been no consensus on the ideal dose of contrast medium and the exact time of data acquisition," said lead author Dr. Iacopo Carbone from the University of Rome "La Sapienza." "We should take into account, especially in patients with acute myocardial infarct who already underwent administration of iodinated contrast media for primary angioplasty, that it is common sense to use as little as possible a dose of gadolinium to avoid the complication of NSF."
Patient analysis
Researchers analyzed 15 consecutive patients (11 males and four females) with acute myocardial infarcts. The patients all underwent two consecutive cardiac MRI examinations at least 24 hours apart on a 1.5-tesla system. Gadolinium-BOPTA (MultiHance, Bracco, Milan, Italy) was administered at a dose of 0.05 mmol/kg, based on body weight (bw), for one examination and 0.1mmol/kg/bw for the second scan in random order.
The interval between the two MRI scans was 24 to 48 hours. Both scans recorded data during the MR image sequences before gadolinium-BOPTA administration, and then again at one, three, five, 10, 15, and 20 minutes after injection of the two different dose amounts.
Two radiologists evaluated the images and measured the contrast-to-noise ratios in the infarcted myocardium, noninfarcted myocardium, and left ventricle cavity. All the measurements were performed at each time point for every image for both contrast agent dose amounts, added Carbone, who presented the study at the 2009 annual RSNA meeting.
Statistical difference
In the results, the researchers found a statistically significant difference in image quality for the standard and half dose at each time point in the comparison of the infarcted myocardium and noninfarcted myocardium, and in the comparison of the infarcted myocardium and left ventricle cavity.
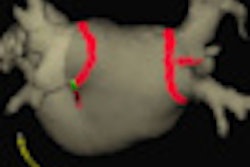
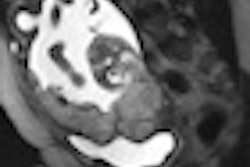
In measuring the signal intensity, the researchers found that the mean relative percent contrast between infarcted myocardium and noninfarcted myocardium was 774.4% for the 0.1 mmol/kg dose and 772.6% for the 0.05 mmol/kg dose. However, the maximum relative contrast was reached in a shorter time (10 minutes) with the dose of 0.05 mmol/kg than with the 0.1 mmol/kg dose (15 to 20 minutes).
With a 0.1 mmol/kg/bw dose, the signal intensity of the infarcted myocardium was lower than the signal intensity of the left ventricular cavity at each time point between 0 and 20 minutes.
Conversely, for the 0.05 mmol/kg/bw dose, the signal intensity of the infarcted myocardium was significantly higher (p < 0.05) than the signal intensity of the left ventricular cavity starting at 10 minutes after injection.
Half-dose benefits
"Based on our results, we can conclude that a half dose of gadolinium-BOPTA gets comparable results to a full dose, with shorter acquisition times for the depiction of delayed enhancement in patients with acute myocardial infarction," Carbone said. "The use of gadolinium-BOPTA at the half dose can help reduce examination times, reduce costs, and especially could be very useful in patients at high risk for NSF."
The study also noted that "superior contrast" between the infarcted myocardium and the left ventricle cavity is achieved with a dose of 0.05 mmol/kg of gadolinium-BOPTA, "which better delineates the subendocardial face of infarcted myocardium."
By Wayne Forrest
AuntMinnie.com staff writer
January 21, 2010
Related Reading
FDA panel: NSF incidence falls with gadolinium restrictions, December 9, 2009
MRI contrast media switch eliminates NSF cases, October 15, 2009
Mayo study finds few serious reactions to CT and MRI contrast, September 21, 2009
Gadolinium-based contrast agents alone don't cause NSF, study finds, July 8, 2009
JHU study: Screening patients prior to MRI lowers NSF risk, February 4, 2009
Copyright © 2010 AuntMinnie.com



![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=100&q=70&w=100)





![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)








