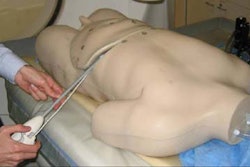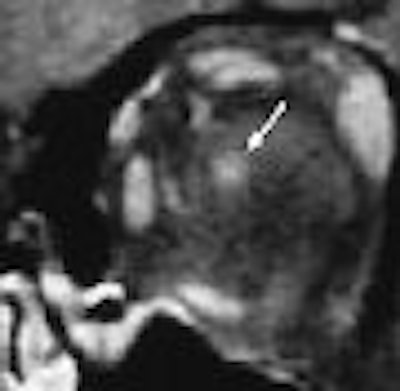
When a patient experiences sudden yet ongoing vision problems, concerns about tumor or multiple sclerosis may prompt the ordering of an MRI. But Florida researchers have now identified MR features that will offer some patients a reassuring diagnosis of cat scratch disease (CSD) as the cause of their symptoms.
A team from the University of Florida in Gainesville, led by Dr. Ilona Schmalfuss, is apparently the first to extensively evaluate MRI findings in CSD-related optic neuropathy.
Their study, which found CSD effects very localized to the optic nerve-globe junction, appears in the latest issue of the American Journal of Neuroradiology (June/July 2005, Vol. 26:6, pp. 1310-1316).
Cat scratch disease is far more likely to cause lymphadenopathy than optic neuropathy, so patients with the latter are perhaps more likely to endure diagnostic uncertainty despite their self-limiting infection.
"We had several patients who had been going from one hospital to the next and nobody was able to help them," said Schmalfuss, in an interview with AuntMinnie.com. "A lot of the patients are just desperate to have a diagnosis."
Exacerbating the problem is the fact that macular exudate that characterizes CSD may not appear until weeks after the vision problems begin. Thus, a radiologist reading the MRI may be the first physician to suggest CSD, Schmalfuss said.
"What is unique about cat scratch disease is that the imaging really helps because it is, based on our data, able to distinguish it," Schmalfuss said. "This has significant implications for the patients because they know they're unlikely to have MS."
There's also an imperative for a speedy MR diagnosis when optic neuritis is a precursor to multiple sclerosis, according to Schmalfuss and her coauthors. Specifically, the Optic Neuritis Treatment Trial has shown that intravenous administration of high-dose steroids decreases the risk of progression of optic neuropathy to multiple sclerosis within two years of follow-up.
In their retrospective study, the Florida researchers looked at patients diagnosed with various causes of optic neuropathy at their institution between January 1995 and March 2003. After eliminating more than 100 image sets with inadequate fat suppression or other issues, they evaluated the MRI features found in 82 patients with optic neuropathy.
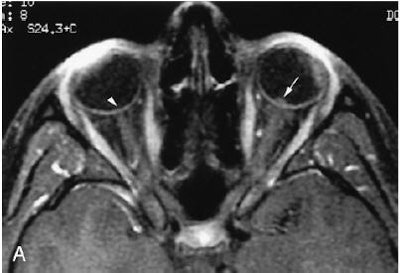 |
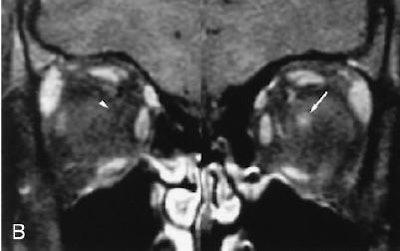
| Seventeen-year-old girl with moderate imaging findings of optic neuropathy due to cat scratch fever. Axial (A) and coronal (B) gadolinium-enhanced, fat-suppressed, T1-weighted images (TR1, Tr2/TE, 735, 875/14) show bulging of the left optic disk (arrow in A) that is markedly less pronounced than that on the right (arrowhead in A). The associated enhancement at the left optic nerve-globe junction (arrow in A and B) is also markedly less extensive. Note that normal appearance of the optic nerve-globe junction region on the right (arrowhead in A and B). Schmalfuss IM, Dean CW, Sistrom C, Bhatti MT, "Optic Neuropathy Secondary to Cat Scratch Disease: Distinguishing MR Imaging Features from Other Types of Optic Neuropathies" (AJNR, 26:1310-1316, June/July 2005). |
 |
Of those 82 cases, 42 (51%) had ultimately been deemed idiopathic, 18 (22%) were diagnosed as ischemic optic neuropathy, nine (11%) attributed to cat scratch disease, another nine related to multiple sclerosis, and one each due to sarcoidosis, radiation exposure, compression by tumor, or giant cell arteritis.
All of the MRIs were evaluated separately by a neuroradiologist and a neuro-ophthalmologist who were blinded to patient identifiers, demographics, medical histories, clinical exams, laboratory results, and final diagnoses.
Four of the nine patients diagnosed with CSD-related optic neuropathy had normal-appearing optic nerves on the reviewed MR images, the researchers found.
Among the other five, the enhancement of the optic nerve was localized to a 3- to 4-mm segment at the optic nerve-globe junction, the authors wrote. In contrast, 31 patients with non-CSD-related neuropathy showed enhancement away from the optic nerve-globe junction or a long-segment enhancement when that junction was involved.
"The analysis of variance revealed a significant difference in both extent of enhancement (p < 0.018) and distance between the optic nerve-globe junction and the beginning of enhancement (p = 0.004) between the patients in the cat scratch disease group and those with other types of optic neuropathy," the authors wrote.
"The finding of optic nerve enhancement confined to the optic nerve-globe-junction was 56% sensitive (5/9 disease-positive patients) and 98.6% specific (1/73 disease-negative patients) for optic neuropathy due to cat scratch disease," they continued.
The authors were unable to explain, however, the four CSD cases that showed no optic nerve enhancement on MRI. "Consequently, a normal finding on an MR imaging examination does not exclude cat scratch disease as the cause of optic neuropathy," they noted.
The group also had little experience with other infections that can cause optic neuropathy, Schmalfuss stated. But in general, she suggested that their findings could prove helpful by distinguishing CSD-related optic neuropathy from other important causes.
"We saw such a unique distribution of the enhancement," Schmalfuss said. "It was always very localized to the optic nerve-disk junction."
"With MS in particular you usually have a long segment involvement, and we did not see it at all." Also, she noted, "none of our cat scratch disease patients actually had white-matter lesions."
Since submitting their article, the group has spotted another three patients with CSD-related optic neuropathy. "I think it's more common than you think," Schmalfuss said, "but you have to train your eye because some of the lesions are very subtle."
By Tracie L. Thompson
AuntMinnie.com staff writer
July 5, 2005
Related Reading
MRI findings unrelated to severity of MS course after onset of optic neuritis, September 29, 2004
Sophisticated MR techniques hone in on micro levels of MS, August 11, 2004
Brain lesion in optic neuritis linked with increased risk of MS, July 17, 2003
MRI may speed MS diagnosis, September 12, 2003
Fibrous dysplasia of the optic canal alone not associated with vision loss, November 22, 2002
Copyright © 2005 AuntMinnie.com