By comparing baseline and follow-up coronary calcium scores from PET/CT scans of lymphoma patients after chemotherapy, researchers say they can better follow the cancer treatment's debilitating impact on the heart, and perhaps get a better handle on possible cardiotoxicity.
The study from Saint Louis University would expand the utility of calcium scores beyond their traditional use for measuring coronary calcification to predict a person's risk of a future cardiac event. The new approach would also help evaluate the negative effects that calcium deposits caused by chemotherapy can have on coronary health.
"We are reporting that chemotherapy can accelerate coronary calcium deposition, particularly among patients with detectable calcium deposits at baseline scans, and may lead to an adverse cardiovascular reaction," said lead author and nuclear medicine resident Dr. Ahmed El-Sabbagh. "We are hoping to see if calcium score is an early detector for cardiotoxicity."
Calcium scoring's benefits
As previous research has shown, cardiotoxicity is one of the more serious adverse reactions to chemotherapy and can lead to a greater chance of morbidity and mortality. Cardiotoxicity due to chemotherapy most commonly comes from the anthracycline group, such as doxorubicin and idarubicin, frequently used in chemotherapy.
"A patient with pre-existing cardiovascular disease, including coronary atherosclerosis, shows an increased risk of heart failure after chemotherapy," El-Sabbagh said during a talk at this year's Society of Nuclear Medicine and Molecular Imaging (SNMMI) annual meeting. "It also is well-known that chemotherapy can cause deterioration in heart function."
Past studies have also shown that patients with high coronary calcium scores could develop additional cardiovascular issues such as renal artery stenosis and peripheral vascular disease. In all of those cases, subsequent treatment can be altered.
"So my colleagues and I decided to see how we measure calcium scores from the low-dose CT portion of a PET/CT scan and see if calcium score deterioration is an early indicator of cardiotoxicity," El-Sabbagh told AuntMinnie.com.
Lymphoma example
El-Sabbagh and colleagues randomly collected data from 89 lymphoma patients: 47 men and 42 women, ranging in age from 30 to 80 years. The subjects had received baseline and at least two postchemotherapy PET/CT scans within four years (± 1 year); subjects who had already undergone chest radiation therapy were excluded.
"We specifically chose lymphoma patients because these patients usually have baseline PET/CT before chemotherapy and subsequent PET/CT after chemotherapy to assess response to therapy," he said.
The researchers reviewed a total of 375 PET/CT scans and extracted calcium scores from coronary arteries using the low-dose (approximately 3 mSv) CT portion before and after chemotherapy.
They then divided the patients into five groups based on baseline calcium score:
- Score of 0 (62 patients, 70%), indicating no calcium deposition in coronary arteries and no cardiac risk
- Score of 1 to 10 (0 patients), indicating minimal atherosclerosis
- Score of 11 to 100 (4 patients, 4%), representing mild coronary atherosclerosis and coronary artery disease
- Score of 101 to 400 (10 patients, 11%), indicating the presence of moderate calcium deposits in coronary arteries and atherosclerotic plaque
- Score greater than 400 (13 patients, 15%), representing a significant risk of a cardiovascular event within the next five years
Calcium score gains
When reviewing the results for all 89 patients, the researchers found a statistically significant increase in coronary calcium scores after chemotherapy, with an average gain of 118% from baseline to the postchemotherapy results (p = 0.0124).
As one might expect, the 27 patients with calcium scores greater than 10 at baseline were most responsible for the statistically significant increase in calcium deposition due to chemotherapy (p = 0.025), with an average gain of 651% from baseline to the postchemotherapy results.
Among the 62 patients with no calcium deposition at baseline, there was no statistically significant increase in their calcium score after therapy (p = 0.147). The average gain in calcium score from baseline to the postchemotherapy results was 39%.
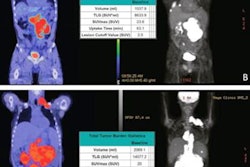
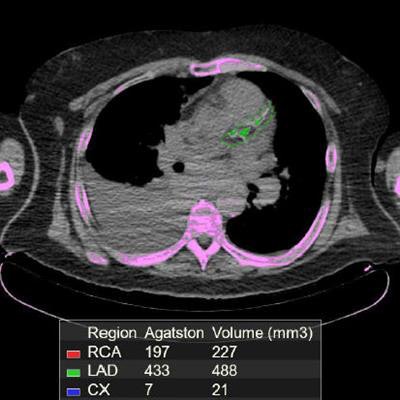
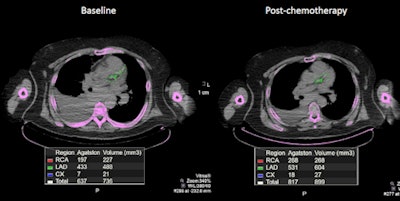 A 71-year-old man with non-Hodgkin's lymphoma had a total calcium score of 637 on his baseline PET/CT. When the scan was performed one year later after two cycles of chemotherapy, it showed a significant increase in calcium deposition and a calcium score of 817. Image courtesy of Dr. Ahmed El-Sabbagh.
A 71-year-old man with non-Hodgkin's lymphoma had a total calcium score of 637 on his baseline PET/CT. When the scan was performed one year later after two cycles of chemotherapy, it showed a significant increase in calcium deposition and a calcium score of 817. Image courtesy of Dr. Ahmed El-Sabbagh.Given the study's findings, oncologists and cardiologists at Saint Louis University are considering how to take advantage of coronary calcium scores generated by PET/CT scans. That information could be added to PET/CT reports to help evaluate the risk of cardiotoxicity in patients undergoing chemotherapy.
"We are now in an area where we talk to our oncologists and involve the cardiology group as well to see how best to evaluate a patient, based in part on the calcium score," El-Sabbagh said.
The usual standard of care is to order a baseline cardiac ejection fraction evaluation for a patient undergoing chemotherapy specifically with anthracyclines. After therapy, clinicians would perform a follow-up ejection fraction test, perhaps using echocardiography or multigated acquisition, to see if there is any deterioration.
The researchers also plan to continue this path by investigating the correlation between calcium score and left-ventricular ejection fraction to determine if calcium scores could serve as an early indication of deteriorating performance of the heart as it pumps blood out of the ventricles.
"Next we want to study the impact of incorporating calcium score in PET/CT reporting on patient management, whether an oncologist would change the chemotherapy choice, dosage, or form of therapy," added Dr. Medhat Osman, PhD, director of nuclear medicine.