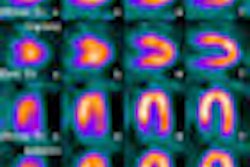
A new study concluded that myocardial perfusion imaging (MPI) is a significant predictor of sudden cardiac death and gated SPECT imaging may represent a more effective means of risk stratification than solitary left ventricular ejection fraction (LVEF) determination.
The study comes from the Duke Clinical Research Institute in Durham, NC, and the University of Alabama at Birmingham, with Duke's Dr. Jonathan Piccini as the lead author (Circulation, September 17, 2008).
While SPECT MPI has proven beneficial in the identification of patients at high risk of cardiovascular events and mortality, the researchers noted that it is still unclear whether the imaging technique "can identify patients with coronary artery disease at risk for de-novo sudden cardiac death."
The goal of the study was to determine if SPECT MPI could identify those patients and to determine if myocardial perfusion could provide incremental prognostic information to LVEF and clinical history.
Patient selection
The retrospective study reviewed 6,383 patients from the Duke Databank for Cardiovascular Disease from January 1993 to December 2006. Patients were confirmed for coronary artery disease, defined as greater than 75% stenosis of at least one major epicardial coronary artery. Researchers excluded patients with primary valvular heart disease, congenital heart disease, or an implantable cardioverter defibrillator, as well as patients who had undergone revascularization less than 60 days after SPECT MPI and if angiographic data were incomplete.
Exercise-capable patients underwent a treadmill stress test, while less mobile patients received a pharmacologic stress test. SPECT myocardial perfusion images were acquired using multihead detectors with 30 seconds per projection at rest and 20 seconds per projection during stress. The majority of patients (6,351, or 99%) underwent imaging with technetium-99m.
The researchers also took note of patients' age, gender, race, hypertension, diabetes, and history of heart failure, among other factors.
In a follow-up analysis of outcomes, 215 (3.4%) of the 6,383 patients with coronary artery disease died suddenly. Among those patients who died, the median time to sudden cardiac death was 2.7 years. The incidence of nonsudden death was 31.2%, or 1,992 patients, over a median follow-up of 6.1 years.
Age factors
The median age of those with sudden cardiac death was 62 years, and the median LVEF was 47%; 65% of patients with sudden cardiac death had an LVEF of greater than 40%. "As expected," the researchers wrote, "the incidence of sudden cardiac death was increased in patients with advanced heart failure."
The researchers found that age was not associated with an increased incidence of sudden cardiac death in this coronary artery disease population, and that cerebrovascular disease and peripheral vascular disease were "significantly associated" with increased risk of sudden cardiac death.
"SPECT myocardial perfusion defects are associated with increased all-cause mortality and cardiovascular death," Piccini and colleagues reported. "In this observational analysis of 6,383 patients with coronary artery disease, we have shown that impaired myocardial perfusion ... is also associated with an increased risk of sudden cardiac death."
The findings suggest that sudden cardiac death events are driven by both myocardial scar and ischemia, the researchers wrote.
Study limitations
Selection bias may have been a limitation of the study. While the researchers adjusted for pharmacotherapy, including beta-blockade and antiarrhythmic drugs at baseline, they "could not account for changes in pharmacotherapy over time," according to the study.
Another limitation was that LVEF determination "was not uniform and represented several imaging modalities, including angiography, SPECT, and echocardiography. Nonetheless, there was no association between the source of LVEF determination and sudden cardiac death in adjusted analysis."
Despite the limitations, the researchers concluded that with the large patient sample, the wide range of coronary artery disease, the prospective data collection, and the strict definition and adjudication of sudden cardiac death, the results "are not likely to be spurious."
"In this study, we show an association between impaired myocardial perfusion on SPECT imaging and the incidence of sudden cardiac death," they wrote. "Additionally, we have shown that impaired myocardial perfusion ... provides incremental prognostic information, beyond clinical characteristics and the LVEF among patients with ischemic heart disease."
Funding for the research was provided through a grant from GE Healthcare of Chalfont St. Giles, U.K.
By Wayne Forrest
AuntMinnie.com staff writer
September 26, 2008
Related Reading
Using coronary CTA first versus SPECT cuts costs, May 30, 2008
Study correlates CTA to angiography, myocardial perfusion SPECT, May 25, 2007
Stress MPI with Tc-99m SPECT identifies high-risk obese patients, September 1, 2006
PET, SPECT measures of LVEF have superior predictive value, March 13, 2006
SPECT MPI predicts cardiac danger in diabetics, January 14, 2002
Copyright © 2008 AuntMinnie.com