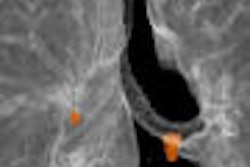
PET may be an expensive way to look at lung nodules, but it makes a lot of sense -- both clinically and economically -- in certain circumstances.
Overall PET is about 90% sensitive and 85% specific for detecting lung cancer in solitary pulmonary nodules, according to a meta-analysis of nine studies presented at the June International Symposium on Multidetector-Row CT. The meta-analysis was led by Dr. Andrew Quon, assistant professor of radiology at the Stanford University School of Medicine in Stanford, CA. The university sponsors the annual meeting in San Francisco.
The PET studies conducted throughout the 1990s relied mostly on an older generation of scanners that couldn't reliably evaluate solitary pulmonary nodules (SPNs) smaller than 10 mm, Quon noted.
Today's 16-slice PET/CT scanners can reliably find malignant SPNs in the 6-8 mm range, so the results from the newer machines are expected to be even better once their efficacy has been confirmed in large clinical trials, Quon said.
Already "there are some very good large studies, including one by (Dr.) Michael Gould at the VA Palo Alto, showing that PET is very cost-effective, and very beneficial to patient outcomes when you perform them on the right patients," he said. "And we have a pretty strong idea of who these patients are."
Once PET comes back positive on a suspicious nodule, it's time to go directly to tissue diagnosis in biopsy or surgery, he said. And although PET's high cost ensures that CT and radiography will remain the first-line lung cancer detection modalities for at least the near future, PET can be very useful adjunctively in patients whose diagnosis remains uncertain in the light of available radiographic and clinical evidence.
The PET decision should rely on two opinions: the clinician's and the radiologist's, Quon said.
First, based on the patient's clinical history (smoking, prior lung cancer, etc.) does the clinician believe the patient has a low, intermediate, or high risk of having lung cancer? Based on the CT appearance of the nodule, does the radiologist think the patient has a low, medium, or high risk of lung cancer?
"You should keep these two factors in mind before you pull the trigger on a PET," Quon said. "Once you have an overall gestalt on this patient, if you believe there is an intermediate or high risk of cancer, then you shouldn't do a PET scan -- you should just go ahead and get a biopsy, either percutaneous biopsy or surgical wedge resection," he said.
Pulling the trigger
There are some specific areas where PET can be extremely helpful. For example, if the lesion is at intermediate or high risk of cancer, but located in a very difficult spot to obtain a good biopsy percutaneously, a negative PET can be very helpful by pushing the management decision away from tissue diagnosis and toward watchful waiting, Quon said.
"On the other hand, if that lesion is positive (on PET), that would actually push you to be more aggressive in obtaining a definitive diagnosis rather than percutaneous biopsy by going right to resection," Quon said. "So in either scenario the PET can be helpful."
PET is also appropriate when the patient is uncomfortable with "watchful waiting" of a suspicious nodule, or alternatively, is averse to any kind of invasive procedure even though the CT looks suspicious.
"PET may be fairly helpful as a tiebreaker for those patients, to push them or assuage them into watchful waiting, or to getting a biopsy up front," Quon said. But the most important use of PET is when the CT and the clinical history are discordant, he said.
"Let's say you have a patient who has quite a bit of clinical risk, has a really bad clinical history that's really suspicious to your referring physician, but on the CT the lesion doesn't look very bad to you," he said. "Or the opposite can be true -- the patient had a nodule found, just a screening evaluation, very low risk." But the nodule looks suspicious, he said.
In the face of discordant evidence, there are good study results showing that PET is accurate, cost-effective, and very beneficial to the patient, Quon said.
Caveats and conclusions
Be wary of patients with a history of granulomatous disease or active infection -- they're a significant source of false positives, he said. Conversely, patients with bronchoalveolar carcinoma with mucinous features, and those with typical carcinoid tumors, have a false-negative rate as high as 50% with PET.
"So once you get this fancy PET scan, what do you do? When the PET scan is positive, that's fairly clear: go ahead and get the tissue diagnosis, either by the surgical incision or by percutaneous biopsy," Quon said. "However, when the PET scan is negative, you can go back to your tried-and-true algorithm of watchful waiting with interval CT or chest x-ray at six, 12, and 24 months. And it's certainly reasonable to do an additional PET scan perhaps at one of those other points as well."
Order a PET scan only if the clinician or patient will act on the results, advice that probably holds true for all radiology procedures, Quon said. CT is still going to be the mainline screening exam; PET is best used selectively in patients who have discordant diagnoses between clinical factors and CT results.
"Finally, the role of PET/CT is uncertain, but I believe -- this is my own speculation -- that you could probably start to evaluate nodules in the 7-10-mm range," Quon said.
By Eric Barnes
AuntMinnie.com staff writer
July 12, 2005
Related Reading
Report projects rapid PET procedure growth, July 6, 2005
PET/CT provides cost-savings for NSCLC radiotherapy, July 4, 2005
PET/CT demonstrates staging strength over PET, CT, and PET plus CT, March 7, 2005
Copyright © 2005 AuntMinnie.com