Venous stenting significantly reduced disease severity and improved quality of life in patients with post-thrombotic syndrome, according to a study presented April 13 at the Society of Interventional Radiology (SIR) 2026 annual meeting in Toronto.
The randomized, multicenter trial is the first prospective study to evaluate stent placement specifically for post-thrombotic syndrome (PTS), a debilitating long-term complication of deep vein thrombosis that affects deep vein thrombosis patients, noted principal investigator Suresh Vedantham, MD, of Washington University in St. Louis.
"Many patients with PTS suffer in silence because few physicians are aware of this complication or know how to effectively treat it. This study suggests that even severe PTS is, in fact, a treatable condition in many patients,” said Vedantham, in an SIR news release.
Each year approximately 600,000 Americans experience a deep vein thrombosis (DVT), with clots forming in veins that return blood from the limbs to the heart and lungs. PTS is a common, chronic complication occurring in up to 50% of patients within one to two years after a DVT. It results from damaged vein valves and persistent blockage, causing chronic pain, swelling, heaviness, and skin changes in the affected limb. Management primarily involves compression stockings and lifestyle adjustment.
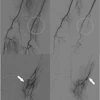
The study, known as Chronic Venous Thrombosis: Relief with Adjunctive Catheter-Directed Therapy (C-TRACT), compared two treatment strategies for PTS in a randomized, multicenter trial involving 225 patients with moderate to severe PTS across 29 institutions. Patients were randomized to either standard therapy alone -- anticoagulation plus compression --or standard therapy plus endovascular stent placement in blocked veins, performed predominantly by interventional radiologists.
At enrollment, 93% of patients had PTS classified as severe by the Venous Clinical Severity Score. At six months, only 40% of patients in the stent arm retained that severe classification, a shift Vedantham described as “remarkable” given how resistant severe PTS has historically been to treatment. Stented patients also reported significantly greater improvement in self-reported quality of life compared with controls.
PTS is frequently overlooked or mismanaged because many clinicians are unfamiliar with the complication or its treatment options, Vedantham added.
"Standard treatments such as anticoagulation and compression are important, but for many patients such treatments are not enough to improve leg symptoms and enable patients to function normally in their daily lives," Vedantham said. "C-TRACT shows that patients with moderate-to-severe PTS and large vein blockage could benefit greatly from endovascular stent treatment, so patients should consult with an interventional radiologist for proper evaluation and management."
The C-TRACT Trial received its primary support from the National Institutes of Health and additional support from the SIR Foundation. The trial was co-led by Washington University School of Medicine in St. Louis and McMaster University in Hamilton, Canada.