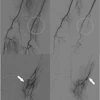
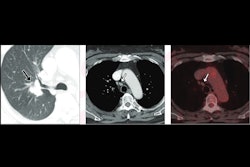
Interventional radiologists are disproportionately distributed in the U.S, with higher densities practicing near urban areas, according to a study published October 30 in the Journal of Vascular and Interventional Radiology.
“Almost 31.2% of the United States population does not have access to an interventional radiologist, however, many patients would prefer minimally invasive care,” wrote first author Yusuf Ahmad, a student at Lake Erie College of Osteopathic Medicine in Erie, PA, and colleagues.
Previous studies have shown unequal distributions of radiologists in the U.S., with less practicing in rural areas and more in counties with larger populations, higher average household incomes, and higher life expectancies, the authors explained.
Since interventional radiology is still a relatively nascent field, the distribution of interventional radiologists is not yet clear, they noted.
To that end, the researchers analyze the geographic distribution of 2,989 board-certified interventional radiologists in all cities within the U.S.
Interventional radiologists were found to be operating in just 15.5% (n = 487) of all U.S. counties. Of the 487 counties with interventional radiologists, 141 counties contained only one. The mean interventional radiologist per population ratio in the U.S. was calculated at 0.305 per 100,000 people, according to the findings.
In addition, the average median income among counties with interventional radiologists was greater at $67,649, compared with $53,528 among counties without interventional radiologists and an average of 31.3% of the population had a college degree in counties with interventional radiologists versus 20.3% in other counties.
Finally, the researchers found higher average percentages of African Americans, Pacific Islanders, and Hispanics in counties with interventional radiologists.
"By establishing standardized metrics and assessment tools, there will be a clearer understanding of the barriers that exist for different patient populations when it comes to accessing interventional radiology treatments,” the group wrote.
Ultimately, further work is needed to develop a framework for improving access to interventional radiology for patients, the group wrote. This includes assessing data on timeliness (e.g. travel time), workforce density, infrastructure (e.g. operating rooms, access to blood products), and affordability.
“These findings emphasize the need for a conversation surrounding interventional radiology care in rural settings and further exploration of specific socioeconomic variables pertaining to patients who have received interventional radiology care and how to better distribute that care to all,” the group concluded.
The full article can be found here.