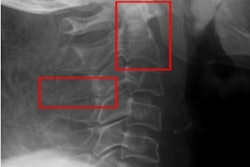
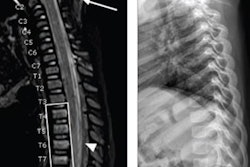
A new study supports the first-line role of cervical spine x-ray as a screening exam in pediatric blunt trauma patients.
The finding is from a 10-year review in which cervical spine (c-spine) x-ray screening had a sensitivity of 100% for clinically significant injuries, noted lead author William Starr, MD, of the University of Utah Health in Salt Lake City, and colleagues.
“Our study provides a large contemporary cohort where national c-spine protocols are followed showing a normal c-spine [x-ray] and a normal physical examination resulted in zero missed clinically significant injuries,” the group wrote. The study was published August 3 in Trauma Surgery & Acute Care Open.
Detection of pediatric c-spine injuries and the process by which cervical collars are removed is of the utmost importance, as missed injuries can be devastating, the authors explained. C-spine x-ray has been shown to be a valid screening tool for c-spine injury when coupled with a normal physical examination, and it is recommended by the Pediatric Trauma Society, they added.
“Despite these recommendations, [x-rays] have been abandoned as a screening tool at some institutions,” the group wrote.
Furthermore, the sensitivity and negative predictive value of c-spine x-rays have not been evaluated in a large, contemporary cohort of pediatric trauma patients, they noted.
Thus, the group conducted a retrospective review of cases at their level 1 pediatric trauma center from 2012 to 2021. The hospital’s protocol is to start with x-ray in patients with Glasgow Coma Scale (GCS) scores between 14 and 15 and then go to multidetector CT in patients with a depressed GCS score. The researchers compared a group with negative c-spine x-ray and no additional imaging to a group with negative c-spine x-ray followed by additional c-spine CT and/or MRI.
According to the results, out of 2,081 patients with negative x-rays, 1,974 (95%) had their c-spines cleared without additional imaging. The remaining 108 patients had additional c-spine imaging after negative c-spine x-ray for c-spine clearance (24 CT, 76 MRI, and 8 both CT and MRI). Indications for additional c-spine imaging were pain (48.1%), a GCS score ≤ 14 (43.5%), and paresthesia (8.3%), the researchers reported.
“In this cohort, screening [x-ray] had a sensitivity of 100% for clinically significant c-spine injuries,” they wrote.
Ultimately, although x-ray has been supported as a safe initial c-spine imaging modality for evaluable pediatric blunt trauma patients, its use remains a complex and debated topic, the authors noted. X-ray has been shown to be more cost-efficient, associated with increased quality of life, and to have a decreased radiation burden when used as the initial screening modality.
Meanwhile, in adult trauma, the utilization of x-ray has been almost completely replaced by CT, making c-spine x-ray a foreign test in many locations other than pediatric-specific centers, they wrote.
“As pediatric specialists, it is important that we continue to promote [x-ray] as an important tool in pediatric trauma,” the group concluded.
The full study is available here.