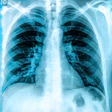
Philips Healthcare has received U.S. Food and Drug Administration (FDA) clearance for its MobileDiagnost wDR mobile digital radiography (DR) system.
The mobile system provides the same image quality as Philips' premium DigitalDiagnostDR rooms and includes a wireless portable detector with an ergonomic handle and a rubber case, Philips said. Images are acquired in just a few seconds and are sent wirelessly to the facility's PACS, according to the vendor.
MobileDiagnost wDR utilizes a 40-kW generator as well as Philips' Unified Image Quality Enhancement (UNIQUE) image processing algorithm and Eleva user interface.
UNIQUE and Eleva are also part of the new third release of the vendor's DigitalDiagnost system. In new features, the latest DigitalDiagnost provides for further customization of radiography rooms and the ability to scale from single, dual, or even triple detector systems depending on individual application requirements, room conditions, and budget flexibility, according to the vendor. Multiple table designs and vertical stands are also available.
In addition, DigitalDiagnost now includes a new tray that locks the wireless portable detector with just one click and automatically charges it, Philips said. Technologists can also use the wireless portable detector to take free exposures, such as with wheelchair patients. The detector has five amplimat chambers to reduce the risk of capturing incorrect exposures, according to the company.

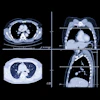
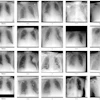



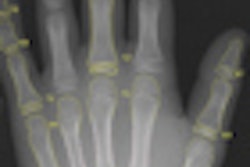





![Representative example of a 16-year-old male patient with underlying X-linked adrenoleukodystrophy. (A, B) Paired anteroposterior (AP) chest radiograph and dual-energy x-ray absorptiometry (DXA) report shows lumbar spine (L1 through L4) areal bone mineral density (BMD). The DXA report was reformatted for anonymization and improved readability. The patient had low BMD (Z score ≤ −2.0). (C) Model (chest radiography [CXR]–BMD) output shows the predicted raw BMD and Z score in comparison with the DXA reference standard, together with interpretability analyses using Shapley additive explanations (SHAP) and gradient-weighted class activation maps. The patient was classified as having low BMD, consistent with the reference standard. AM = age-matched, DEXA = dual-energy x-ray absorptiometry, RM2 = room 2, SNUH = Seoul National University Hospital, YA = young adult.](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/04/ai-children-bone-density.0snnf2EJjr.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)