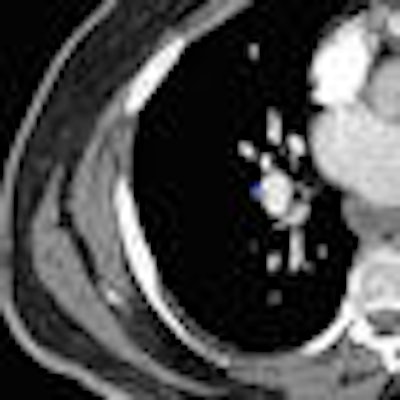
CT angiography (CTA) is an effective and reliable method for detecting pulmonary emboli, yet inexperienced readers may frequently miss filling defects when working alone or evaluating countless images under pressure. New research suggests that computer-aided detection (CAD) software could serve as a valuable surrogate second reader.
At this month's European Congress of Radiology (ECR), U.S. researchers presented a study evaluating the effects of a prototype CAD algorithm on the sensitivity of inexperienced readers for pulmonary emboli (PE) detection with CT angiography.
"We all know that during weekends and evenings, PE interpretation is mostly performed by junior/on-call residents, with no attending supervisor for consultation," noted Dr. Joseph Schoepf, director of CT research and development at the Medical University of South Carolina in Charleston. "However, missing PE in this initial phase is actually a common problem and has the potential to result in the mismanagement of patients."
His group asked two first-year residents inexperienced in reading cross-sectional CTA to mark vessels they thought contained a PE. Both were blinded to perform independent assessments of a randomized cohort comprising 41 CTA examinations clinically identified as positive for PE, plus 43 identified as negative.
A reference standard was provided by consensus of two expert radiologists, and all scans were deemed to be of adequate diagnostic quality.
Three months later (avoiding recall bias), the same first-year residents re-evaluated the same CTA images, this time aided by a prototype CAD system provided by Siemens Healthcare of Malvern, PA.
Consensus between expert readers revealed 294 PE (20 central, two lobar, 264 segmental, and eight subsegmental) in the group of 41 patients.
CAD doubles sensitivity
The researchers found that use of CAD nearly doubled the sensitivity of the inexperienced readers. On their first attempt, the inexperienced readers showed an average sensitivity of 23.13% on a per-PE basis. On their second attempt, using the CAD system as a detection prompt, sensitivity improved significantly to 45.24% (p < 0.001), while the number of false negatives fell by 33%, from 15 to 10.
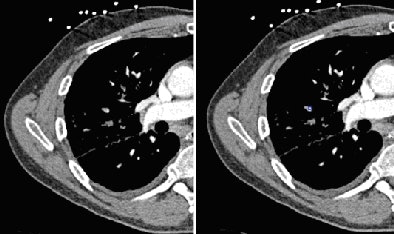 |
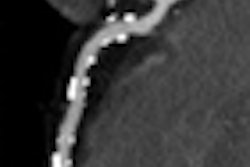
| Segmental embolus indicated by blue square (right image) -- PE was missed by both inexperienced readers upon initial interpretation (left image) without CAD as a second reader. All images courtesy of Dr. Joseph Schoepf. |
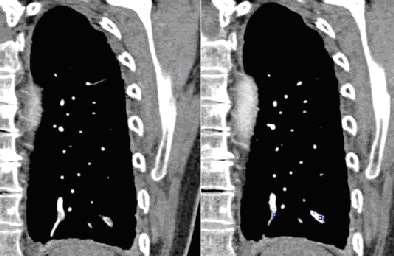 |
| Notice both medial and lateral subsegmental PE (bottom right) found by CAD but missed by inexperienced readers. |
The effectiveness of CAD in boosting sensitivity, however, depended to an extent on the location of the PE. Overall, its sensitivity averaged 82.65%, but sensitivity ranged notably from 90.15% (segmental) to just 5% (central). This principle also held true for the human readers.
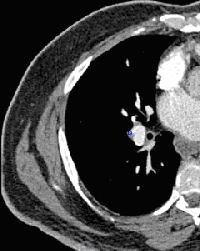 |
| CAD identifies a false positive on the pulmonary vein. |
In conclusion, Schoepf noted that adding CAD to the initial assessment by inexperienced CTA readers significantly improved sensitivity of PE detection, with a small but appreciable risk in the number of false positives.
He admitted, however, that the findings demand further research to better understand their implications.
"We need to see the downstream effect of such algorithms in terms of patient management, cost-effectiveness, and overall clinical outcomes: Are we creating additional risk by treating patients who don't require it?" Schoepf said. "And is that outweighed by detecting patients with PE who would otherwise have been missed?"
By Rob Skelding
AuntMinnie.com contributing writer
March 26, 2009
Related Reading
CT protocols reduce risk for pulmonary embolism, March 9, 2009
Lung CAD holds up well in low-dose MDCT studies, November 25, 2008
Researchers cut false positives in lung CAD, November 10, 2008
Experience may make a difference with lung CAD, February 4, 2008
Copyright © 2009 AuntMinnie.com