A new study from Korea found that radiologists reading chest studies on PACS workstations do just as well with standard-resolution computed radiography (CR) as they do with a high-resolution version of CR.
Most computed radiography studies are conducted with standard-resolution CR, generally defined as a 1760 x 2140 (2K) image matrix with 200-micron pixel size. In the late 1990s, high-resolution CR was introduced, featuring a 3520 x 4280 matrix with a 100-micron pixel size. CR readers equipped with a high-resolution capability can switch back and forth between the modes.
A number of research papers have examined the differences between standard-resolution CR and its high-resolution alternative based on technical criteria such as modulation transfer function (MTF), detective quantum efficiency (DQE), and noise power spectra. But a group from Inje University in Gimhae, South Korea, sought to determine whether there was a clinical difference as well -- namely, if the extra pixels translated into improved diagnostic accuracy for radiologists in a conventional PACS environment. Their analysis was published online in the Journal of Digital Imaging on December 27, 2006.
"Considering cost-effectiveness and access, it would be important to know whether the 4K images can actually achieve better diagnostic accuracy or not," the researchers stated.
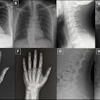
The group started with a patient population of 140 subjects, who received chest x-ray exams between January and December 2003. Forty patients were excluded from the study for various reasons, leaving a study population of 100. Abnormalities were classified in three groups: nodules (n = 15), pneumothorax (n = 14), and interstitial disease (n = 10). Sixty-one patients had no abnormality. The group tried to select cases with smaller or more subtle lesions, the researchers said.
Each patient was imaged first in 4K mode, then in 2K mode on a high-resolution CR reader (FCR-5501-HQ, Fujifilm Medical, Tokyo). The group used the following imaging parameters: 130 kVp, 1.25-mm nominal focus, 183-cm film-focus distance, 10:1 oscillating grid, and phototimed exposure.
Four board-certified radiologists read the images using a 5-megapixel monitor (2048 x 2560-pixel matrix) over the hospital's PACS network. The readers were not told of the pathologies on the images or whether they were from 2K or 4K studies, but they could discern the difference in resolution if they used the zoom option on the PACS software.
For each of the three categories of pathology, the readers rated the images on a five-point confidence scale, with 0 meaning the pathology was definitely absent and 4 indicating the pathology was definitely present. The accuracy of the readers' scores in detecting the three pathology types was then measured using the area under the receiver operating characteristic (ROC) curve (Az), and the ROC scores of the 2K images and 4K images were compared.
In most categories, the readers produced Az scores that either were identical or showed no statistical significance regardless of whether they read a 2K image or a 4K image. For example, in detecting pneumothorax, one radiologist showed a slight improvement in accuracy, with Az growing from 0.927 on the 2K image to 0.96 with the 4K image. But the other three radiologists showed no change in Az -- the average score for the four radiologists for pneumothorax detection was 0.954 for 2K images and 0.963 for 4K images.
For nodules, three of the observers performed better with 4K images, but the difference was not statistically significant. The average Az score for the group in nodule detection was 0.887 for 2K images and 0.894 for 4K images.
The results were similar in the detection of interstitial disease, with two of the radiologists performing better with 2K images and the other two performing better with 4K images. The average Az score for the group in interstitial disease detection was 0.867 for 2K images and 0.87 for 4K images.
In addition to diagnostic accuracy, the group measured the amount of time that the radiologists spent reading images. They found that review time was slightly longer for 4K images, with the group spending an average of 61.2 seconds reviewing 4K studies versus 59.6 seconds reviewing 2K studies, a difference that is statistically significant.
The researchers noted that the results were in line with previous studies on the technical characteristics of 2K versus 4K CR that concluded that high-resolution imaging did not produce a significant image-quality advantage over standard mode.
"We may conclude that the 2K mode would be sufficient for the detection of abnormalities on chest radiograph, and there is no considerable validity to incline toward the 4K mode in current PACS environment using a 2K monitor," they wrote.
By Brian Casey
AuntMinnie.com staff writer
January 22, 2007
Related Reading
Study: DR delivers lower radiation dose, November 7, 2006
U.S. hospitals find ways to take the digital x-ray plunge, October 12, 2006
Digital radiography slowly, but surely, makes its mark, July 25, 2006
Copyright © 2007 AuntMinnie.com