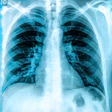
Every x-ray tech knows they should follow the "ALARA" principle when taking diagnostic images. It's important to keep radiation exposure "as low as reasonably achievable" -- especially in children.
Yet compared to film-screen systems, the design of many computed radiography (CR) and digital radiography (DR) systems makes it harder to gauge that exposure while simultaneously encouraging "exposure factor creep" to achieve great-looking images without retakes.
So what are the solutions to the conundrum? The manufacturers of CR and DR systems need to take responsibility for improved training of radiologic technologists, and also need to improve and standardize their presentation of exposure information.
That's the consensus view from the expert faculty of a 2004 ALARA conference sponsored by the Society for Pediatric Radiology (SPR). The conference, which was held in Houston and attended by 77 pediatric radiologists, medical physicists, radiologic technologists, and engineers, was also funded by unrestricted grants from six CR and DR vendors.
An overview of the conference findings and seven resulting recommendations was co-authored by Charles E. Willis, Ph.D., of Texas Children's Hospital in Houston, and Dr. Thomas L. Slovis from the Detroit Medical Center Children's Hospital.
Their report has been reprinted in both the February issues of Radiology and the American Journal of Roentgenology, having originally appeared in Pediatric Radiology (October 2004, Vol. 34, Suppl. 3, pp. S162-S164).
The ALARA principle is more important in pediatric exams, the authors note, because children "are roughly an order of magnitude more sensitive to radiation than middle-aged adults."
"Research indicates an increased risk of childhood acute lymphocytic leukemia from plain-film studies and an increased risk of fatal breast cancer from scoliosis series," the authors wrote. "The younger the patient at the time of exposure, the greater the risk of developing a fatal cancer."
But the advent of CR and DR has created the potential for "systematic overexposure" of young patients, the report states.
"The disconnection of acquisition from display in CR and DR allows these systems to compensate for variations in exposure factor by automatically rescaling the image to provide a relatively consistent appearance," the authors wrote.
"Faced with the prospect of repeating images, radiologic technologists tend toward overexposing. This phenomenon, so-called 'exposure factor creep,' has been documented in the CR literature."
Meanwhile, a technologist's desire to minimize dosages is also thwarted by the newer systems, the authors wrote.
"Almost every CR and DR system provides a derived numerical indicator of radiation dose," they noted. "Unfortunately, there is no standardization of the mathematical form or units of these indicators. The indicators depend on proper calibration of the acquisition systems, are subject to interferences, and require interpretation to translate into meaningful feedback for radiologic technologists."
"Without explicit guidance from the manufacturer, and without interpretable feedback from the acquisition system, CR and DR practitioners are free to develop exposure guidelines that violate the ALARA principle."
The authors credited "most" CR and DR manufacturers with developing special provisions for pediatric exams. Nonetheless, the recommendations developed by the conference faculty seemed to lay the burden for improvement on industry. (No vendors were named in the report at any point.)
The seven recommendations in the conference report are:
The use of a team approach to dose management in CR and DR, including "the active participation of a radiologist, medical physicist, radiologic technologist, biomedical engineer, manufacturer service engineer, manufacturer applications engineer, and manufacturer imaging scientist."
Improved training of radiologic technologists in CR and DR technology and practice.
"Disciplined" nomenclature within CR and DR technology, including the use of terms such as density, speed class, and sensitivity.
Standardization of dose indicators that are interpretable in real time. The report noted that a standardization proposal has been submitted to the Science Council of the American Association of Physicists in Medicine (AAPM).
Standardization of the nomenclature for digital image processing.
Automatic provision of "a number that represents the radiation dose expected at the detector in order to produce an adequate image."
Standardization in the use of ionizing radiation. This might include voluntary standards developed by a professional organization such as the SPR, the report noted, which could then be adopted as U.S. federal regulations, akin to the government's adoption of the American College of Radiology's mammography standards into the Mammography Quality Standards Act (MQSA).
By Tracie L. Thompson
AuntMinnie.com staff writer
February 4, 2005
Related Reading
Gonadal shield cuts scatter radiation from MDCT, January 10, 2005
Radiation burns 'often' iatrogenic -- UN, May 10, 2004
Use of pediatric head CT growing steadily in emergency departments, May 4, 2004
Constant image-noise standard lowers CT dose in pediatric exams, April 21, 2004
Pediatric CT won't stop growing, but dose can be minimized, May 8, 2003
Copyright © 2005 AuntMinnie.com

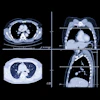
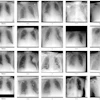







![Representative example of a 16-year-old male patient with underlying X-linked adrenoleukodystrophy. (A, B) Paired anteroposterior (AP) chest radiograph and dual-energy x-ray absorptiometry (DXA) report shows lumbar spine (L1 through L4) areal bone mineral density (BMD). The DXA report was reformatted for anonymization and improved readability. The patient had low BMD (Z score ≤ −2.0). (C) Model (chest radiography [CXR]–BMD) output shows the predicted raw BMD and Z score in comparison with the DXA reference standard, together with interpretability analyses using Shapley additive explanations (SHAP) and gradient-weighted class activation maps. The patient was classified as having low BMD, consistent with the reference standard. AM = age-matched, DEXA = dual-energy x-ray absorptiometry, RM2 = room 2, SNUH = Seoul National University Hospital, YA = young adult.](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/04/ai-children-bone-density.0snnf2EJjr.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)