Combined pulmonary fibrosis and emphysema (CPFE) fibrosis patterns identified on high-resolution CT may influence how quickly fibrosis will progress, but they don't necessarily predict long‑term survival, according to a study published February 24 in Radiology.
The findings suggest that although fibrosis patterns help clinicians anticipate CPFE trajectory and monitor the progression of the disease, treatment decisions should focus on fibrosis extent, wrote a team led by Min Seon Kim, MD, of Seoul National University Bundang Hospital in South Korea.
"Radiologic fibrosis patterns in [CPFE] were associated with the rate of fibrotic progression, whereas survival was primarily determined by baseline fibrosis extent and adverse clinical events, including lung cancer development," the group explained.
CPFE often presents with diverse radiologic patterns, and its impact on disease progression and clinical outcomes has not been well understood. To evaluate the effect of different fibrosis patterns on disease trajectory and outcomes in patients with CPFE, Kim and colleagues conducted a study that included 236 individuals who underwent high-resolution CT between January 2011 and December 2021. The team defined CPFE as emphysema (any subtype) involving at least 5% of total lung volume and fibrosis on CT. It classified radiologic fibrosis patterns in the following manner:
- Usual interstitial pneumonia (UIP) and/or probable UIP: n = 99, or 41.9%
- Nonspecific interstitial pneumonia (NSIP): n = 73 or 30.9%
- Smoking-related interstitial fibrosis (SRIF): n = 48, or 20.3%
- Desquamative interstitial pneumonia (DIP): n = 14, or 5.93%
- Unclassifiable pattern: n = two, or 0.85%
The researchers reported that radiologic fibrosis patterns were associated with the rate of fibrotic progression, which was fastest in usual interstitial pneumonia (median, 1.2 years), followed by nonspecific interstitial pneumonia (median, 2.1 years), and slowest in smoking-related interstitial fibrosis or desquamative interstitial pneumonia (median, three years). But these patterns were not significantly associated with the progression of emphysema (p = 0.27), lung transplant-free survival (p = 0.55), time-dependent lung cancer (p = 0.65), or acute exacerbation (i.e., sudden worsening of chronic lung disease; p = 0.64).
Kim and colleagues did find links, however, between greater baseline fibrosis extent, lung cancer, and acute exacerbation and worse survival (adjusted hazard ratio [HR]: 1.04, 3.9, and 4.31, respectively).
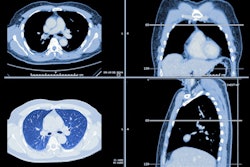
 Long-term fibrosis progression on serial unenhanced high-resolution chest CT scans in combined pulmonary fibrosis and emphysema with a smoking-related interstitial fibrosis pattern. Serial unenhanced high-resolution axial chest CT images in a 59-year-old man with a history of cigarette smoking (53 pack-years) demonstrate slow but long-term progression of fibrosis. (A) On baseline unenhanced axial chest CT scan, both readers classified the radiologic pattern as smoking-related interstitial fibrosis, which was confirmed with surgical biopsy. (B) Axial CT scan obtained at 1-year follow-up shows no radiologic progression. (C) Axial CT scan obtained at 4.7 years shows progression. (D) Follow-up axial CT scan obtained approximately 11 years after the baseline scan shows a marked increase in the extent of fibrosis with an increase in the size of irregular nonemphysematous cysts.RSNA
Long-term fibrosis progression on serial unenhanced high-resolution chest CT scans in combined pulmonary fibrosis and emphysema with a smoking-related interstitial fibrosis pattern. Serial unenhanced high-resolution axial chest CT images in a 59-year-old man with a history of cigarette smoking (53 pack-years) demonstrate slow but long-term progression of fibrosis. (A) On baseline unenhanced axial chest CT scan, both readers classified the radiologic pattern as smoking-related interstitial fibrosis, which was confirmed with surgical biopsy. (B) Axial CT scan obtained at 1-year follow-up shows no radiologic progression. (C) Axial CT scan obtained at 4.7 years shows progression. (D) Follow-up axial CT scan obtained approximately 11 years after the baseline scan shows a marked increase in the extent of fibrosis with an increase in the size of irregular nonemphysematous cysts.RSNA
While fibrosis pattern helps anticipate fibrotic progression, clinicians should rely more on assessing quantitative fibrosis burden via surveillance for lung cancer and acute exacerbations when managing CPFE patients, according to the authors.
"Although radiologic patterns offer information on the disease trajectory of fibrotic progression, comprehensive baseline quantitative assessment of fibrosis and emphysema, along with surveillance for subsequent adverse clinical events such as lung cancer, is essential for accurate risk stratification and long-term management in CPFE," they concluded.
Access the full study here.