Dynamic wide-area CT can easily distinguish two different but similar-appearing types of central airway narrowing that are hard to diagnose on conventional MDCT. Even a low-dose protocol captures the information reliably, according to researchers from China.
The radiology group from Hangzhou said image noise levels were much higher in the 80-kV protocol than with 100 kV, but diagnostic confidence was unchanged when diagnosing three patients with tracheomalacia and a larger group with central airway stenosis.
Results were presented earlier this month at the European Congress of Radiology (ECR) in Vienna.
Tracheomalacia is characterized by excessive airway collapsibility due to weakness of the airway walls and supporting cartilage, explained Dr. Zhong-Xiang Ding from Zhejiang Provincial People's Hospital.
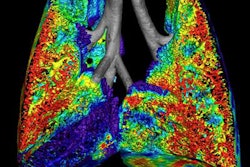
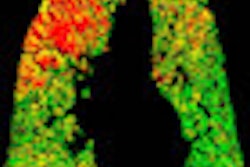
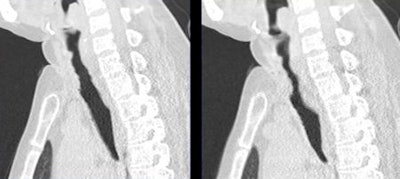 |
| Patient with tracheomalacia. All images courtesy of Dr. Zhong-Xiang Ding. |
"In clinical practice, a reduction of cross-sectional area more than 30% is a diagnostic standard for tracheomalacia, but routine CT has difficulty differentiating tracheomalacia from central airway stenosis," which is often caused by intubation of the patient, he said.
"640-slice dynamic volume CT covers a z-axis of 16 cm, and, more important, it can detect dynamic processes during the respiratory cycle," Ding said.
The study sought to differentiate tracheomalacia from stenosis using 640-slice dynamic volume CT. The group also compared the radiation dose and image quality of multiplanar reformation (MPR) and 3D reconstruction images of the central airways acquired at two different peak voltages, 80 kV and 100 kV.
In all, 16 patients with a body mass index less than 25 underwent 640-slice dynamic volume CT examinations (Aquilion One Vision Edition, Toshiba Medical Systems). Eight of the patients were scanned with the 100-kV protocol and eight were scanned using the 80-kV protocol at 320 x 0.5-mm collimation, 0.5-sec gantry rotation, and 50 mA.
The researchers measured expiratory time from maximal end-inspiration to the end of forceful exhalation, and image acquisition time was tailored to the expiratory cycle.
The group generated 3D images and MPRs from each expiratory phase. The 3D images were graded according to confidence level, ranging from 0 (lowest confidence) to 3 (highest confidence), while noise was assessed on the MPR images. Radiation doses were also calculated (CT dose index volume, dose-length product [DLP], and effective dose).
The acquisition times were approximately 5.1 seconds for the 100-kV protocol and 5.2 seconds for the 80-kV protocol.
"Central airway collapse was seen in three patients, and the remaining 13 subjects had stenosis," Ding said.
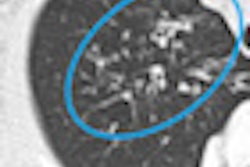
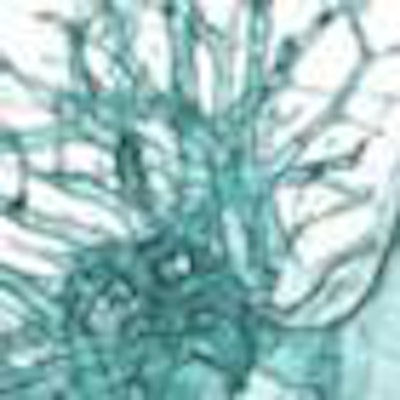
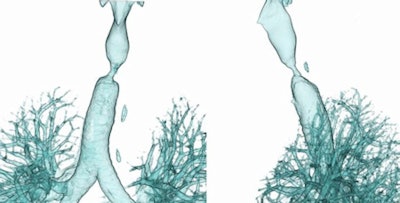 |
| Patient with central airway stenosis (not tracheomalacia). CT was performed three times: preoperatively, at one week after surgery, and at six months after surgery. Dynamic 3D images show that the central airway is stenosed before operation (above), and that stenosis persists a week after surgery (below) due to soft-tissue edema. However, six months after the operation (bottom image), the tracheal lumen is almost normal. |
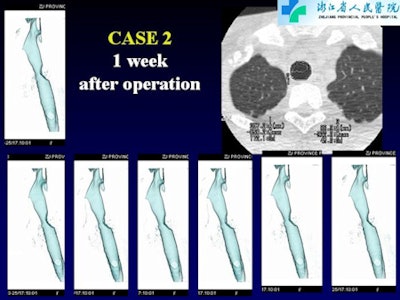 |
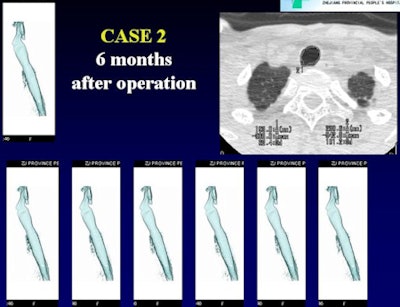 |
The level of confidence in tracheal lumen measurement was high (average score, 2.5; range, 1-3). Image noise was significantly higher for the 80-kV images; however, there was no significant difference in confidence level between the 80-kV and 100-kV protocols (p > 0.05).
Dose was far lower with the 80-kV protocol (DLP, 244.9 mGy-cm) than with the 100-kV protocol (DLP, 539.8 mGy-cm), the group reported.
"3D CT showed the dynamic process of the trachea during the respiratory cycle, and we can see the change in the lumen from end-inspiration to end-expiration showing stenosis," Ding said of an example from the study.
640-detector-row dynamic volume CT "is a promising method for differentiating tracheomalacia from central airway stenosis, and the 80-kV protocol performs as well as the 100-kV protocol in dynamic imaging of patients with small body mass index," he said.