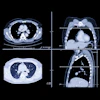
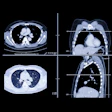
Histopathology data are uncommon in CT lung imaging studies, owing to the risks, costs, and high threshold of suspicion required to sample imaging findings. But a new study from researchers in South Korea got the goods on 53 ground-glass opacities (GGOs) in 49 patients who underwent resection or biopsy. The results yielded a majority of bronchoalveolar cell carcinomas, combined with other less common findings, according to the authors.
"Nonsolid pure ground-glass opacity (GGO) nodules, when persistently (either no change or an increase in diameter for ≥ 1 month) present on serial thin-section computed tomography (CT) scans, suggest the possibility of atypical adenomatous hyperplasia (AAH), bronchoalveolar cell carcinoma (BAC), pulmonary lymphoproliferative disorder, or organizing pneumonia/fibrosis," wrote Drs. Ha Young Kim, Young Mog Shim, Kyung Soo Lee, and colleagues from Sungkyunkwan University in Seoul (Radiology, October 2007, Vol. 245:1, pp. 267-275).
But the percentages in which the various findings occur are unknown, and the question of whether BAC can be distinguished from other findings also remains unanswered, they explained.
"According to one report, AAHs are less than 10 mm in diameter; however, others report that their diameters overlap those of BAC and AAH," Kim and colleagues wrote, noting that GGOs are also an important component of lymphoproliferative diseases and focal organizing pneumonia/fibrosis. Finally, few reports are available for multiple pulmonary nodules, and the authors did not exclude such cases from their retrospective evaluation.
"Thus, the purpose of our study was to retrospectively compare pure pulmonary GGO nodules observed on thin-section CT images with histopathologic findings," they wrote.
The researchers began by searching all biopsy files from their facility between 1994 and 2006, looking for the descriptive term "GGO nodule," and assessing patient demographics for analysis, they explained.
GGO nodules were defined as discrete pulmonary abnormalities 3 cm or smaller, with homogeneous attenuation lower than that of surrounding soft-tissue structures such as blood vessels. The study included 49 patients with persistent GGOs lasting more than a month on CT.
Images were acquired on several HiSpeed and LightSpeed series scanners (GE Healthcare, Chalfont St. Giles, U.K.) including eight patients on the single-slice machine, 24 on a four-detector-row scanner, 12 patients on an eight-detector-row scanner, and five patients on a 16-detector-row LightSpeed 16 model.
Scan parameters included 120 kVp and 70-200 mAs on all patients, and 7-mm section thicknesses. Reconstruction intervals were 2.5-5.0 mm for four- to 16-detector-row scanners. On the single-slice cases, additional thin-section images (1.0-2.5 mm) were obtained from GGO nodules; for the four- to 16-slice scanners, additional thin-section reconstructions (1.25-2.5 mm) were acquired from the source data, according to Kim and colleagues. Forty-one patients had both unenhanced and contrast-enhanced scans, while eight underwent unenhanced scans only.
All images were reconstructed using a bone algorithm and viewed on a PACS (GE Centricity 2.0) by two experienced chest radiologists, the authors noted. The mean time for CT-pathologic comparison was eight days, with a range of 0-49 days.
The results showed 53 nodules in 49 patients (20 men, 29 women; mean age 54 years, range 29-78). A total of 40 of the 53 (n = 36, 75%) were proved to be BAC or adenocarcinoma with a predominant BAC component (n = 4). There were also three (6%) AAHs and 10 (19%) cases of nonspecific fibrosis or organizing pneumonia.
"Multiple nodules were demonstrated in 22% (eight of 36) of BAC or adenocarcinoma with predominant BAC component, 67% (two of three) of AAH, and 20% (two of 10) of nonspecific fibrosis or organizing pneumonia patients (p = 0.21)," the authors wrote. As for symptoms, 10 (20%) of 49 patients had symptoms such as chest pain, cough, or blood-tinged sputum; symptomatic patients constituted 90% of patients with BAC or adenocarcinoma with a BAC component.
Follow-up CT over a mean of 10 months showed size increases of more than 5 mm in two patients, one with BAC and another with chronic inflammation, Kim and colleagues noted.
The mean size values, consisting of maximum diameter ± standard deviation, were 13 mm ± 6.9 mm for BAC or adenocarcinoma with a predominant BAC component, 8 mm ± 3.8 for AAH, and 12 mm ± 6.7 for nonspecific fibrosis or organizing pneumonia patients (p ≥ 0.99). The mean CT attenuation values were -499 HU ± 171.6 for BAC and adenocarcinoma with a predominant BAC component, -667.3 HU ± 62.1 for AAH, and -554.6 HU ± 165.2 for nonspecific fibrosis and organizing pneumonia.
Morphology including shape, margin characteristics, internal characteristics, and presence of pleural tag were not significantly different among the different conditions diagnosed (all p > 0.05). Nor did the team find significant differences in sex (p > 0.99) or age (p = 0.58) between BAC or adenocarcinoma with a BAC component, AAH, or nonspecific organizing pneumonia.
Several previous studies have sought to apply discriminative imaging findings; however, no such correlations were seen in the present study, the authors wrote. For example, Furuya et al asserted that a tentacled or polygonal margin indicated a benign inflammatory nodule in up to 80% of cases. But the present study showed no significant morphologic differences between BAC and adenocarcinoma with a BAC component, and the other conditions diagnosed.
Polygonal shape and lobulated or spiculated margin were found in two (20%) and three (30%) of 10 nodules, respectively, in organizing pneumonia/fibrosis, caused by "granulation tissue aligned in a linear manner in perilobular regions with or without interlobular septal thickening ... thus simulating septal thickening and contributing to a coarse reticular pattern with or without interlobular septal thickening," the group wrote.
Selection bias was a principal limitation because only patients who underwent surgery or biopsy were included, the authors noted. "This may explain why, when compared with previous reports, our study contains a relatively small percentage of AAH (6%) and no cases of lymphoproliferative malignancy," they stated, adding that data clustering due to patients with multiple nodules may represent another limitation.
"About 75% of pure persistent pulmonary GGO nodules turn out to be BAC or adenocarcinoma with predominant BAC component, and these do not manifest distinguishing morphologic features on thin-section CT images that allow their differentiation from other GGO nodules with different histopathologic diagnoses," Kim and colleagues concluded.
By Eric Barnes
AuntMinnie.com staff writer
October 22, 2007
Related Reading
Ground-glass lung nodules need extra scrutiny, August 22, 2007
Divergent research on CT lung screening sparks more debate, fewer answers, April 19, 2007
Ultralow-dose lung MDCT may still find ground-glass lesions, November 30, 2005
Emphysema alters CT appearance of benign nodules, May 4, 2005
Copyright © 2007 AuntMinnie.com