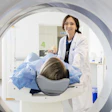
SAN FRANCISCO - Dr. Gene Hern uses a brand-new multislice CT scanner at Highland Hospital's brand-new trauma center in Oakland, CA. It can scan a trauma patient head to toe in 45 seconds, and frequently does. But is trauma CT being overused, or used for the wrong indications?
At a talk on Wednesday at the American College of Emergency Physicians (ACEP) annual meeting, Hern led a whirlwind tour of CT in the trauma setting, building a set of evidence-based recommendations.
CT didn't earn its popularity on its looks. It's an incredibly sensitive test that can quickly assess what other modalities and the physical exam frequently miss, Hern said. But it carries risks of too much radiation, and of overuse in low-risk indications for which the best studies indicate that CT is unnecessary.
"We'll talk about pan-scanning versus physical exam and observation," he said. "How diagnostic is our physical exam in significant trauma? Is there such a thing as a quick look? Frequently the surgeons will take a case to the CT scanner even though they're going to the (operating room) anyway. Is there a role for that?"
CT is highly sensitive in the assessment of many trauma injuries -- in fact, it frequently "finds more disease than we want to know about," said Hern, who is an assistant clinical professor of medicine at the University of California, San Francisco, and associate residency director at the department of emergency medicine at ACMC-Highland General Hospital in Oakland.
CT also finds disease that requires intervention and changes in patient management. The challenge is to nail down the applications in which the probability of significant findings is high enough to justify the expense and radiation risk, according to Hern.
"From a philosophical standpoint, how sensitive do we want our tests to be? What is our tolerance of risk? Do we have to actually get every single diagnosis, or are there a couple that we can miss? I think our trauma surgeons have a much lower risk of tolerance than we do, they tend to scan everyone, and that's part of the hierarchical argument and standpoint coming from that department," Hern said.
Head trauma
CT has an obvious benefit in severe (Glasgow Coma Scale or GCS 3-8) and moderate (GCS 9-12) head injury, Horn said. However, 75% to 80% of all trauma patients fall into the mild head trauma category (GCS 13-15), and routine CT has been highly controversial in this largest category of patients.
Patients in the moderate category have a very large chance of deteriorating, and need very close observation; 10% progress to coma. Among the mildly injured patients, those with GCS 13 tend to have very poor outcomes, he said. For this reason, it's often better to categorize head trauma patients into low, medium, and high risk rather than going by the numbers.
As for serious head injury, the rate of serious head injury requiring surgical intervention is not insignificant -- 3% to 4% in some large studies, he said (Stein et al, Journal of Trauma, July 1992, Vol. 33:1, pp. 11-13; Shackford et al, Journal of Trauma, September 1992, Vol. 33:3, pp. 385-394).
Even patients at low risk can have significant injuries, he said, although there is undoubtedly some selection bias at work. "These patients have been activated into the trauma system, and so there is a higher instance of their being ill," Hern said.
A study by Haydel et al indicated a number of high-risk features indicative of a positive head CT, including age greater than 65 years, vomiting, drug and alcohol intoxication, short-term memory deficits, seizures, signs of trauma above the clavicles, and seizure. Median risk factors included failure to reach GCS 15 within two hours, asymmetric pupils, and a dangerous mechanism of injury. "For the evaluation of patients with minor head injury, the use of CT can be safely limited to those who have certain clinical findings," the authors concluded (New England Journal of Medicine, July 13, 2000, Vol. 323, pp. 100-105).
Finally, trauma physicians are eager to see the upcoming results of the National Emergency X-ray Utilization Study II (NEXUS II), a multicenter prospective observational study of all ED patients for whom CT was ordered by the examining clinician. This study should provide definitive information on a large number of trauma head patients.
Applying these criteria can help ED physicians decide when to send low-risk patients home, Hern said.
Spinal trauma
"Spine trauma is interesting in that it is an area that is very difficult to image -- yet a high proportion of x-rays in the ED are actually C-spine x-rays," Hern said. But since CT is very sensitive, should x-rays even be continued?
Plain films are clearly inadequate. In patients with a C-collar, the lateral-view x-rays are inadequate 25% of the time. Also, positioning the patients is often difficult and risky, and patients may be uncooperative.
On the other hand, CT can quickly evaluate bony fragments, herniation, and hematoma. CT is fast, and can generally be done without moving the patient a great deal. And unlike x-ray, CT can easily evaluate patients who are intubated.
Trauma organizations, including the Eastern Association for the Surgery of Trauma (EAST), recommend the acquisition of axial CT images through the C1 and C2 vertebrae anytime trauma head CT is acquired. A study by Schenarts et al supporting the EAST decision found that plain film had only 54% sensitivity for cervical spine injury, versus 96% for CT, Hern said (Journal of Trauma, October 2001, Vol. 51:4, pp. 663-668).
"It's clear that (CT) is a much more sensitive test," Hern said. "The question is, are there areas where we can eliminate CT scans?"
"The NEXUS I study had over 34,000 patients in its derivation group. The low-risk criteria required that patients be awake and alert, and have a GCS of 15. Such patients had no midline tenderness, no distracting injuries, no neural deficits, and were not intoxicated.
The Canadian C-spine rule predicted risk better than NEXUS I criteria. The Canadian high-risk criteria include patients over 65 years of age, presence of parathesius, or a dangerous mechanism of injury including a fall greater than 3 feet or five stairs, or a motor vehicle accident at greater than 60 mph, or rollover or ejection in an accident, Hern said.
If none of these were present, range-of-motion criteria could be queried, such as whether the patient walked at the scene of the injury, or had midline tenderness or limited neck motion that could be indicative of greater risk (New England Journal of Medicine, December 25, 2003, Vol. 349:26, pp. 2510-2518).
By these criteria, lower-risk patients can be safely shunted out of the emergency system, Hern said.
Lower in the spine, CT also has greater sensitivity than plain films. For example, Brandt et al reported that 13/47 fractures were seen on CT but not plain films; Sheridan et al found 19 thoracic fractures, seven of which were picked up only on CT; and 27 lumbar fractures, two of which were picked up on CT alone, he said (Journal of Trauma, May 2004, Vol. 56:5, pp. 1022-1026; Journal of Trauma, October 2003, Vol. 55:4, pp. 665-669).
Chest trauma
It turns out the physical exam is not very good. It is clear that doctors cannot pick up as many chest injuries as they thought they could. The sensitivity of physical exam for pneumonia, for example, is far less than 50%.
"While some may decry the lack of training in physical exam skills, one might also say that our skills weren't very good to begin with," Hern said.
Plain films miss significant chest injuries. Surgeries have been required in the range of 40% of chest-injury patients whose plain films were negative, he said. However, that doesn't mean that all these people need angiography as well, especially if they undergo CT on a multislice scanner.
Aortic injuries, often caused by severe deceleration, demonstrate no external signs of trauma in one-third to one-half of patients. Physical exam is insensitive. A widening mediastinum has been used successfully to gauge such injuries on plain film; however, the sensitivity is about 50%.
There are other causes of mediastinal widening, include venous bleeding from the top of a fracture, pulmonary contusions, a previous mediastinal mass, or magnification caused by the AP view, he said. But rather than measuring width, it turns out trauma surgeons can gauge mediastinal abnormalities much better in plain films when they rely on their instincts, he said.
Still, the abysmal negative predictive value of a plain chest film is well-documented, he said. Up to 44% of patients with a proven aortic rupture have a normal mediastinum on chest x-ray (Archives of Surgery, October 1998, Vol. 133:10, pp. 1084-1088).
Occult pneumothorax, often seen on CT but missed on plain film, has been shown to be clinically unimportant in general, and tube placement is often avoided.
A number of studies have demonstrated the superiority of CT over plain film. Among them, Trupka et al examined 103 consecutive blunt trauma patients who had both chest x-ray and CT. Sixty-seven of the patients received a new diagnosis as a result of CT, and a change in management occurred in 42 patients (Journal of Trauma, September 1997, Vol. 43:3, pp. 405-411).
"The bottom line in chest trauma: If the patient has a high-risk mechanism (of injury), I think it's important that we CT the chest," Hern said. "I think it's clear and well-documented in the trauma literature, at least, that those patients are going to have further injuries.... Plain films will miss some of the injuries, and plain films will actually miss some of the interventions, including aortic surgeries or chest tube (placement)."
Abdominal trauma
CT has become the primary diagnostic tool in abdominal trauma, and its routine use is far less controversial than chest imaging. CT has been shown to be highly accurate (92% to 97% sensitivity, 98% specificity) for the detection of abdominal injuries, and often provides unexpected additional diagnoses.
CT has also paved the way to noninvasive management of a number of intra-abdominal injuries. CT scans also decrease negative laparotomy rates, and can readily determine the presence, source, and quantity of intraperitoneal blood. Where ultrasound could reliably detect peritoneal blood, it was far less accurate in ferreting out its location, source, and quantity. And unlike ultrasound, CT is highly sensitive for the detection of solid organ injuries, Hern said.
CT does have its disadvantages, including poor visualization of the pancreas and diaphragm, small bowel, and mesentery. Also, if the CT scanner is located away from the emergency room, the acutely injured patient may have to be out of sight of the ED for longer than the physicians are comfortable with.
What about "quick look" CT studies for patients headed to the operating room anyway? They can make sense if the scanner is close to the ED, and is a fast multislice scanner.
"But it is clearly not going to be advisable when the patient is unstable, or supervision is difficult," he said.
Other issues
A full-body scan can be helpful in revealing additional findings, Hern said. A retrospective study found that of 457/660 patients who had chest, abdomen, and pelvic scans, 48.5% had positive CT scans, 38% showed unexpected findings, and 26% a change in management (American Journal of Surgery, December 2003, Vol. 186:6, pp. 609-614).
IV contrast is often very helpful in evaluating trauma patients, especially when the subtle details of vasculature are needed for diagnosis. It is probably not necessary to wait for creatinine results before scanning, Hern said. In cases of known renal insufficiency, nonionic contrast agents have been shown to yield good results. Rectal contrast is not helpful, he said. In his institution it has been found to be difficult to administer, adding unnecessary delays to the examination.
Radiation dose is a significant concern in CT, he said. CT exams account for only 13% of imaging studies, but 70% of all radiation. Among the studies he cited, 3,094 men who had received radiation for cutaneous hemangioma before age 18 showed significant differences in academic performance that were dose-related, and unrelated to socioeconomic status or other factors (British Medical Journal, January 3, 2004, Vol. 328:19). Radiation to the thyroid is of particular concern in pediatric head imaging.
"The bottom line is that previous techniques before CT evaluation of trauma were not very helpful," Hern said. "What's probably more important for us in the emergency department is to try to eliminate diagnostic testing in those patients that we feel are in a low-risk category. We can use our head injury rules, we can use our C-spine rules, and actually shunt patients out of the trauma system, and thereby eliminate diagnostic testing."
But if the patient is sick enough, that's when CT is the test of choice for many injuries due to its incredible sensitivity, he said. For many applications, CT will remain the test of choice for many high-risk patients, as long as they are hemodynamically stable. In 10 years, he predicted, chest and spine films will be a thing of the past.
By Eric Barnes
AuntMinnie.com staff writer
October 21, 2004
Related Reading
Hospital finds cheaper facial imaging with CT versus x-ray, September 22, 2004
CT: An all-star modality for C-spine trauma?, August 18, 2004
MDCT drives important changes in U.K. healthcare, August 10, 2004
CT scan after isolated loss of consciousness may not be necessary, June 17, 2004
CT can reduce unneeded laparotomy for patients with gunshot wounds, May 21, 2004
CT shows lab tests fail to predict pediatric trauma, May 6, 2004
Use of pediatric head CT growing steadily in emergency departments, May 4, 2004
Copyright © 2004 AuntMinnie.com