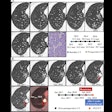
A new study reports high per-patient sensitivity and specificity for virtual colonoscopy using second-look conventional colonoscopy as a reference standard. The virtual exam missed plenty of lesions -- due largely to poor prep or inadequate colonic distension -- but still managed to identify 98% of the patients who needed follow-up exams.
"A major strength of the present study is its use of unblinding to allow second-look conventional colonoscopy for clarification of discrepant results," wrote Dr. Hanno Hoppe, Dr. Peter Netzer, Dr. Adrian Spreng, and colleagues from Inselspital and the University of Bern in Switzerland (American Journal of Gastroenterology, October 2004, Vol. 99, pp. 1924-1935).
The study is the second paper published in the past month to rely on segmental unblinding of VC results after first-pass conventional colonoscopy. Study data by Pickhardt et al was previously re-examined in this manner to yield a better understanding of VC's sensitivity for the detection of colonic neoplasia.
Segmental unblinding requires that VC results be unveiled for each colonic segment immediately after colonoscopic examination of the segment. If VC results are positive but colonoscopy is negative for a particular segment, the colonoscope is reinserted into the segment for a second look. The technique not only picks up lesions colonoscopy may have missed the first time around, but ensures the accuracy of the reference standard by verifying whether the original VC findings were true- or false-positive.
Hoppe and colleagues examined 100 adults referred for conventional colonoscopy, who were recruited for the addition of virtual colonoscopy to the protocol. The patients (62 men, 38 women age 21-91, mean age 66) were all referred for indications including hemoatochezia, positive fecal occult blood test, anemia, and personal or family history of colorectal lesions.
The day before virtual and conventional colonoscopy, the subjects underwent purgative bowel cleansing after ingesting 4 L of a methylcellulose solution. Just before CT imaging, the bowel was insufflated manually with room air to patient tolerance. And except for 24 patients who were contraindicated for the use of contrast, the cohort received 300 mg/mL of iopromide (Ultravist 300, Berlex Laboratories, Montvale, NJ) power-injected at 3 mL/sec, with a scan delay of 60 seconds.
Patients underwent prone and supine imaging of the abdomen and pelvis on a four-detector CT scanner (Asteion, Toshiba America Medical Systems, Tustin, CA) at 200 mAs, 120 kVp, and 4 x 2-mm collimation. Pitch was 1.375, rotation speed 0.75 sec, and the axial CT data were reconstructed at 2 mm with 1-mm intervals. Both 2D and 3D endoluminal images were reviewed on an Advantage Windows Workstation (Version 4, GE Healthcare, Waukesha, WI).
The three interpreting radiologists had each read between 30 and 60 virtual colonoscopy exams before the study began.
"The supine and prone datasets were viewed as continuous 2-mm axial sections with a high-contrast window display setting (width 2000 H, level 0 H), which was chosen to provide high contrast for polyp detection," the authors wrote. "For confirmation of polyps, the window setting was changed.... When an abnormality or a suspicious lesion was detected on axial CT ... additional views were evaluated to ascertain the morphologic features of the lesion. If no abnormality was seen or suspected at axial image review, no further image processing was performed." Different window and level settings were used to examine the internal attenuation of suspected polyps in an effort to distinguish stool or colonic folds from polyps, they added.
Conventional colonoscopy using the second-look technique was performed immediately after the virtual exam, with all resected polyps submitted for histologic examination. In all, 94/100 conventional exams reached the cecum, and four of the remaining patients underwent only VC. Two other patients were excluded due to inadequate bowel prep.
The results in 92 patients who successfully underwent both exams showed that conventional colonoscopy found 122 lesions, including eight carcinomas (one rectal, four sigmoid, one ascending colon, two cecal) in 49 patients. Sixty-three polyps were 5 mm or smaller, 28 ranged from 6-9 mm, and 31 were 10 mm and larger, including seven carcinomas, 17 adenomas, and seven hyperplastic mucosa.
Second-look conventional colonoscopy revealed what appeared to be two false-negative VC results, as well as two false-negative conventional colonoscopy results, consisting of a 6- and an 8-mm polyp. Compared to second-look conventional colonoscopy, VC's overall sensitivity for detecting patients with at least one polyp 6 mm or larger was 76%, with specificity of 88%.
For the detection of lesions 10 mm and larger, VC was 95% sensitive and 98% specific per patient. Per-polyp sensitivity was 71% for lesions 10 mm and larger, and 61% for lesions 6-9 mm. VC missed a single 7-mm carcinoma in the ascending colon, which was detected by the conventional exam.
"CT colonography (VC) demonstrated 65 false-positive polyps using by-polyp matching," the researchers wrote. "Seven polyps were 10 mm or larger, 25 were 6-9 mm, and 33 were 5 mm or smaller. Thirty-nine of the 65 false-positive polyps 10 mm or larger were found in colonic segments that were poorly distended or poorly prepared. Ten ... lesions (3-9 mm) were false-positive due to angiodysplasia of the colon, which mimic polypoid lesions on (VC)."
In addition, four false-positive lesions on VC were judged at colonoscopy to be mucosal pseudopolyps due to ulcerative colitis. And among the six patients excluded due to failed colonoscopy as a reference standard, VC found an 18-mm lesion in the cecum and a 13-mm lesion in the ascending colon, the authors stated.
"If the results of the present symptomatic population were transferred to a screening population, 50% of the polyps sized between 6-9 mm could not be detected with (VC)," the authors wrote. "This would necessitate repeat screening exams within approximately three to five years compared to conventional colonoscopic screening every 10 years," increasing cost and radiation, they wrote.
Still, the authors noted that a large study of asymptomatic patients by Pickhardt et al yielded comparable sensitivities for the two exams in the same 6-9-mm range (New England Journal of Medicine, December 4, 2003, Vol. 349:23, pp. 2191-2200).
Hoppe and colleagues also emphasized that 40/70 missed lesions on VC were in poorly prepared segments. The authors cited motion artifacts and inadequate bowel cleansing as additional causes of missed lesions and false-positives.
"This underlines the importance of proper bowel cleansing and the application of techniques employing fluid and stool-tagging agents, which allows digital subtraction of residual material from images," they wrote. The use of intravenous contrast in VC may increase specificity, they added, but the associated costs and risks probably exclude its use in screening of large populations.
"CT colonography was found to have both high by-patient sensitivity and specificity for detection of clinically important colorectal neoplasms," the authors wrote. "This suggests that CT colonography has the potential to become a valuable clinical screening method for colorectal neoplasms."
By Eric Barnes
AuntMinnie.com staff writer
October 4, 2004
Related Reading
VC fares better as its own gold standard, September 8, 2004
What virtual colonoscopy misses might not matter, August 18, 2004
Group credits 3-D reading for best-ever VC results, October 15, 2003
Virtual colon dissection is promising, if flawed, July 9, 2003
Multiobserver performance trial assesses utility of screening VC, November 27, 2002
Copyright © 2004 AuntMinnie.com