AuntMinnie.com is pleased to present the fifth in an ongoing series of practice management articles contributed by the Radiology Consulting Group in Boston. This twice-monthly series addresses topics and issues of concern to radiology administrators and business managers.
By Ronald Doncaster, senior consultantRadiology Consulting Group

The approach has yielded both qualitative and quantitative results. Once an adversarial, frantic, and reactive culture, the relationship between the two departments is now built on cooperation, collaboration, and trust. As a result, the two groups have been able to achieve significant, sustained reductions in patient throughput time and an improvement in the patient experience.
By leveraging technology (PACS and Web-based image distribution), systems thinking, and continuously challenging each other to work together and improve, patient throughput time has been reduced by more than 34%. In addition, the improvements contributed significantly to an overall film cost savings of $1 million (U.S.).
So how did MGH do it? Key stakeholders from both departments formed a radiology and orthopedic task force. The main credo of the group was the following: If a patient has a bad experience in either department, in the end, it is the patient and the hospital that suffer.
The task force consisted of a physician champion from each department, operations managers, and members of the radiology quality management division. Tactically, the task force employed the following steps:
- Defining the problem
- Identifying the goal
- Using the available tools
- Analyzing the results
- Focusing intensely on sustainment
- Planning for the future
Defining the problem
The strategic barrier to success, as in most healthcare systems, has been that both radiology and orthopedics provide patient care independent of the other. Yet the departments are interdependent. The radiology department depends on orthopedics’ referrals, while orthopedics needs radiology's images and diagnoses.
Neither department focused on -- or even considered -- the patient’s experience in the other’s department. The operations and relationship could be described as independent silos within the walls of one physical institution.
The tactical problem was that patients had significant wait times in both departments, and the patient experience was typically frustrating. In today’s competitive healthcare market, this could impact the profitability of the institution.
The agreed-upon goal, decided at the first meeting of the task force, was to reduce patient throughput time. To reach that goal, however, the two groups needed to look carefully at the continuum of care provided throughout the entire system.
The process
In an effort to improve patient care, the radiology department began a phased-in approach to incorporate both PACS and computed radiography (CR). The initial entry point for CR was the ambulatory outpatient diagnostic radiology division -- where orthopedics is the biggest referrer.
As radiology learned about the benefits and possibilities of Web-based image distribution, collaboration with the orthopedics department became critical. Some of the issues addressed by the departments were:
- Acceptance of the image-distribution system by orthopedics (operational improvements were a secondary consideration compared with image quality).
- Image throughput: a patient was able to return to the orthopedic department from radiology in 25 minutes; therefore, images would need to be waiting when the patient got back.
- A total change in the way study images were to be viewed.
Tool time
The task force set about quantifying the changes it needed to make. The group used flow charting, failure-point and data-point analysis, service metrics, queuing theory, and after-action reporting as its tool set.
Of the available tools, service metrics was perhaps the most critical for the radiology department. For an organization or system to improve performance it must first measure itself among the dimensions that customers value. In this case, radiology had two customers:
- The patient and his/her experience (throughput).
- The orthopedic surgeons and their ability to care for their patients (image quality and throughput).
After-action reporting, another key to successful culture change and performance improvement, can be rough at times, especially if the report is brutally honest about performance shortfalls. However, objective and candid feedback is extremely effective when ground rules are established, all levels of staff are included, and developing and maintaining the system’s success are discussed.
Move ‘em out
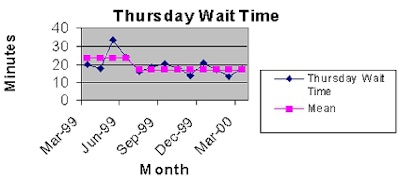
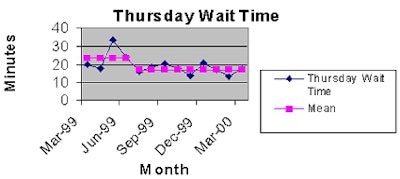
Reducing patient throughput time was identified as the task force's most critical goal. Working together, the radiology and orthopedic departments were able to reduce patient throughput time by 34% over the course of one year. Their success has been sustained to this day.
In the attached graph, the group chose Thursday patient times because Thursdays are a typically busy day in orthopedics. Consequently, volume of traffic is consistently high in radiology.
 |
The evolution of patient throughput continues to evolve and grow in sophistication. With digital imaging, image throughput becomes part of the patient throughput value. Thus, any image or data bottlenecks in the PACS/RIS will be reflected throughout the institution’s systems.
From its inception, the task force recognized the need to develop sustainable solutions. After experiencing the frustrations of prior initiatives whose results were short-lived, the departments placed a high value on sustainment. To this end, the group did not claim victory after reducing the patient throughput time, but rather used the success as momentum for continuing improvement.
The transformation of radiology and orthopedics from two independent constituencies to a team focused on improving patient care was a win in itself. And while challenges still exist, the departments now have an objective, systems-focused forum to address any issues that may arise.
By Ronald Doncaster
AuntMinnie.com contributing writer
June 13, 2001
Related Reading
PACS quality control ensures that exams get read, May 30. 2001
Secure patient satisfaction through superior service, May 17, 2001
What's up D.O.C? Non-PACS innovations in radiology, April 30, 2001
Copyright © 2001 AuntMinnie.com
Click here to post your comments about this story. Please include the headline of the article in your message.