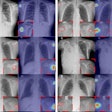
There is large amount of interreader variability in the detection of lung nodules on chest x-rays. For many cases, lung cancer has been reported as visible in retrospect. CAD helps, of course, but Bram van Ginneken, PhD, a professor at Radboud University Nijmegen Medical Centre, and colleagues sought to explore the potential gain by combining multiple, independent observers. Thus, they aimed to define the "visual" detectability that CAD should ideally achieve.
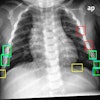
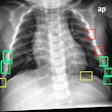
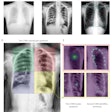
For their study, the researchers included 111 digital chest x-rays that contained a single small nodule with an average diameter of 16 mm, as well as 189 normal controls. Nodules had to be visible on the frontal radiograph, with 42% of them judged as being of low and very low conspicuity.
Twelve observers were asked to localize the lung nodules in the chest x-rays with the help of bone-suppressed images. Mean sensitivity in a false-positive fraction range between 0 and 0.2 was used to measure nodule localization performance.
Mean sensitivity was 64% for a single reading (range, 45.5% to 78.2%). When the readings of two observers were combined, mean sensitivity improved to 73.1%. Adding more observers led to an even better performance: Mean sensitivity for 12 observers was 82.3%. On average, 26 nodules were missed by single observers, 15 nodules were missed by a combination of two observers, and five were missed by a combination of 12 observers.
The variable and partially low baseline performance shows the limitation of single observers. If CAD can attain the performance level of multiple readers, a dramatic improvement in nodule localization can be expected with a drastic reduction of missed rates, the researchers concluded.