VIENNA - Incidence and management of tuberculosis (TB) in Russia are much mystified and misunderstood, according to Dr. Igor Tyurin, the chief radiologist at Russia's Medical Academy for Postgraduate Education.
Despite a constant yearly decrease in the number of new cases, the high number of patients infected with the disease means that the country's screening strategy and follow-up, a legacy from the Communist era, must be radically updated to enable its radiological services to manage these patients effectively. New modalities have already started to modify radiology's diagnostic approach to the disease, and this must be built on to ensure continued improvement in this area, Tyurin told delegates on Friday.
As part of the "ESR meets Russia" session that highlighted Russian contributions to, and accomplishments in, imaging, attention was drawn to current TB imaging, one of the former Soviet Union's imaging success stories in the '60s and '70s.
TB is a potentially curable disease, but it presents no initial specific clinical symptoms, is contagious, progressive, and can be fatal without treatment. Its association with poverty, poor nutrition, alcoholism, and economic instability has meant that Russia, with 80 cases per 100,000 inhabitants and a mortality rate of 15 per 10,000, has one of the heaviest incidence rates after South Africa, North Korea, and South East Asia.
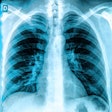
Russia's 5,000 plus x-ray machines serve as a wide network of TB screening devices that outweigh the low diagnostic sensitivity of bacteriology, which ranges from 25% to 65%. Therefore, while x-ray is not recommended for TB screening in most developed countries, it is a well-established system of TB control in the big country, according to Tyurin.
Furthermore, in the past 10 years digital radiography has replaced around 80% of traditional fluorography screening procedures, yielding decreased radiation exposure, increased sensitivity, and improved workflow. More than 60% of adults are involved now in screening programs and 60% of all new cases in Russia are detected at screening.
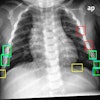
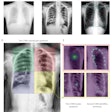
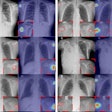
X-ray screening, however, presents its own challenges: There is no radiographic pattern unique or specific to TB, and this is compounded by atypical patterns seen in TB patients with HIV. Moreover, chest x-ray is insufficient as a single tool in the diagnosis and follow-up of the disease.
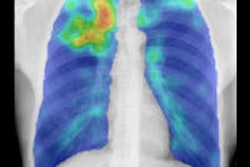
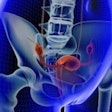
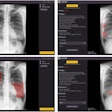
The introduction of CT, MRI, and PET/CT, as well as whole-body imaging for HIV-associated TB, now promises much for honing detection, assessment, and follow-up, particularly for differential diagnoses, staging, and disease activity. Multislice CT could aid in the assessment of multifocal and multisystem TB. It could also reduce the overdiagnosis of TB, or "false positives" by identifying nontuberculous changes such as calcification and thymus and vascular abnormalities, as Tyurin demonstrated in his presentation through a ductus arteriosus calcification visualized both on CT and x-ray.
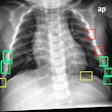
Furthermore, lymphadenopathy, often the only radiographic finding in the pediatric patient and, therefore, a hallmark of TB, might be difficult to assess with x-ray if the primary TB changes were only slight. CT therefore was an important tool in risk group pediatric patients as it improves the diagnosis of lymphadenopathy.
However, lymph node assessment with CT in the pediatric TB patient remained problematic, often leading to overdiagnosis of TB due to errors in interpretation and a lack of measurement standards, as well as a lack of standardization in contrast enhancement dose in high-risk patients.
"The challenge is now to accompany this new technology by a change in organization and education. New equipment needs new specialists. CT, MRI, and PET must be routine practice in TB treatment," Tyurin noted. "Clinical guidelines are needed for the routine use of CT in pediatric patients with suspected TB. We also need to make changes to the frequency of screening and target the high-risk population rather than conduct whole-population screening."
Originally published in ECR Today on 8 March 2014.
Copyright © 2014 European Society of Radiology