VIENNA - Exposure indexes, image quality, and patient dose were at the heart of the scientific session for radiographers on Thursday at ECR 2014.
Good radiographic technique should result in a low patient dose and high-quality images, but that's not always the case, as there is generally a trend toward increased dose through a greater frequency of examinations and high-dose examinations.
Decision-making and variation exposure factor selection also vary significantly from radiographer to radiographer, according to a study by the University College Dublin (UCD) School of Medicine and Medical Science in Belfield, Dublin, Republic of Ireland. "There is inconsistency in the exposure factor selection by radiographers, and we should be worried," said Sarah Darcy, who presented the results of the study in front of a packed audience.
 Sarah Darcy from Dublin, Republic of Ireland.
Sarah Darcy from Dublin, Republic of Ireland.She and her colleagues at UCD used the Tobii TX300 system, an eye tracker using pupil-center corneal reflection technology (PCCP). Eye tracking uses an infrared light to print the reflection, which is then captured by a camera. The images obtained are then turned into data. "What we were interested in was fixations, fixation duration, and the time it takes to first fixation. We wanted to determine whether variations do exist between radiographers in the area of exposure factor selection and, if so, how does this relate to the way they visually assess patients before examination," she said.
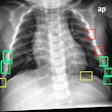
They asked radiographers of different ages and experience from an Irish teaching hospital to sit down at the eye tracker, look at the images, and explain which examination factors they were going to use for this or that examination. Darcy and her colleagues used 40 virtual patient models and four commonly performed radiographic examinations: anteroposterior (AP) shoulder, portable chest, AP lumbar, and lateral lumbar). They also recorded exposure factors for patient models while eye-tracked.
What Darcy and her colleagues found out was unexpected: a significant correlation between lower radiant milliampere-seconds (mAs) values and age and experience, and an even stronger correlation with the number of years of digital-only practice.
"Older and more experienced radiographers gave lower mAs doses for the lumbar examinations. The higher mAs doses were used for AP shoulder. The longer the time to first fixation on relevant anatomical areas for the AP portable chest examination, the higher the patient kVp/mAs dose was," she said.
In this environment, standardization and equalization of dose is even more important and must be achieved, she argued. "To achieve this, we believe that we need to understand the decision-making of the radiographer. Further investigation is necessary and should be expanded to other centers, and we should pursue optimal patient care."
 Nejc Mekiš from Ljubljana, Slovenia.
Nejc Mekiš from Ljubljana, Slovenia.In another talk, Nejc Mekiš, from the medical imaging and radiotherapy department at the Faculty of Health Sciences at the University of Ljubljana in Slovenia, discussed the impact of additional copper filtration upon radiation dose received and image quality during adult chest examinations. Copper filtration is used, especially in pediatric applications, to reduce radiation dose to patient.
Mekiš took part in a study by the University of Ljubljana, the UCD School of Medicine and Medical Science in Dublin, and the College of Health and Technology at the Polytechnic Institute of Coimbra in Portugal.
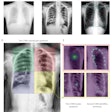
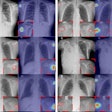
They looked at the impact of additional copper filtration within the primary x-ray beam, and used anthropomorphic phantom imaging to do so. They used routine chest examination protocols across Slovenian clinical sites and experimental protocols in two representative clinical centers. They then analyzed the resultant radiation dose and image quality findings.
"We found out there is a wide range of protocols in use clinically for the most common diagnostic examination (chest x-ray). Even in the PA position, radiosensitive organs recorded significant dose reductions, between 20% and 57%. There is also potential for greater superficial organ dose savings in this position," he said. "The sharing of experiences between the three academic centers created the potential to investigate practice and optimize protocols to achieve dose reductions."
Originally published in ECR Today on 7 March 2014.
Copyright © 2014 European Society of Radiology