CHICAGO - The utilization rates of noninvasive imaging in patients with suspected coronary artery disease show a precipitous decline, with coronary CT angiography greatly underused, according to a study presented on Wednesday at RSNA 2015.
The brunt of the decrease is in nuclear myocardial perfusion imaging, which experienced a double-digit decline from its peak in 2006 to 2013. Stress echocardiography was also down by more than 10% between 2010 and 2013.
 Dr. David C. Levin from Thomas Jefferson University.
Dr. David C. Levin from Thomas Jefferson University."In the recent years, there has been considerable downward pressure on the use of cardiac imaging," said lead author Dr. David C. Levin from Thomas Jefferson University. "This has come from things such as appropriate use criteria developed by both the American College of Radiology and the American College of Cardiology; the Choosing Wisely campaign; reductions in reimbursement, mostly with the technical components; and high deductible health plans as well."
To quantify utilization trends, Levin and colleagues analyzed the nationwide Medicare Part B databases from 2001 through 2013, using CPT codes for primary nuclear myocardial perfusion imaging (MPI), stress echocardiography, and coronary CT angiography (CTA).
"We looked only at the primary codes [and] not the add-on codes, which apply to MPI and stress echo. When those codes are bundled, that did not affect the data," Levin told RSNA attendees.
They calculated procedure volumes for all facilities that provide imaging services, along with utilization rates per 1,000 Medicare fee-for-service beneficiaries. Medicare specialty codes were also used to determine the participation of radiologists and cardiologists in performing the scans.
Crunching the numbers
In the realm of nuclear myocardial perfusion imaging, the utilization rate per 1,000 increased from 63.4 in 2001 to a peak of 88.0 in 2006. The numbers then declined to 61.9 per 1,000 in 2013, representing a drop-off of 30% from the modality's height in 2006.
In 2013, cardiologists performed 77% of the nuclear MPI studies, while radiologists handled 17% of the scans and other physicians were involved with the remaining 6%.
"Radiologists never really saw much in the way of growth in MPI in the earlier years," Levin said. "Then in the more recent years -- from 2006 to 2013 -- there has been a more gradual downward drift."
For stress echocardiography, the utilization rate was 12.5 per 1,000 in 2001. That rate remained relatively stable for the next nine years until 2010, when the number peaked. The utilization rate then declined to 10.8 per 1,000 by 2013, representing a decrease of 14% from 2010 to 2013.
Cardiologists' numbers mirrored the total utilization rate for stress echocardiography, as radiologists essentially play no role in administering these studies.
For coronary CT angiography, the results were particularly noteworthy. The researchers analyzed coronary CTA beginning in 2006, when CPT codes for the imaging scan were established.
Initially, there was a steep increase in utilization, advancing from a rate of 1.0 per 1,000 in 2006 to 2.1 per 1,000 in 2007, primarily because coronary CTA was a relatively new technique.
The novelty wore off rapidly, however, with a sharp decrease in 2008 followed by a steady decline to 1.1 per 1,000 in 2013, representing a fall of 49% from its peak in 2007.
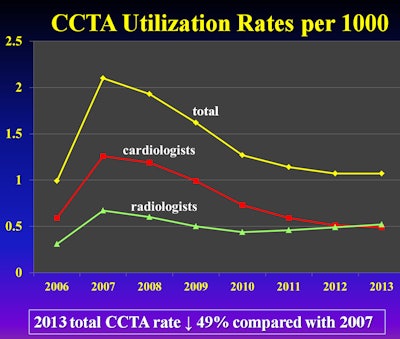 Image courtesy of Dr. David C. Levin.
Image courtesy of Dr. David C. Levin.Back in 2007, cardiologists performed almost twice as many coronary CT angiographies as radiologists. By 2013, radiologists conducted slightly more coronary CTA procedures, accounting for 49% of the total, compared with cardiologists, who handled 46%.
There has been "a fair amount of controversy" over whether coronary CTA is better than nuclear MPI for suspected coronary artery disease, Levin said in his presentation.
"My own personal opinion is that for patients with suspected early coronary artery disease, CTA is a better test," he said.
Typically, patients will present to a doctor or emergency room with some sort of chest pain. Under those circumstances, CTA can be used to rule out a host of more serious causes of chest pain.
"Not just coronary disease, but also pulmonary embolism, aortic dissection, pneumothorax, lung tumor, mediastinal tumor, a rib lesion, or other malady," Levin told AuntMinnie.com. "And if that CT scan is negative, you can rest assured that the patient has no real serious cause of chest pain."
In support of CTA's value, he cited a 2015 study in Circulation: Cardiovascular Imaging, which concluded that the technique is "more accurate than SPECT-MPI" for the diagnosis of coronary artery disease "as defined by conventional angiography and may be underused for this purpose in symptomatic patients."
Underutilized CTA
"To say that coronary CTA is underused is quite an understatement," Levin added. His study found that in 2013, there were 56 times as many nuclear MPI scans than coronary CTAs.
"That is almost unbelievable," he said to AuntMinnie.com. "If you were to ask: What should the ratio of myocardial perfusion imaging to coronary CTA be, in terms of which test is the better test? Maybe the ratio should be 1-to-1 or maybe twice as many myocardial perfusion imagings done as coronary CT angiography, but not 56 times."
Levin said there are several reasons for coronary CTA's lack of growth, including the high cost of equipment, the specialized software required, its labor-intensive nature, poor reimbursement and frequent insurance denials, and a fair amount of self-referral for MPI among cardiologists.
In addition, cardiologists may not feel comfortable reading the noncardiology portions of the scan, he noted.
As for the future, Levin speculated that coronary CTA utilization will increase, given the recent number of published papers that validate its efficacy in comparison with myocardial perfusion imaging.
"I think the use of coronary CTA will increase and it will be mostly among radiologists," Levin said. "We in radiology should be promoting the use of coronary CTA, and we should be pointing out to referring physicians -- not just cardiologists, but primary care doctors -- that coronary CTA is the best first imaging test for coronary artery disease."