TORONTO - A breath test that analyzes chemical compounds could distinguish between malignant and benign tumors in the lung, according to data presented at the American Association for Thoracic Surgery (AATS) meeting. Early research indicates the test has better specificity than PET.
But don't go throwing out your imaging scanners in favor of Breathalyzers: the technique requires additional study and is some ways away from clinical use, according to Dr. Michael Bousamra, an associate professor in the thoracic and cardiovascular surgery division at the University of Louisville. Bousamra is also head of thoracic surgery at the James Graham Brown Cancer Center in Louisville, KY.
Still, it offers a tantalizingly simple solution to the problem of detecting cancer in an asymptomatic population.
"The idea of analyzing exhaled breath is not new," Bousamra said. "It would be extremely easy for patients to participate [in a breath test as a form of diagnosis of lung cancer]."
Previous research
Over the past few years, clinicians have noted significantly higher concentrations of carbonyl compounds in the breath of lung cancer patients, which prompted this investigation, Bousamra explained. Previously published research identified four carbonyl compounds that were elevated in patients with lung cancer compared to healthy controls (Fu et al, Cancer Medicine, February 2014, Vol. 3:1, pp. 174-181). In addition, a 2007 study in Cancer Biomarkers found that a two-minute breath test was comparable to CT chest screening in terms of accuracy for lung cancer detection (Phillips et al, Vol. 3:2, pp. 95-109).
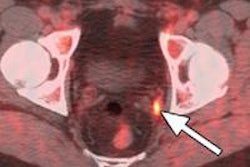
In the current study, the researchers sought to compare breath analysis and PET for diagnosing malignancy. They used aminooxy-coated silicon microchips to selectively capture exhaled carbonyls; breath samples were flowed through the silicon chips by applied vacuum. Bousamra and colleagues used mass spectrometry to analyze the carbonyl adducts. They utilized four carbonyls that have significantly greater concentrations in lung cancer as markers of disease.
The researchers studied 88 healthy control subjects, of whom 45 were current smokers and 43 were nonsmokers; 107 patients with early-stage lung cancer, mainly non-small cell lung cancer; and 40 patients with benign pulmonary disease, of whom 12 were current smokers. Seven patients had a solitary pulmonary metastasis. Those patients had primary tumor sites including the colon, skin, prostate, and breast.
The researchers also noted the age of participants: They found that healthy control subjects and patients with benign lung disease were younger than patients with lung cancer. The average age of healthy controls was 42.2 years, the average age of patients with benign disease was 50.9, and the average age of patients with lung cancer was 65.8.
When having more than two elevated markers was defined as an indicator of early-stage lung cancer, the breath test showed 83% sensitivity and 75% sensitivity. PET imaging in the same group of patients produced 90% sensitivity but only 39% specificity.
"The sensitivity is similar to PET but the specificity is greater," Bousamra said.
Not ready for prime time?
Bousamra stressed that breath analysis is not yet ready for prime time. The data need to be reproduced in a larger study that, in particular, will have a much larger number of patients with benign pulmonary disease, he said.
"That is a weak spot of the dataset, that we only had 40 patients with benign pulmonary disease," Bousamra said.
Also, the use of the markers was not definitive. A total of 24% of lung cancers classified as stage 0/I had fewer than two elevated cancer markers. One stage III patient had one elevated cancer marker, and one stage II patient had no elevated cancer markers.
The group observed normalization of three of the four markers subsequent to resection within one month, suggesting that breath analysis could be used in the future to monitor patients for tumor recurrence. "This could represent a means of following patients postoperatively," Bousamra said.
A less-invasive method of diagnosis such as breath analysis does not pose the same risks as other methods of diagnosis, Bousamra noted.
"An error in diagnosis is potential harm [with a breath test], but there is no risk of pneumothorax as you would have with a [percutaneous lung] biopsy," he said in an interview with AuntMinnie.com.
In addition, a breath test is significantly less expensive than PET imaging, for example, as a diagnostic tool.
Bousamra and colleagues plan to compare breath analysis and screening CT prospectively in a future investigation.