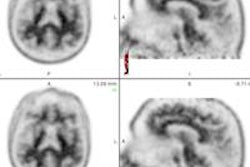
In a large study of patients with known or suspected cardiac sarcoidosis, researchers found that FDG-PET could identify those at higher risk of death or life-threatening arrhythmia, according to results published in the February 4 issue of the Journal of the American College of Cardiology.
Patients with two key markers on FDG scans -- perfusion defects and abnormal FDG uptake -- were almost five times as likely to have an adverse event. Patients with cardiac sarcoidosis and a poor prognosis may benefit from an implantable cardiac defibrillator as well as anti-inflammatory therapies, the study authors wrote.
"We found that patients that have abnormalities in both myocardial perfusion and metabolism (reflecting active inflammation) had the highest event rate, particularly if there was also evidence of [right ventricular (RV)] involvement," wrote lead author Dr. Ron Blankstein and colleagues from Brigham and Women's Hospital (JACC, February 4, 2014, Vol. 63:4, pp. 329-336).
"Since all of these patients also had PET abnormalities involving the [left ventricle], it is conceivable that the presence of focal RV inflammation may be a marker for greater extent and/or severity of disease," they added.
Diagnostic challenges
Cardiac sarcoidosis is an inflammatory disease that can adversely affect heart function; increasingly, it has been cited as a cause of heart failure and arrhythmias. It can be difficult to detect with imaging due to the focal nature of the disease, according to the authors. Endomyocardial biopsy has limited sensitivity, as it often misses areas of cardiac involvement.
"Therefore, the diagnosis of cardiac sarcoidosis is challenging and often relies on integrating both clinical and imaging findings," Blankstein and colleagues wrote.
The study included 125 consecutive patients with no coronary artery disease who were referred for a cardiac FDG-PET scan for known or suspected cardiac sarcoidosis between May 2006 and January 2011. Subjects underwent rest myocardial perfusion and metabolic imaging using rubidium-82 and FDG in a whole-body PET/CT scanner (Discovery RX LightSpeed 64, GE Healthcare).
Follow-up records were available for 121 of the 125 patients, with another four patients lost during follow-up, bringing the final cohort to 118. The mean age of the participants was 52 years (± 11 years), with 67 men and 51 women.
During the median follow-up of 1.5 years, 31 patients (26%) died or experienced ventricular tachycardia, a potentially serious heart-rate irregularity that begins in the ventricles. Of the 27 (23%) ventricular tachycardia events, 25 required device-related treatment and two people were admitted to the emergency room. Among the eight (7%) patients who died, four also had ventricular tachycardia.
Two key signs
The PET images were interpreted independently by two experienced cardiologists. Normal metabolism was defined as either complete suppression of FDG from the myocardium or diffuse FDG uptake with no areas of focal uptake. The presence or absence of focal RV FDG uptake also was recorded.
Among the 118 subjects, 47 (40%) had normal cardiac PET results; 37 (31%) had myocardial perfusion defects or focal FDG uptake, and 34 (29%) had both abnormal myocardial perfusion and FDG uptake.
It was this latter group that demonstrated the prognostic value of cardiac PET. The presence of both a perfusion defect and abnormal FDG uptake had a hazard ratio of 3.9 as a predictor of death or ventricular tachycardia. The association remained statistically significant after adjusting for left ventricular ejection fraction and clinical criteria.
Another key indicator of future adverse events was right ventricular uptake of FDG; these patients had a hazard ratio of 4.2 for future adverse events -- a nearly fivefold increase in risk. The authors postulated that right ventricular involvement could be a marker for greater disease severity.
That said, patients with normal myocardial perfusion and normal metabolism were not immune to adverse cardiac events. They had an annual adverse cardiac event rate of 7.3%, although that rate was dwarfed by the 31.9% for patients with abnormal perfusion and inflammation.
Advantages over cardiac MR
The study demonstrated that PET has advantages over another up-and-coming modality for cardiac imaging, cardiac MRI, Blankstein and colleagues noted.
"Our study suggests that inflammation-targeted cardiac PET imaging has a potentially important role in evaluating patients with known or suspected cardiac sarcoidosis," they concluded. "In comparison to [cardiac MRI], PET has the advantage of being able to image patients with implanted pacemakers or defibrillators and those with impaired renal function."
The authors speculated that PET might also "identify FDG-avid disease outside the heart, which may be more accessible to biopsy than the myocardium."