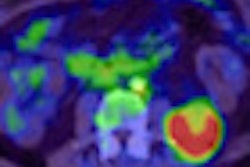
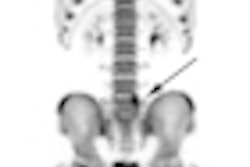
According to the Society of Nuclear Medicine (SNM), more than 16 million Americans undergo nuclear medicine procedures each year for medical conditions including cancer, cardiovascular disease, neurological disease, and other physiological problems.
To increase awareness of nuclear medicine and molecular imaging's benefits, the organization is reaching out to patients, physicians, payors, and other decision-makers in a variety of ways.
 |
| Dr. George Segall. |
AuntMinnie: Since assuming the role of SNM president, what have been your target priorities?
Segall: There are four major goals that we would like to accomplish in a timely manner. One goal concerns radiation safety. SNM was one of the leading organizations, along with the Society for Pediatric Radiology, the American Association of Physicists in Medicine, and the American College of Radiology, in the Image Gently campaign to reduce radiation exposure in children.
As a result of these efforts, there were two important publications that appeared in the Journal of Nuclear Medicine this year. One paper was the 2010 North American guidelines on pediatric radiopharmaceutical doses, published in February, which makes recommendations on dosage of radiopharmaceuticals for a number of procedures used in children and indicates strategies to reduce dose to as little as possible. The second notable paper, published in August, specifically addresses how to reduce radiation in children and how to communicate the small risk associated with radiation to concerned parents.
There will also be a poster developed to raise awareness of these new guidelines for pediatric procedures in the December issue of the Journal of Nuclear Medicine Technology.
SNM is also taking the lead in the Image Wisely campaign, which will deal with radiation exposure from nuclear medicine procedures in adults. It will follow a similar trajectory to the work done for the Image Gently campaign.
How different is the message for the adult population compared to pediatric patients?
The basic principle called ALARA -- as low as reasonably achievable -- is equally applicable in adults as it is in children. The specifics of the various procedures are different. Children are not just scaled-down adults. There are special considerations with children, but the principle that we should use as low a dose as possible will be the same.
First and foremost, is the study indicated the appropriate one to answer the question? We need to heighten awareness about that. The indications for many procedures are clear-cut but difficult to apply to individuals with complex medical problems.
Because technology has improved and our machines are more accurate and faster, we can use lower doses of radiation to get the same image quality in the same amount of time. There are new radiopharmaceuticals that are more specific for the medical conditions, and as a result, the agent is specially designed to answer questions in a most accurate and efficient way. By having a wider choice of agents, it is possible to select the most appropriate agent for patients and utilize the smallest dose possible.
How do you educate more patients about the benefits of nuclear medicine and molecular imaging?
That is our second goal. SNM has embarked on an outreach campaign to inform patients about the field of molecular imaging and, specifically, the diagnostic tools that are now available.
We formed a patient advocacy advisory board with representatives from several large patient groups, including the Alzheimer's Association, the American Thyroid Association, the Leukemia & Lymphoma Society, the Ovarian Cancer National Alliance, and the Coleman Foundation. As a result, we developed a new website that will be officially launched later this month: discoverMI.org. It will be a gateway with resources for patients to educate themselves about molecular imaging diagnostics and therapy, and they can discuss with their doctors whether these agents are appropriate in their particular circumstances.
What is the most difficult part about educating patients about molecular imaging?
Technology advances so quickly and there are new developments all the time, so it can be hard to keep pace. It is important to present information concisely, accurately, and efficiently to people, and that is the goal of this website.
The field of medicine in general and medical technology have exploded so rapidly that it is very difficult for even healthcare professionals to fully appreciate the value of all the medical tools available to them. Patients are at a greater disadvantage because they do not always understand the terminology. I think this website will go a long way to helping patients educate themselves, and they will not have to Google "molecular imaging" or "nuclear medicine" and find 16,000 links.
Another priority has been to increase comparative effectiveness research. How is it progressing?
Comparative effectiveness research has been happening in a number of healthcare fields, but it has not happened in a consistent, organized fashion in nuclear medicine and molecular imaging. SNM has engaged the Center for Medical Technology Policy to help us organize a symposium that will bring together a broad cross-section of professionals specifically to develop comparative effectiveness research study blueprints on the use of FDG-PET/CT in oncology.
Our first workshop will be held next spring to focus on comparative effectiveness studies of FDG-PET/CT in head and neck cancer. We will bring together imaging physicians, head and neck surgeons, medical oncologists, patient advocates, and representatives from the U.S. Centers for Medicare and Medicaid Services, private payors, and industry to identify the methodologies we need to answer specific questions. That way, we can generate the medical evidence and appropriateness criteria to make sure that FDG-PET/CT is used appropriately for patients with head and neck cancers.
And the fourth priority is?
That would be our Clinical Trials Network (CTN) to facilitate the use of molecular imaging biomarkers in clinical trials and new therapeutic drugs. There is an unfulfilled need to ensure that quality imaging is conducted in clinical trials of drug development. If the data were not reproducible, then the validity of the whole trial regarding the therapeutic drug was open to question.
To date, we have validated more than 110 PET/CT scanners across the U.S., the U.K., Canada, Europe, Australia, and Asia. Clinics and hospitals voluntarily underwent and passed a rigorous evaluation program and have been designated as CTN-validated sites. When pharmaceutical companies wish to use biomarkers in their drug development trials, they can go to these sites confident that the quality of the data will be very high.
SNM also obtained an investigational new drug (IND) application for the radioactive tracer molecule fluoro-L-thymidine. This is a nonproprietary agent that seems to be very useful in monitoring early response to chemotherapy in a number of cancers. As such, it is of interest to pharmaceutical companies that are designing new drugs to be more effective in fighting cancer. As a result of this IND, there are two multicenter, industry-supported studies under way right now.
Given the increasing role that hybrid imaging plays in radiology, what initiatives are under way to educate aspiring technicians in this area?
SNM and the American College of Radiology have a joint task force on nuclear medicine training, and we identified educational goals and training pathways in a report that was published in June.
SNM has also developed a Web-based molecular imaging basics curriculum for radiologists and nuclear medicine residents. This is a series of 12 webinars, one per month, for Molecular Imaging 101. It is intended specifically for radiology residents and nuclear medicine residents to fill gaps in the educational programs at the training centers across the country, which focus on clinical aspects of molecular imaging, such as hybrid imaging, and don't have the time or the expertise to teach the basic principles of new molecular imaging agents that are CT, MRI, ultrasound, optical, and radioisotope based.
Speaking of hybrid imaging, how would you evaluate the efficacy and future role of PET/MRI?
I think it is most intriguing from a number of perspectives. It is the hybrid imaging technology that presents the most technical challenges. Technically speaking, it makes PET/CT look relatively simple, and many people are excited about the actual technology.
Many people, including myself, are very excited about the potential clinical applications because the capabilities of MRI are substantially different from CT. We see potential applications in head and neck cancer, breast cancer, and tumors that have metastasized to the liver and the skeleton, as well as in primary tumors of the pelvis, such as gynecological malignancies. These are all areas where MRI either outperforms CT or adds additional information to CT.
How soon do you see PET/MRI making a significant contribution in the clinical setting?
The challenge will be to do the studies and obtain medical evidence needed in this era of healthcare reform to prove value. I think that will take some time. The technology is ready for prime time. Prime time is now, but we are not quite sure how we will use it appropriately right now, and I think it will take a couple of years.