With the help of real-time images from a portable gamma camera, Dutch physicians intraoperatively identified 20% more laparoscopic sentinel nodes in testicular cancer patients imaged by SPECT/CT, according to a study in the April issue of the Journal of Nuclear Medicine.
The sentinel node procedure, with the addition of real-time gamma camera images, "may enable better selection of patients who would benefit from adjuvant treatment after orchiectomy, avoiding costly surveillance and decreasing the risk of finding lymph node metastases at a later stage," the researchers wrote.
The lead author of the study is Dr. Oscar Brouwer, from the department of nuclear medicine and surgery at the Netherlands Cancer Institute in Amsterdam (JNM, April 2011, Vol. 52:4, pp. 551-554).
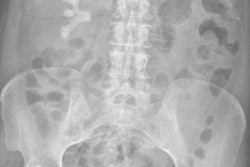
The study enrolled 10 patients with a mean age of 37 years, ranging from 25 to 50 years old. All 10 patients had clinical stage I testicular cancer and were referred to the institute between November 2006 and November 2010. Primary tumors were located on the right side in five patients and on the left side in the other five patients.
Imaging protocol
Patients received an average dose of 80 MBq of a technetium-99m (Tc-99m) nanocolloid radiopharmaceutical before a dual-head gamma camera was used to obtain anterior and lateral dynamic images to visualize lymphatic flow and identify early-draining lymph nodes. The authors noted that Tc-99m nanocolloid under local anesthesia was well-tolerated by all 10 patients, with no adverse side effects observed.
In the same imaging session, SPECT/CT was performed using a hybrid camera (Symbia T, Siemens Healthcare), followed by correction for attenuation and scatter.
Two hours after tracer injection, delayed planar images were obtained to differentiate first-echelon nodes from higher-echelon nodes and identify unexpected drainage patterns. The researchers considered the first node in each nodal basin on the early planar images as the sentinel node. Nodes appearing later in the same basin were deemed the higher-echelon nodes.
All patients then underwent sentinel node excision and orchiectomy within six hours after injection of the tracer. Surgeons viewed the patients' SPECT/CT images in the operation room to guide the laparoscopic detection witha laparoscopic gamma ray probe (Europrobe, Euro Medical Instruments).In addition, sentinel nodes were intraoperatively identified using the portable gamma camera (Sentinella, OncoVision) in nine patients. (The portable gamma camera was not yet available for one patient.)
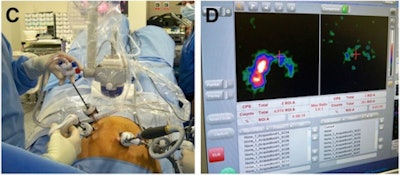 |
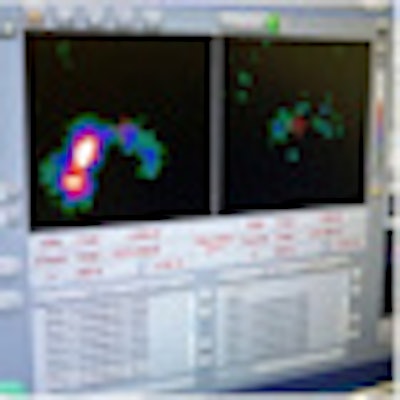
| (C) The laparoscopic sentinel node procedure uses a portable gamma camera and laparoscopic gamma ray detection probe. (D) The pre-excision image (left screen) acquired with the portable gamma camera shows both sentinel nodes. After excision (right screen), no significant remaining activity is seen. All images courtesy of the Journal of Nuclear Medicine. |
Localization of the sentinel node by the portable gamma camera was aided through the use of an iodine-125 brachytherapy seed placed on the tip of the laparoscopic probe, which aided physicians in seeing the location of the probe relative to the sentinel node.
Image analysis
A review of the images found that lymphoscintigraphy in combination with SPECT/CT showed lymphatic drainage in all 10 patients (100%), and a total of 21 sentinel nodes were preoperatively identified. SPECT/CT also accurately located the sentinel nodes and provided anatomic reference points to plan the laparoscopy in all patients.
Surgeons localized and removed all preoperatively identified sentinel nodes, but left the higher-echelon nodes in place. The portable gamma camera then enabled real-time sentinel node visualization in all nine patients for whom the device was used.
Brouwer and colleagues noted that intraoperative images after excision of sentinel nodes showed unexpected significant residual radioactivity at the same location in three of the nine patients, "resulting in identification and removal of five additional sentinel nodes (20%). In total, 26 sentinel nodes were laparoscopically removed."
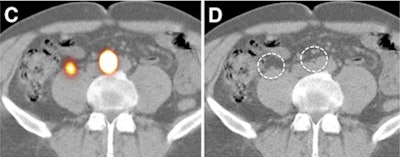 |
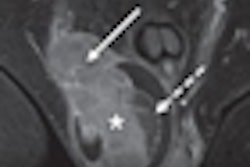
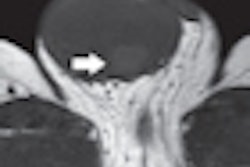
| Transverse SPECT/CT image (C) shows two sentinel nodes displayed in yellow. CT image (D) shows medial sentinel node corresponding to small lymph node ventral to area between aorta and cava, whereas lateral node is in area ventral to psoas muscle (circles). |
The researchers concluded that SPECT/CT enables anatomic localization of retroperitoneal sentinel nodes in patients with testicular cancer. Real-time image guidance using a portable gamma camera with a laparoscopic gamma ray detection probe "improves intraoperative sentinel node detection and appears to identify 20% additional sentinel nodes," they wrote.
While the procedure may help determine which patients might benefit from adjuvant treatment after orchiectomy, further study is needed to verify the clinical value of the sentinel node procedure in testicular cancer, according to the authors.