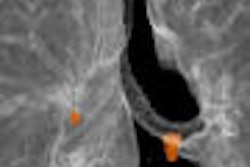
The use of PET/CT can decrease uncertainty and improve diagnostic accuracy in 18-F FDG-PET studies to detect unexpected malignancies. By precisely localizing the area of focal 18-F FDG uptake, PET/CT can increase accuracy and reduce the probability of false-negative cases, as well as unnecessary biopsies caused by false-positive cases.
PET/CT can decrease the number of instances in which physiologic 18-F FDG uptake is interpreted as abnormal, according to two recent studies on the detection and clinical significance of unexpected 18-F FDG uptake. In addition, PET/CT can guide further investigations, such as biopsy or surgery, into areas of increased 18-F FDG uptake.
"In the interpretation of 18-F FDG-PET images, correlation with anatomic imaging is important not only because it can clarify the precise location of an 18-F FDG avid focus but also because it can reduce the probability of a false-positive or false-negative result," according to a research group from the Johns Hopkins Medical Institutions in Baltimore (Journal of Nuclear Medicine, May 2005, Vol. 46:5, pp. 752-757).
In the second study, researchers from the Rambam Medical Center and the B. Rappaport School of Medicine, both in Haifa, Israel, looked at the clinical significance of PET/CT detection of unexpected foci. "PET/CT can play an important role in guiding further investigations, including a biopsy or surgery, leading to a decrease in tissue-sampling errors and enhancing early, improved diagnosis and treatment," the group wrote (JNM, May 2005, Vol. 46:5, pp. 758-762).
Role of PET/CT in detecting new primary malignancies
Whole-body 18-F FDG-PET/CT is useful in detecting new, unexpected 18-F FDG avid primary malignant tumors, according to researchers from the division of nuclear medicine at the Russell H. Morgan department of radiology and radiological science at Johns Hopkins.
The research group retrospectively evaluated 1,912 patients with known or suspected primary tumors and found whole-body PET/CT (Discovery LS, GE Healthcare, Chalfont St. Giles, U.K.) detected unexpected 18-F FDG avid primary malignant tumors in 22 patients (1.2%) with cancer. These were new lesions not detected earlier by other modalities and that were atypical in location for metastases.
In all, PET-positive lesions suggestive of new primary malignant tumors were found in 79 patients (4.1%). But in 39 patients, no decision could be made whether the lesions were false-positive or false-negative results because of the lack of follow-up data. In 18 patients, the PET results were false-negative. The results were confirmed as true positives or false negatives based on pathological assessment, and clinical follow-up confirmed the results for eight of the false-negative patients.
Seven new malignant lesions were detected in the lungs, six in the thyroid, four in the colon, two each in the breast and esophagus, one in the bile duct, and one in the head and neck area (excluding thyroid). In one patient, two new lesions in the lung and thyroid were malignant. Among the false-positive sites that were pathologically confirmed, five were located in the thyroid, two in the uterus, two in the head and neck area (excluding thyroid), and one in the lungs.
"Detection of unanticipated malignant lesions has a significant clinical impact not only on healthy individuals but also on patients with known malignant disease," the researchers wrote. "In patients with known cancer, workups often focus on the patient's primary disease, and incidental coexistence of another primary malignant disease can be missed."
Seven of the 77 patients with either two or three primary malignant tumors before the PET/CT exam also had suspected new primary malignant tumors. Histology and immunochemistry showed 20 of the 22 patients had a different primary malignancy and not metastases from the known primary lesion. Even without follow-up data for 39 patients, the prevalence of additional primary tumors was almost the same as that of malignant tumors detected by 18-F FDG in asymptomatic individuals, according to the researchers.
The detection of new primary malignancies resulted in changed treatment plans for 17 patients. "Although false positives can occur, the true-positive prevalence is substantial," the authors noted. "Such newly identified lesions are often of early stage and thus have an excellent likelihood of being cured if treated promptly and aggressively."
Unexpected GIT foci on PET/CT clinically significant
Unexpected foci of 18-F FDG uptake that are localized by PET/CT to the gastrointestinal tract (GIT) are of clinical significance in most cases, and should be assessed further by tissue sampling using invasive procedures, according to the second JNM study.
"Most of these incidental foci represent unexpected GIT-related abnormalities, such as second primary tumors, sites of unusual metastatic spread, or premalignant lesions," the authors wrote.
The researchers retrospectively reviewed 4,390 patient files for cases that showed a single site of focally increased abdominal 18-F FDG uptake, localized to the GIT using PET/CT. And among the 58 cases that were found, they evaluated 34 cases for which follow-up data was available.
The results showed 71% (24/34) of the gastrointestinal foci had GIT-related pathology, and 59% (20/34) of the foci represented either malignant or premalignant lesions. Overall, in the group of 34 foci, there were 11 malignant lesions, nine premalignant lesions, four benign lesions, and 10 physiologic sites.
Four of the 34 patients were further assessed through clinical follow-up, while the other cases used surgery, colonoscopy, colonoscopy with biopsy, ultrasound-guided fine needle aspiration, or gastroscopy with biopsy.
"No additional diagnostic procedures were performed on four patients who had an uneventful clinical follow-up period of 12-31 months," the researchers wrote.
For patients with endoscopic findings that were negative and who had no evidence of disease during follow-up, the increased focal 18-F FDG update was attributed to physiologic activity and not due to any GIT-related pathology.
The maximal standardized uptake value (SUVmax) of 18-F FDG was measured for four categories -- malignant, premalignant, benign, and physiologic -- but there was no statistically significant difference in their intensities.
For malignant lesions, the SUVmax ranged from 8.1 to 40.3 (mean 17.3), for premalignant lesions from 4.5 to 40 (mean 14), for benign lesions from 8.7 to 35.6 (mean 18), and for physiologic sites from 5.7 to 30.8 (mean 11.1).
With regard to lesion location, three of the malignant lesions were located in the stomach, two in the small intestine, and six in the colon. One benign lesion was found in the stomach and three in the colon. All premalignant lesions and physiologic sites were in the colon.
In all, 28 foci of increased 18-F FDG uptake were found in the colon, of which 13 were in the ascending colon, six in the descending colon, seven in the sigmoid, and two in the rectum.
Whole-body PET images and unenhanced CT images for this study were also acquired using a Discovery LS PET/CT system. PET, CT, and fused whole-body images in axial, coronal, and sagittal planes were available for review.
The researchers noted that despite the increased confidence and decrease in the number of suggestive or equivocal lesions, the precise localization of increased 18-F FDG foci using PET/CT cannot yet solve the diagnostic dilemma of abnormal tracer uptake in the GIT.
However, PET/CT can play an important role in guiding further investigations, including biopsy or surgery, leading to reducing tissue-sampling errors and enhancing early, improved diagnosis and treatment, according to the researchers.
By N. Shivapriya
AuntMinnie.com contributing writer
June 30, 2005
Related Reading
PET benefits IWC for non-Hodgkin's lymphoma, June 10, 2005
FDG-PET/CT tops other technologies for lymphoma staging, March 23, 2005
PET/CT planning allows for greater gamble on NSCLC radiotherapy, March 16, 2005
PET/CT demonstrates staging strength over PET, CT, and PET plus CT, March 7, 2005
Copyright © 2005 AuntMinnie.com