Referring physicians who are attuned to FDG-PET's advantages are more likely to use the information for colorectal cancer treatment, according to the latest issue of the Journal of Nuclear Medicine.
Researchers from two institutions, the Ahmanson Biological Imaging Clinic at the University of California, Los Angeles and the Northern California PET Imaging Center (NCPIC) in Sacramento, CA, assessed the impact of 18fluorodeoxyglucose (FDG) PET imaging on the management of patients with colorectal cancer. Basing their results on a survey of referring physicians, the group suggested that more "with-it" doctors were satisfied enough with the modality’s results to change their protocol, as well as take the time to fill out the study survey.
Between October 1998 and January 2000, the researchers surveyed 95 physicians who had referred 146 patients for whole-body FDG-PET at UCLA and NCPIC. PET scans at both centers were performed on an Exact HR or HR+ system (CTI, Knoxville, TN), following injection of 555 Mbq of FDG. No attenuation correction was used at UCLA, and the images were reconstructed using standard filtered back projection. At NCPIC, attenuation was corrected and iterative image reconstruction algorithms were used. The resolution of reconstructed images was 8-12 mm.
In a single fax blitz, pre-PET and post-PET questionnaires were sent to referring physicians. Pre-evaluation questions included "How would you have managed the patient without knowledge of the PET findings?," while the post-evaluation form asked specifically what kind of management changes the PET exam had wrought (JNM, April 2001, Vol.42:4, pp.586-590).
The final response rate was 41%, or 60 doctors, with the highest number of returned surveys coming from medical oncologists (27%). The number one reason for ordering the FDG-PET exam was for more accurate staging (55%). The next most common reason was for monitoring the course of the disease (23%), the authors reported.
"The intended treatment before PET was surgery in 36.5%, medical treatment in 27%, radiation in 3%, and a combination of treatments in 5%," they said. Based on the FDG-PET results, changes in clinical stages were reported in 25 patients (42%). Of those, all but five were upstaged, while 32 had no change in clinical stage.
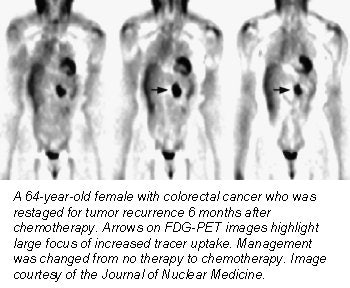 |
FDG-PET exams brought about intermodality treatment changes in 37% of the patients. More specifically, the referring physicians said they shifted from surgery to medical treatment in 11.7% of the cases. In 8% of the patients, surgery was chosen over the option of no treatment. Intramodality changes, including different surgical, medical, or radiation approaches, occurred in 18% of patients.
The group, led by Dr. Joubin Meta from UCLA, conceded that the study did have some limitations. Since more than 50% of the surveys were not returned, responder bias may be an issue.
"As a worst-case scenario, only supporters of PET might have responded, whereas those who believe that PET imaging was not useful for patient management might have refrained from participating in the study. In addition, less isolated and more ‘with-it’ doctors tend to respond more frequently," the authors said. But with a response rate of 44% solely from NCPIC, the probability of biased data was less likely, they wrote.
"This study shows that PET alters the clinical stage in 42% and changes the clinical management in >60% of the patients with colorectal cancer," the authors concluded. Given FDG-PET's high accuracy -- 95% for local disease -- the authors believe that including it in the diagnostic workup of patients with colorectal cancer is justifiable.
Information for this study was extracted from a larger prospective survey of referring physicians on FDG-PET’s role in the management of various cancers that was presented at the Society of Nuclear Medicine conference in June 2000. Co-author Dr. Marc Seltzer from UCLA told AuntMinnie.com that this type of information should help boost Medicare coverage of PET exams for other types of cancer.
In December 2000, the U.S. Health Care Financing Administration (HCFA) announced new or expanded Medicare coverage of PET imaging for six types of cancer, including lung and colorectal, but excluding ovarian and prostate cancers.
By Shalmali PalAuntMinnie.com staff writer
April 10, 2001
Related Reading
PET imaging is cost-effective in management of recurrent colorectal cancer, April 2, 2001
HCFA broadens Medicare coverage for PET, December 18, 2000
FDG-PET gains favor among referring doctors for cancer staging, treatment, June 7, 2000
Click here to post your comments about this story. Please include the headline of the article in your message.
Copyright © 2001 AuntMinnie.com