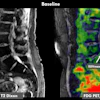
Low brain metabolic activity on FDG-PET/CT scans is associated with increased mortality in patients with advanced non-small cell lung cancer (NSCLC), according to research published April 9 in the Journal of Nuclear Medicine.
The finding is from a study that included 380 patients with NSCLC who underwent imaging before any treatment and suggests that brain glucose uptake independently predicts overall survival, noted lead author Julie Auriac, of Institut Curie in Orsay, France, and colleagues.
“Brain F-18 FDG uptake is a prognostic biomarker for survival in patients with advanced NSCLC and may help identify patients who would benefit most from prioritized supportive care interventions,” the group wrote.
F-18 FDG-PET/CT scans play a key role in the management of patients with NSCLC, with the scans focused on detecting tumors and their characteristics. Yet recent studies have suggested that metabolic activity in various organs and tissues measured from whole-body F-18 FDG-PET/CT images can also provide valuable information, the researchers explained.
To further investigate the potential role of brain function in patients, the researchers retrospectively collected clinical data and whole-brain FDG uptake measurements (mean standardized uptake values [SUVmean]) from 380 patients treated at Institut Curie between 2010 and 2023. They split the cohort chronologically into a discovery set of 234 patients (mean age, 64 years old) scanned through 2018 and a test set of 146 patients (mean age, 66 years old) scanned from 2019 onward.
 A visual abstract of the studyJournal of Nuclear Medicine
A visual abstract of the studyJournal of Nuclear Medicine
In the discovery set, a univariable analysis showed that high brain SUVmean (greater than or equal to the median) was associated with longer overall survival (OS) (hazard ratio [HR] 0.83; p < 0.001). Conversely, brain SUVmean was significantly lower in patients who died within one year compared with those who were still alive at the same time point (median brain SUVmean, 4.9 versus 5.7; p < 0.001).
In a multivariable analysis, brain SUVmean was an independent prognostic factor for OS (HR, 0.89), which was confirmed in the test set (p < 0.001), the researchers reported. In addition, a subgroup analysis based on treatment type found that brain SUVmean retained its prognostic significance in patients receiving chemotherapy, radiotherapy, and immunotherapy separately.
“Low brain metabolic activity was associated with increased mortality in patients with advanced NSCLC,” the group wrote.
Ultimately, the study supports recent research suggesting the existence of a “lung–brain axis,” indicating that diseases affecting the pulmonary system can lead to alterations in brain structure and function, the researchers noted.
“Further studies investigating the role of brain F-18 FDG uptake as a prognostic biomarker for OS and its association with systemic inflammation and the patient’s functional status are warranted,” the researchers concluded.
The full study is available here.