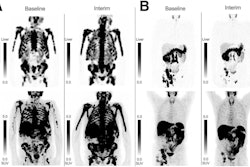
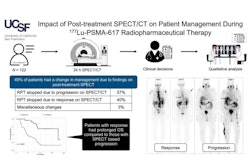
SPECT scans can provide early response information in prostate cancer patients treated with lutetium-177 (Lu-177) prostate-specific membrane antigen-617 (Lu-177 PSMA-617), researchers have reported.
The finding is from an analysis involving 192 patients with advanced disease treated in Seattle, WA, who had a SPECT scan performed 24 hours after starting cycle 1 of treatment, noted lead author Alireza Ghodsi, MD, of the University of Washington, and colleagues.
“As Lu-177 PSMA-617 is being used earlier in the treatment of [metastatic castration-resistant prostate cancer], accurate and early risk stratification is needed to guide treatment selection among available therapies,” the group wrote. The study was published March 12 in the Journal of Nuclear Medicine.
Radiopharmaceutical therapy with Lu-177 PSMA-617 (Pluvicto, Novartis) is effective for treating metastatic castration-resistant prostate cancer (mCRPC), yet patients respond differently to treatment, and reliable predictive biomarkers are needed to optimize patient management, the authors explained.
While studies suggest that post-treatment PSMA-SPECT is useful for early response monitoring after cycles 2 and 3 of the drug, its predictive value after cycle 1 is understudied, the group noted. To bridge the gap, the team analyzed data from 192 patients with mCRPC treated with Lu-177 PSMA-617 at the Fred Hutchinson Cancer Center between June 2022 and January 2025.
All patients had undergone a SPECT scan 24 hours after cycle 1, as well as a standard PSMA-PET scan prior to treatment. As of the last follow-up in March 2025, 109 of the patients (57%) had died, and 87 patients (45%) had achieved a decline of 50% or more from baseline in prostate-specific antigen (PSA) levels (PSA50).
The researchers first divided the group into four quartiles, with quartile 1 representing patients with the lowest uptake of Lu-177 PSMA-617 and quartile 4 the highest. Next, they analyzed associations between uptake (using SPECT mean standardized uptake values [SUVmean]) with PSA50, after controlling for PSMA-PET SUVmean and the time interval between the PET and SPECT scans.
According to the results, SPECT total tumor SUVmean measured after cycle 1 of Lu-177 PSMA-617 was associated with PSA50 independent of PSMA-PET SUVmean and the time interval between modalities, the researchers reported. Specifically, higher SPECT SUVmean quartiles were independently associated with greater odds of PSA50 response (odds ratios of 4.45, 10.2, and 17.1 for quartiles 2, 3, and 4.
“These findings support the role of cycle 1 PSMA-SPECT for early on-treatment risk stratification,” the group wrote.
The researchers noted limitations, namely that this was a single-center study, and that the metrics derived from it may not generalize because of technical variabilities, including differences in camera technology, imaging acquisition, and reconstruction parameters.
Nonetheless, “the development of models including pretreatment PSMA-PET and cycle 1 PSMA-SPECT is warranted for more accurate outcome prediction,” the group concluded.
The full study can be found here.