SAN DIEGO - Imagers from Indiana University are advocating the routine use of post-toilet imaging for the detection and grading of enteroceles, a common problem found in women who have undergone hysterectomy or bladder neck suspension.
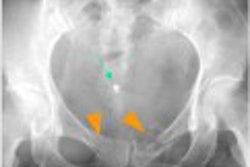
"An enterocele is a herniation of the small bowel into the posterior peritoneal cul-de-sac or into the vagina itself," wrote Dr. Fatima Kazem in a poster presentation at the American Roentgen Ray Society meeting. Kazem and her co-authors are from the Indiana University of School of Medicine and Methodist Hospital in Indianapolis.
Global imaging of the pelvic floor is needed because physical examination is so inaccurate for detecting enteroceles. Kazem’s group chose to work with dynamic cystoproctography (DCP), which is normally done post-evacuation with the patient on a radiographic commode.
However, the distension of the bladder and rectum in order to accommodate contrast administration can prevent the descent of the enteroceles because of limited pelvic space, the authors wrote. Instead, the group imaged the patients after they had used a regular toilet.
"(We found that) more effective emptying is usually achieved by evacuation in the privacy of the bathroom, and is then assessed on a post-toilet image with the patient straining maximally," they wrote.
In this retrospective study, 127 patients with enteroceles were referred to the imaging department by urologists and/or gynecologists. The patients underwent DCP according to the department’s standard protocol.
A preliminary radiograph (36 x 43 cm) was obtained to identify the pubococcygeal line (PCL). Fifty ml of contrast material was used to fill the bladder. The patients ingested 500 ml of barium suspension to opacify the small bowel. After the preliminary radiograph was obtained, the bladder was catheterized, and 50 ml of diatrizoate sodium (Hypaque 50%; Amersham Health, Princeton, NJ) was introduced.
Two lateral radiographs of the bladder were obtained, one at rest and the other on maximal strain. Bladder drainage was performed, the catheter was withdrawn, and the patient was asked to void.
The vagina was opacified with 20 ml of a mixture of barium and a vaginal gel (Acigel, Ortho Pharmaceutical, Raritan, NJ). A folded gauze square was inserted in the introitus to limit the loss of barium. The rectum was filled with 200 ml of a thick barium paste (Anatrast, Lafayette Pharmacal, Lafayette, IN). Lateral radiographs were obtained at rest, on squeeze, and during and after evacuation (American Journal of Roentgenology, January 2000, Vol. 174:1, pp.81-88).
"On reviewing the films, an enterocele was determined to be present if the small bowel extended below the PCL line," the poster presenters wrote. An enterocele was classified as small if it was up to 3 cm below the PCL; moderate if 3-6 cm below the PCL; and larger if more than 6 cm below.
According to the results, 11 patients had enteroceles that were detected only on post-toilet imaging. Of these 11, six were moderate in size and two were larger. Enteroceles showed an increase in size on post-toilet image in 62.2% of the 127 patients. A decrease in enterocele size was found in 21.7% and no change in 16.5%.
The mean depth of a small enterocele on the post-evacuation exam was 2.06 cm versus 4.38 cm on the post-toilet exam. For moderate-sized enteroceles, the mean depth was 4.56 cm on the post-evacuation exam and 5.25 on the post-toilet. Finally, for large enteroceles, the mean depth on post-evacuation x-ray was 8.20 compared to 8.46 on the post-toilet exam, the authors reported. Overall, 25.2% of the enteroceles were upgraded based on the post-toilet x-rays.
"Post-toilet imaging is intuitively more physiologic and encourages further rectal evacuation, which in turn permits further descent of the small bowel," the authors concluded.
Accurate preoperative detection of enteroceles can often change the course of surgical repair, the authors added, especially in the case of larger enteroceles, which can require a transabdominal versus transvaginal surgical approach.
By Shalmali Pal
AuntMinnie.com staff writer
May 9, 2003
Copyright © 2003 AuntMinnie.com