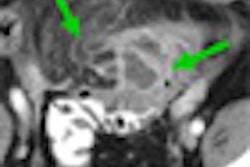
Evidence spanning decades shows that people with coronary artery calcium (CAC) scores of zero have a good chance of avoiding cardiac events. But the assurance applies only to asymptomatic patients. Newly emerging research finds that a zero CAC score combined with symptoms of coronary artery disease can mean trouble down the road. Some may be in the process of transitioning from CAC-negative to positive.
"We've heard of the warranty you have with a zero calcium score, but that's in somebody who doesn't have symptoms," said Dr. João Lima, a professor of medicine, radiology, and epidemiology at Johns Hopkins University in Baltimore. "If somebody presents with symptoms, the story is a little different, although we do need more data to be sure."
At Stanford University's 2009 International Symposium on Multidetector-Row CT, Lima unveiled new research on the prognosis of CAC-negative individuals with angina or other symptoms of coronary artery disease.
Massive MESA
The most ambitious study of atherosclerosis to date has been the Multi-Ethnic Study of Atherosclerosis (MESA), comprising 6,800 individuals (53% women, ages 45-84 years) in the U.S. with no history of heart disease. Patients were scanned with electron beam CT in six academic centers across the U.S. and followed over time, and more than 200 data analyses have been published from the massive database since 2005.
An analysis submitted for publication earlier this year examined individuals with cardiac events who had absent or minimal coronary artery calcifications. Dr. Matthew Budoff from the University of California, Los Angeles, along with Lima and colleagues, looked at data from 3,923 asymptomatic individuals free of known cardiovascular disease at baseline (mean age, 58 ± 9 years; 39% men) with CAC scores of zero to 10.
Overall, Lima said, 3,415 individuals had no detectable CAC, whereas 508 had CAC scores of one to 10.
Rescanned at the four-year mark, the researchers found that "if you had a real zero and you were symptomatic at MESA study entry, you really had a very low incidence of any events, but if your calcium score was between one and 10, then the hazard ratio jumped to three for heart events and for all events," Lima said.
Over a median 4.1 years of follow-up, the investigators logged 16 incident "hard" coronary heart disease (CHD) events and 28 total incident CHD events in individuals with absent or minimal CAC.
Results adjusted for age and gender showed that the minimal (but not zero) CAC level was associated with a threefold risk of a hard CHD event (hazard ratio [HR], 3.23; 95% confidence interval [CI]: 1.17-8.95) or of any coronary event (HR, 3.66; 95% CI: 1.71-7.85).
"Heart disease and smoking were the principal drivers of events in this low calcium score group -- and this is due to the fact that we defined calcium score from a threshold, so when you take 3,000 people with real zero and a lot of people who are about to convert, that's the about-to-convert [population] that we see in between one and 10," Lima said.
Former (HR, 3.57; CI: 1.08-11.77) or current smoking (HR, 4.93; CI: 1.20-20.30) habits and diabetes (HR, 3.09; CI: 1.07-8.93) were all significant risk factors for events in people with zero CAC, Lima added.
Individuals with minimal CAC scores are at very low risk of future cardiovascular events, the study found, but diabetes and smoking were strongly associated with adverse events. Moreover, individuals with minimal CAC (one to 10) are at significantly increased risk of incident CHD events relative to those with CAC scores of zero.
"We concluded that there is a jump between minimal calcium and zero calcium," Lima said. "If you have a positive calcium score, then Caucasians progress [in atherosclerotic disease] more than people from other ethnicities, and the most common progression is 10-99 [CAC] score units. Also in MESA ... there is a relationship between calcium score and events -- and that relationship is valid not only among Caucasians but also the three other ethnic groups."
The noncalcified culprit
In 2006, Hausleiter and colleagues took a different path to the question, examining the prevalence and characteristics of noncalcified plaque in 161 symptomatic individuals using 64-detector-row CT angiography (CTA) (Journal of the American College of Cardiology, July 2006, Vol. 18:2, pp. 312-318).
Patients were scanned using MDCT at 32 x 0.6-mm intervals. Significant disease couldn't be ruled out in 33% of the cohort; noncalcified plaque was present in 44% of the remaining patients. In 10% of the 63 patients with CAC scores of zero, noncalcified plaques were the only ones responsible for coronary artery disease, Lima said of the study.
"Hausleiter et al showed that 16% of 63 patients with calcium scores of zero had noncalcified plaques," Lima said. "None of this is surprising to us, but it's good to have in mind this excellent data when you go to symptomatic people from the [Coronary Artery Evaluation Using 64-Row Multidetector Computed Tomography Angiography (CORE) 64 trial]."
Zero calcium at MDCT
A new analysis of the CORE 64 data, submitted for publication this year by Gottlieb, Lima, and colleagues, analyzed conventional angiography data from a symptomatic subset of CORE 64's population with zero baseline CAC scores.
"Gottlieb took everybody who had calcium scores of zero and looked [for] obstructive disease. In that group, a very high percentage of CTAs were positive," Lima said.
The absence of calcium in the subgroup didn't preclude the presence of obstructive disease, Lima said. In fact, using a calcium score of zero to predict the absence of significant stenosis ≥ 50% was only 45% sensitive and 91% specific, with positive and negative predictive values of 68% and 81%, respectively.
Revascularization was performed in nine (12.5%) of the zero-calcium patients within 30 days. From a total of 383 vessels without any CAC, 47 (12%) presented with a ≥ 50% stenosis. From a total of 64 totally occluded vessels, 13 (20%) had no calcium.
The lack of calcium does not exclude obstructive disease or the need for revascularization, they concluded. Total coronary occlusion occurs frequently in the absence of any detectable calcification.
Symptomatics from MESA
In another study submitted for publication this year, one of the MESA investigators contacted 176 symptomatic people without CAC from the original study cohort and performed invasive angiography on them, Lima said.
"When you look at the arteries that had 50% stenosis [at angiography], several of those arteries had zero calcium at baseline -- and there was 75% stenosis in some arteries with a [baseline] calcium score of zero," he said.
Among the 176 patients who underwent angiography, Rosen and colleagues found ≥ 50% stenosis in the left anterior descending (16.6%), left circumflex (15.7%), right coronary (21.8%), and left main (35%) arteries. A smaller percentage of ≥ 75% stenoses was also found in the left anterior descending (12.7%), left circumflex (17.9%), and right coronary (21.8%) arteries.
This study found a close relationship between the CAC scores and the severity of coronary stenosis, and a considerable number of patients had zero calcium scores in the stenosed vessels, Lima said. Still, only 4% of these stenosed vessels were absolutely free of measured calcium (CAC = 0).
"The bottom line is that a calcium score of zero is a warranty of freedom of events if you're asymptomatic," Lima said. "But in the symptomatic patient, a calcium score of zero really doesn't preclude the performance of angiography or any other parameter or study that you think is clinically indicated."
By Eric Barnes
AuntMinnie.com staff writer
October 2, 2009
Related Reading
Coronary CTA beats calcium scoring for short-term prognosis, August 14, 2009
Coronary artery calcium independently predicts risk in CAD patients, July 29, 2009
Zero calcium means good outcomes, even with undetected plaques, July 23, 2009
CTA predicts coronary plaque instability, June 30, 2009
Absence of coronary calcium predicts excellent 10-year survival: study, June 18, 2009
Copyright © 2009 AuntMinnie.com