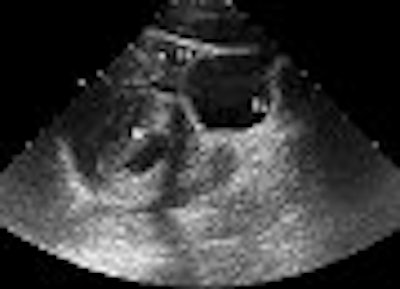
Ultrasound is credited with being able to rapidly and efficiently spot free fluid in blunt abdominal trauma cases. But does this hold true in pregnant patients? Yes and no, according to a study from the University of California, Davis.
Dr. John Richards and colleagues wanted to determine the accuracy of sonography for detecting blunt abdominal trauma in pregnant women, and compare those results to nonpregnant patients. They found that the modality had high specificity in both groups, but showed poor sensitivity among patients who were in a family way.
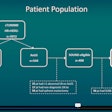
For this retrospective review, records from 2,319 patients were culled from an eight-year period. Out of this number, there were 328 pregnant women, 23 of whom had intra-abdominal injury. There were 208 nonpregnant patients with the same diagnosis.
All underwent focused abdominal ultrasound on an XP10-128 unit, an Acuson Sequoia GI unit (both Siemens Medical Solutions, Malvern, PA), or a 5200S unit (Acoustic Imaging, Phoenix). Phased-array or convex 2.5-5.0 MHz transducers were used. CT exams were also done.
The final ultrasound reports were reviewed for the presence and location of free fluid, as well as the presence of solid organ parenchymal abnormalities.
"Free fluid was assumed to represent hemoperitoneum, and irregularities within the parenchyma of solid organs or subcapsular collections of fluid were assumed to represent lacerations of hematomas," the authors wrote (Radiology, November 2004, Vol. 233:2, pp. 463-470).
According to the results, the sensitivity of ultrasound in pregnant patients was 61%. The specificity was 94.4%, and the accuracy was 92.1%. The most common injury was placental abruption, which required immediate delivery by cesarean section.
The exam's sensitivity was highest in patients who were in the first trimester of pregnancy, the authors said. This may be because of the expanding uterus, which compresses intra-abdominal structures and makes detecting free fluid more difficult.
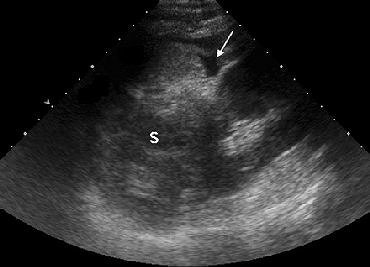 |
| A 22-year-old woman in the first trimester of pregnancy had sustained blunt abdominal trauma and subsequent splenic laceration in a motor vehicle collision. After US was performed, the patient was taken immediately to the operating room for laparotomy. Above, longitudinal US image of left upper quadrant reveals perisplenic free fluid (arrow) and abnormal-appearing splenic parenchyma (S). Below, longitudinal US image of pelvis shows free fluid (FF) superior to the bladder (BL) and gravid uterus (U). |
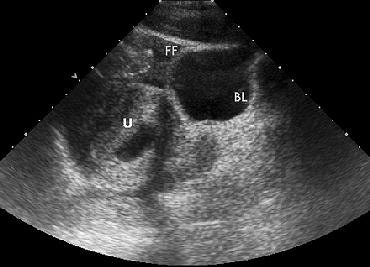 |
| Figure 3a-b, Richards JR, Ormsby EL, Romo MV, Gillen MA, McGahan JP, "Blunt Abdominal Injury in the Pregnant Patient: Detection with US" (Radiology, 2004; 233:463-470). |
In nonpregnant patients, ultrasound's sensitivity was 71.2%, specificity was 97.4%, and accuracy was 94.6%. The most common injury was to the liver in this group.
For all patients, ultrasound had a sensitivity of 70.1%, specificity of 96.9%, and accuracy of 94.3%. The most common finding of free fluid in the pregnant group was in the left and right upper quadrants and in the pelvis, the authors reported.
In the second group, Morison pouch free fluid accumulation was most often detected. In both groups, the most common false-positive finding was isolate pelvic free fluid, possibly because the exam is performed before hemoperitoneum has collected to a level of detection.
While ultrasound is faster in a triage situation than CT, the low sensitivity is still a sticking point. "In the future, US performed with contrast material may be a viable alternative to CT," Richards' group suggested.
Make that fairly far into the future, based on the results of a second ultrasound study in the American Journal of Roentgenology. Dr. Pierre-Alexandre Poletti and colleagues from the University Hospital of Geneva tested out contrast-enhanced sonography in blunt abdominal trauma and found that the modality came up short.
"Second-generation sonography contrast agents consist of stabilized microbubbles filled by an inert innocuous gas, and are characterized by outstanding stability and resistance to pressure that allow prolonged examination time after a single IV bolus," the group explained. "The goal of this study was to determine how the conspicuity of solid organ injuries can be improved by using a second-generation contrast medium," (AJR, November 2004, Vol. 183:5, pp. 1293-1301).
For this study, 210 consecutive, hemodynamically stable trauma patients underwent abdominal sonography and CT upon admission to the level 1 trauma center. Patients who had false-negative ultrasound results for solid organ injuries, in comparison to CT results, then underwent noncontrast sonography (referred to as control ultrasound in the study). If the injury was still undetectable on control ultrasound, the patient underwent contrast-enhanced sonography.
"If the contrast-enhanced sonography examination revealed injury that was not seen on both admission and control sonography, this injury was reclassified as a true-positive result," the authors stated.
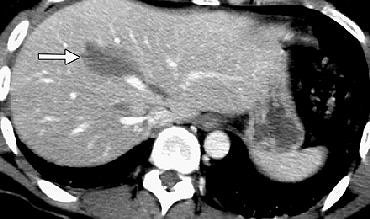 |
| Thirty-one-year-old man admitted one hour after motorbike accident. Admission sonogram (not shown) was normal. Axial CT image obtained at level of upper abdomen shows grade 3 liver injury (arrow). There is no associated free fluid. Poletti PA, Platon A, Becker CD, Mentha G, Vermeulen B, Ubhler LH, Terrier F, "Blunt Abdominal Trauma: Does the Use of a Second-Generation Sonographic Contrast Agent Help to Detect Solid Organ Injuries?" (AJR 2004; 183:1293-1301). |
Contrast ultrasound exams were performed on an HDI 5000 system (Philips Medical Systems, Andover, MA) in pulse inversion harmonic mode. The contrast agent (SonoVue, Bracco, Milan, Italy) was administered intravenously using a 20-gauge catheter. Serial images were obtained every three seconds from the beginning of the injection for the duration of three minutes.
According to the results, CT findings were positive for 88 solid organ injuries in 71 of the 210 patients. In comparison, the detection rate was 40% for admission ultrasound and 57% for control ultrasound. The detection rate improved to 80% when contrast sonography was used.
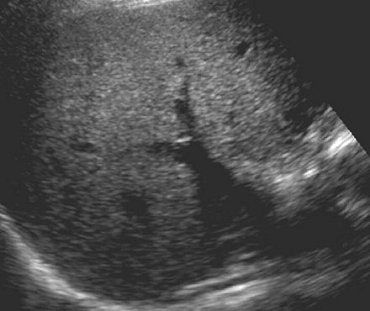 |
| Above, axial control sonogram obtained at level of injury does not show any parenchymal abnormality. Below, axial contrast-enhanced sonogram reveals liver injury as deep hypoechoic area (between arrows) surrounded by enhanced hyperechoic parenchyma. |
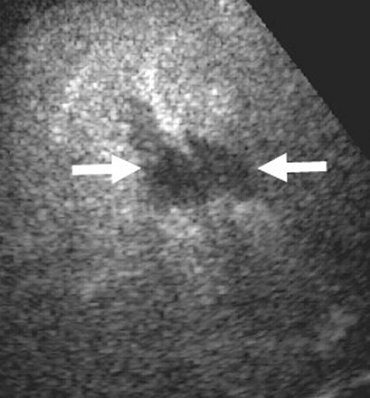 |
| Poletti PA, Platon A, Becker CD, Mentha G, Vermeulen B, Ubhler LH, Terrier F, "Blunt Abdominal Trauma: Does the Use of a Second-Generation Sonographic Contrast Agent Help to Detect Solid Organ Injuries?" (AJR 2004; 183:1293-1301). |
Broken down by specific condition, the sensitivity of admission sonography for nonfree fluid intra-abdominal injuries was 41%. The percentage jumped to 60% on control sonography, and climbed to 76% with contrast ultrasound.
Vascular injuries to the spleen and liver were easily depicted by contrast ultrasound, appearing as isolated hyperechoic foci within the first five minutes after injection.
While these findings were promising, contrast-enhanced ultrasound still missed 18% of all solid organ injuries, the authors reported. Specifically, contrast sonography missed major liver and spleen injuries: eight of 38 CT-proven liver injuries and seven splenic injuries. The modality also turned in false-negative results for kidney and adrenal injuries.
The authors concluded that contrast-enhanced sonography cannot replace CT in the triage of hemodynamically stable trauma patients who also have negative findings on traditional ultrasound. However, contrast ultrasound can serve as an alternative to CT for pseudoaneurysms.
By Shalmali Pal
AuntMinnie.com staff writer
December 15, 2004
Related Reading
SonoVue reinstated for echo use, November 1, 2004
Overexposed? CT in the emergency room, October 21, 2004
MRS predicts severity of brain injury in abused infants, June 10, 2004
Experience beats speed in emergency FAST training, June 2, 2004
Copyright © 2004 AuntMinnie.com