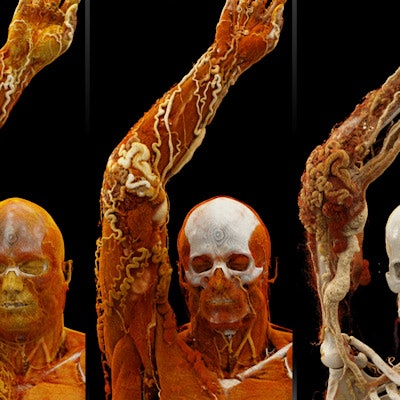
What is the clinical utility of cinematic rendering in musculoskeletal (MSK) CT? It enhances the visualization of soft-tissue injuries and fractures -- in turn improving trauma evaluation and preoperative planning, Dr. Savvas Nicolaou said in a presentation at the recent International Society for Computed Tomography (ISCT) meeting in San Diego.
"I believe cinematic rendering is still trying to find its niche and its role regarding how it affects clinical management and where we can utilize it from a clinical perspective," he told meeting attendees. Nicolaou is the director of emergency and trauma radiology at Vancouver General Hospital in British Columbia, Canada.
The photorealistic quality of cinematically rendered images can reveal details of injuries that might otherwise remain masked or at least difficult to see on conventional CT scans or 3D volume-rendered images, he noted. Therein lies potential for the advanced visualization technique to deliver value in trauma imaging.
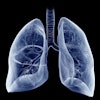
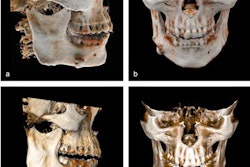
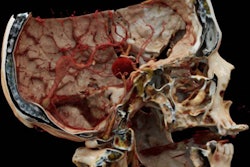
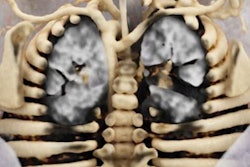
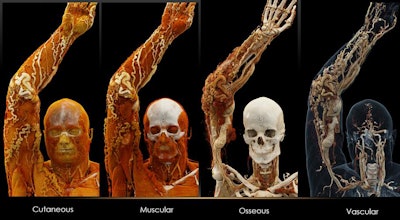 Cinematically rendered images based on patient CT scans viewed using different presets for skin, muscle, bone, and vasculature (from left to right). All images courtesy of Dr. Savvas Nicolaou.
Cinematically rendered images based on patient CT scans viewed using different presets for skin, muscle, bone, and vasculature (from left to right). All images courtesy of Dr. Savvas Nicolaou.Powerful display of injuries
Several recent studies have demonstrated the benefits of applying cinematic rendering to a variety of clinical scenarios, including evaluating maxillofacial CT and spleen pathology and diagnosing colitis.
What distinguished the technique from traditional volume rendering is that cinematic rendering employs a computational model that integrates light scattered from all possible directions. In addition, unlike the synthetic light sources used for traditional volume rendering, cinematic rendering relies on high dynamic range (HDR) lightmaps and camera properties to create a natural, realistic presentation of imaging datasets.
"Cinematic rendering definitely has enhanced delineation of anatomical structures due to its superior depth and shape perception, compared with traditional volume rendering," Nicolaou said.
Various institutions have begun to use these photorealistic images to teach anatomy and pathology to medical students, as well as to educate and communicate with patients regarding their medical conditions.
When it comes to trauma imaging, cinematic rendering is ideal for revealing subtle soft-tissue injuries and bone fractures that might be masked on CT scans or traditional volume-rendered images, he noted. The added depth perception of cinematically rendered images can also help clinicians better visualize the relationship between fractures and underlying vasculature, even in the presence of extensive metal artifacts such as bullets.
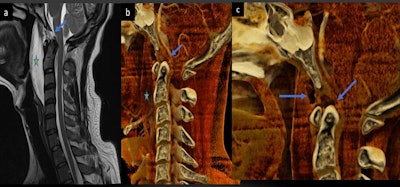 Comparable views of a ruptured tectorial and anterior atlanto-occipital membrane (arrow) seen on a spine MRI scan (a) and a cinematically rendered spine CT scan (b, c).
Comparable views of a ruptured tectorial and anterior atlanto-occipital membrane (arrow) seen on a spine MRI scan (a) and a cinematically rendered spine CT scan (b, c).Another distinct advantage of cinematic rendering is that it enables clinicians not only to view entire imaging datasets as a 3D model but also to see different types of tissue with minimal distraction from other tissues, he continued. Nicolaou and colleagues have used computer software to develop preset windows for cinematic rendering that allow them to examine skin, muscle, bone, and blood vessels almost in isolation.
"A lot of work went into the initial development of presets for different types of tissue," he said. "But once you have presets, you can see cinematically rendered images easily. We have used them for musculoskeletal malformations in cervical spine trauma and some musculoskeletal tumors."
Clinical examples
Though cinematic rendering is not being used on a routine basis just yet, Nicolaou presented several real-life clinical applications demonstrating the utility of the technique in trauma imaging at his institution:
- 28-year-old woman hit by train. Cinematically rendered images showed highly detailed multiple complex fracture dislocations in both of the patient's legs, with a degloving injury to the right foot. The advantage of having cinematic rendering for this case was that the radiologists were able to appreciate the complexity of the injury by quickly looking at the different tissue presets rather than scrolling through thousands of scans from the axial CT dataset.
- 24-year-old passenger in a motor vehicle accident. The patient presented with atlanto-occipital dissociation, initially measured as 12 mm on plain radiographs but later found to be 9.6 mm on cinematically rendered CT scans. Magnified views of the cinematically rendered images revealed the severity of a tear in the tectorial membrane and a disruption of the apical ligament, both of which were very difficult to appreciate on routine CT scans. The soft-tissue injuries were subsequently confirmed on MRI scans.
- 46-year-old with Parkes Weber syndrome. Nicolaou and colleagues presented cinematically rendered images based on the patient's CT scans to interventional radiologists for percutaneous treatment planning. By cycling through different tissue presets, the physicians were able to see the patient's arterial-venous malformation, tears, aneurysms, and even niduses clearly, which proved to be important from a treatment perspective.
"[Cinematic rendering] is clearly a very powerful technique that, in a matter of seconds, shows you the exact anatomic depiction ... of different types of tissue," he said. "Interventional radiologists see a lot of value in this regarding endovascular angioplasty when dealing with patients from a palliative perspective. Cinematic rendering also provides a vascular map for preoperative planning and reveals nicely how good the therapeutic response has been." - 50-year-old woman with metastatic ovarian carcinoma. The patient underwent cementoplasty, a minimally invasive procedure that, in this case, involved pouring cement into the weight-bearing portion of the iliac bone for structural support. Cinematic rendering images allowed the group to identify the location of the cement and distinguish it from sclerosis using different colors. This helped them confirm that the cement was appropriately situated after the procedure and not negatively affecting surrounding structures.
"I believe cinematic rendering techniques do have a role to play in appropriate clinical settings," Nicolaou said. They offer an opportunity for clinicians to visualize true-to-life, ultrahigh-definition, clinically applicable images, and have unprecedented potential to alter surgical management and improve outcomes in musculoskeletal imaging, he concluded.